Magnetoencephalography (MEG) is a noninvasive test that neurologists and neurosurgeons use to help plan brain surgeries for epilepsy and tumor removal. MEG maps out the sensory areas of your brain and can pinpoint the exact location where seizures originate.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
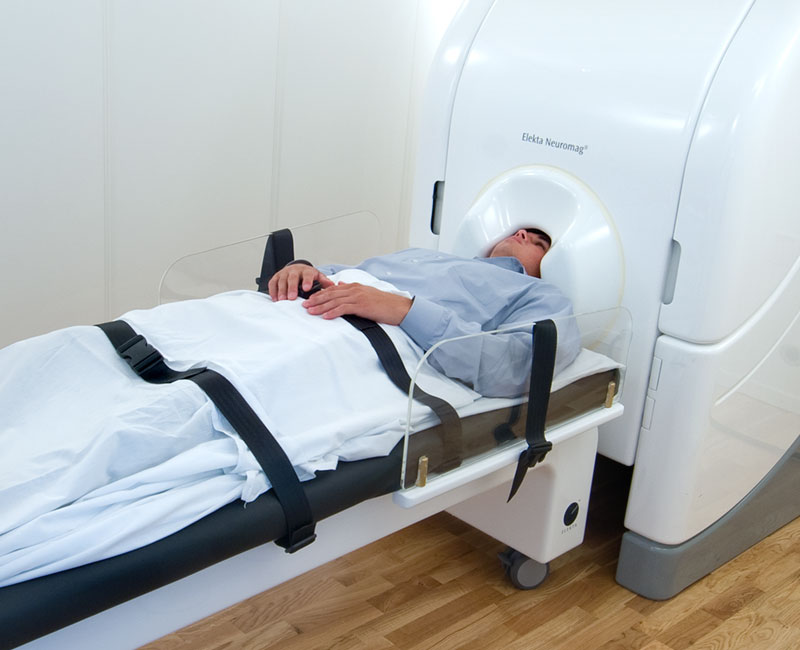
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17218-magnetoencephalography)
Magnetoencephalography (MEG) is a test that measures the magnetic fields your brain’s electrical currents produce. Healthcare providers use this test to map brain function and identify the exact location of the source of epilepsy-related seizures.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
MEG is noninvasive, which means the test happens on the outside of your body and it doesn’t hurt. There aren’t any needles or incisions involved, and you’re not exposed to radiation (X-rays).
MEG is currently the most advanced method of recording and evaluating your brain activity.
Neurologists and neurosurgeons use MEG for two purposes:
MEG is also an important part of neurological and psychiatric research to help scientists better understand human brain function.
Brain cells (neurons) interact with each other by generating tiny electrical voltages. The flow of electrical current produces a magnetic field. MEG detects, records and analyzes these magnetic fields using sensitive magnetic sensors. The strength of the magnetic field your brain produces is very small, so providers need highly specialized systems to pick up the signal.
Advertisement
These sensing systems consist of small, high-resolution coils, coupled to devices called SQUIDs (superconducting quantum interference devices). There are more than 300 of these sensors inside a helmet that fits over your head during this test.
The sensors in the helmet and specialized computer software work together to detect and record the activity of neurons as you lie still or complete a series of tasks, such as listening to sounds or looking at pictures. MEG records both normal and abnormal brain signals every millisecond. The magnetic fields show up on an anatomical image of your brain on a computer screen to “map out” where specific brain activities originate and when they activate.
Your healthcare provider will let you know if you need to stop eating or drinking before the test. They’ll also let you know if you need to make any changes to your medications or routine.
Don’t wear makeup or use any hair products on the day of the test. They can interfere with the testing.
You also won’t be able to wear any metal items in the exam room, such as jewelry, eyeglasses, hair pins, underwire bras and clothing with metal fixtures. A provider will give you a medical gown to wear if necessary.
If you have any medical devices in or on your body, you’ll need to let your provider know before the test. If they contain metal or anything that could interfere with the magnetic fields and you can’t remove them, you might not be able to have the test. These devices may include:
The process of a MEG test can vary depending on the reason for it. In general, you can expect:
Advertisement
You won’t feel any sensations from the MEG machine during the testing and it won’t hurt. There’s a two-way intercom and video monitoring system in the room, so you’ll be able to communicate with the provider performing the test at all times and vice versa.
Some providers perform an electroencephalogram (EEG) or a magnetic resonance imaging (MRI) scan alongside a MEG test. If this is the case, there will be additional steps to the process.
The MEG test takes about one to two hours to complete.
If you or your child had sedation or anesthesia for the test, a healthcare provider will observe you for 30 minutes to two hours after the exam to make sure you recover well. You’ll need someone else to drive you home.
If you didn’t have sedation, there’s no recovery period. You can return to your usual activities.
There aren’t any known risks of a MEG test.
It may take several days or even weeks for specialists to review the recordings of your MEG test. This is because providers use MEG tests to plan complex brain surgeries, and several specialists may work together to do so.
Once they’ve established a plan, your healthcare team will go over the results with you and discuss the next steps.
Brain MRI (magnetic resonance imaging) collects structural information and creates images of your brain using a large magnet and a computer. MEG records magnetic fields from neurons in your brain using hundreds of special sensors and a computer. The fields appear as brain waves.
Advertisement
Providers typically combine MRI with MEG to get what’s called magnetic source imaging (MSI). MSI creates functional maps of brain activity.
MEG is also different from functional MRI (fMRI). Functional MRI evaluates subtle regional blood flow changes in your brain that happen when you perform certain tasks. While both MEG and fMRI evaluate the function of your brain, MEG pinpoints more specific areas of activity, whereas fMRI shows general areas of activity. In addition, MEG is better at showing time-related (temporal) characteristics of brain activation than fMRI.
The first difference between these two diagnostic tests is that EEG (electroencephalography) records the electrical activity of your brain, and MEG records the magnetic fields of your brain (which come from the electrical activity).
Another difference is that MEG is much more sensitive and precise at recording brain activity than EEG. Your skull and cerebrospinal fluid (CSF) can distort the recording of electrical activity during an EEG. These tissues don’t distort magnetic fields. Because of this, MEG provides better “images,” or spatial resolution, of your brain and can specifically pinpoint areas of abnormal activity.
Advertisement
Healthcare providers sometimes perform an EEG at the same time as MEG to gather more information about where your brain activity is coming from.
Magnetoencephalography (MEG) is a very useful, noninvasive and safe test that healthcare providers use to map the sensory areas of your brain and to pinpoint the source of seizures. If you need a MEG test and are worried about the exam or have questions about it, don’t hesitate to ask your healthcare provider. They’re available to answer your questions and support you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Epilepsy and seizures can impact your life in challenging ways. Cleveland Clinic experts can help you manage them and find relief.
