Testicles, or testes, are the part of the male reproductive system that makes sperm and hormones. They’re located outside your body. Talk to your healthcare provider if your testicles change in some way.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
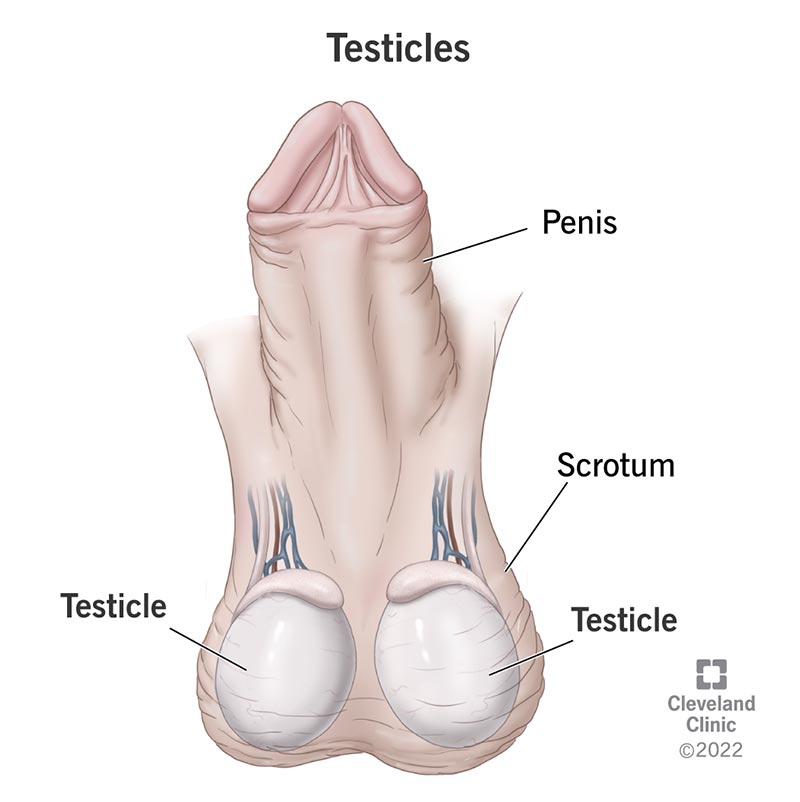
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23964-testicles)
A testicle (pronounced “teh-stuh-kl”) is part of the male anatomy. Generally, you’ll have two testicles. These body parts make sperm and hormones.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Other names for your testicles are male gonads or testes (pronounced “teh-steez”). One testicle is called a testis. There are other more casual names for testicles that you might hear or even use yourself, including “balls,” “nuts” and “cojones.”
The testicles make sperm and sex hormones, particularly testosterone.
Testicles are about two degrees Celsius lower in temperature than the rest of your body. Cooler temperatures are better for making sperm, a process called spermatogenesis. In each of the testes, the process happens in tubes called seminiferous tubules. There are a surprising number of tubes in each testis — about 700.
It takes about 74 days for sperm cells to mature. The immature cells get the blood and nutrients they need in the tubules. From there, they’re pushed along to the epididymis, another type of tube that runs along the back side of your testicle. The epididymis connects to the vas deferens, which is the tube that lets sperm leave your body through your penis.
The testes make hormones like testosterone in the Leydig cells. Testosterone is a hormone that causes people to have deeper voices, stronger muscles and body hair. The testes also make these other hormones:
Advertisement
Your testicles are located underneath your penis. They’re enclosed in a pouch of skin called the scrotum. Generally, you’ll have one testicle to the right and one testicle to the left of your penis.
Your testicles are connected to the inside of your body by a cord called the spermatic cord. Each cord contains nerves and blood vessels. The cords also contain the vas deferens, which are the tubes that move sperm to your penis, so it can leave your body in semen.
Your testicles aren’t visible because they’re located inside your scrotum. However, their outlines are visible, and you can feel them. Testicles have been described as being like large olives, small eggs or walnuts.
There’s no exact size for testicles. In fact, one of your testicles may be a little bit bigger than the other one. One testicle might be a little lower than the other. An adult testicle may range from half an inch (15 mL) to 1.5 inches (35 mL) or more. One comparison says the normal range goes from the size of a bird egg to the size of a small chicken egg.
Many testicle-related diseases are found in children, but not all. Here are some conditions that could affect your testicles:
Your testicles can be damaged by physical trauma, including motor vehicle accidents, falls or fights.
Contact your healthcare provider if you develop these signs or symptoms:
Your healthcare provider will begin by going over your medical history and your current symptoms. The tests they order will depend on what they think they’ll find. You may have:
Your healthcare provider will treat testicular disorders with a variety of therapies. Depending on the testicular disorder, treatments may include:
Advertisement
Here are some tips to keep your testicles healthy:
One testicle can produce enough sperm to get another person pregnant. If your healthcare provider must remove both testicles because you have cancer or an injury, you may be able to bank frozen sperm that could be used to impregnate a partner.
Your testicles are important parts of your anatomy. They’re related to your sexuality and your ability to reproduce. You should become familiar with how they feel and look when they’re healthy. Pay attention to any change. Contact your healthcare provider if you notice any lumps or other changes.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
