Orchiopexy is surgery to treat undescended testicles. A surgeon performs it when your baby is between six and 24 months old if their testicles haven’t moved into their scrotum yet. It also treats testicular torsion (where your testicle twists and cuts off the blood supply).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
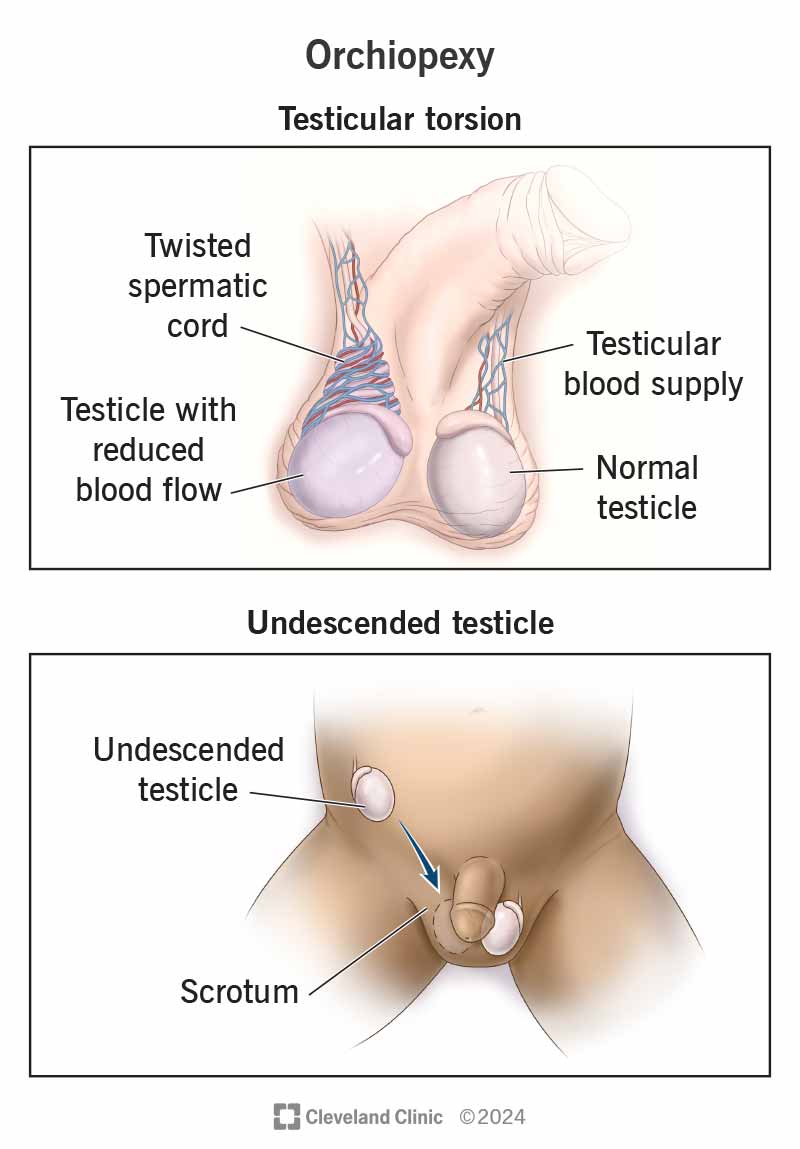
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/orchipexy)
An orchiopexy (OR-kee-oh-peck-see) is surgery to move undescended testicles or to treat testicular torsion. To treat undescended testicles, a surgeon moves them from inside your child’s belly (abdomen) or groin area and attaches them inside the scrotum (the pouch of skin below your penis). To fix testicular torsion, your provider will untwist your testicle and secure it to the inside of your scrotum.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The surgeon may also need to repair hernias or put in an artificial testicle (testicular prosthesis) during surgery.
Other names for an orchiopexy are orchidopexy (OR-keh-doh-peck-see) and undescended testicle repair surgery.
An orchiopexy corrects two conditions:
If your child’s testicles don’t descend on their own by the time they’re about 6 months old, healthcare providers recommend orchiopexy between 6 and 24 months of age.
Providers treat testicular torsion immediately. If blood flow doesn’t return to your testicle within six hours, they may have to surgically remove it.
Your child’s provider will give you instructions on how to prepare for an orchiopexy. Following their directions closely can reduce the risk of complications. You may need to:
Advertisement
It’s OK for your child to take daily medications the day of the procedure unless their provider says otherwise.
Tell your healthcare provider about any prescription or over-the-counter medications your child is taking, including herbal supplements. Aspirin, anti-inflammatory drugs and certain herbal supplements can increase the risk of bleeding.
If you have testicular torsion, you’ll have surgery right away and may not have time to prepare. Remember to tell your provider about all medications you’re taking.
If your child is having an orchiopexy, a team of healthcare providers who specialize in taking care of kids will perform it. This includes:
During an orchiopexy for undescended testicles, your child’s providers will:
If you have testicular torsion, your surgeon will:
An orchiopexy takes about an hour in most cases.
After orchiopexy, providers will move you or your child to a recovery room. Healthcare providers will monitor you or your child until it’s safe to go home (usually about two hours after the procedure is complete). Orchiopexy is an outpatient procedure. So most of the time, you don’t have to stay at the hospital overnight.
Advantages of orchiopexy include:
Advertisement
All surgical procedures carry some risk. Risks of an orchiopexy include:
Rarely, your testicle may move back up and out of your scrotum (reascending testicle). You’ll need additional surgery for a reascending testicle if that happens.
If you’ve had an orchiopexy, you’ll probably have pain or discomfort for a few days to a week. The stitches should dissolve in about two weeks.
People also often feel tired after an orchiopexy. Your child may sleep more for a few days afterward. They may feel nauseous or vomit for about a day from the anesthesia.
Most adults and kids older than a year can resume normal activities about two or three days after an orchiopexy. But someone who’s had an orchiopexy shouldn’t participate in sports or rough physical activity for at least two weeks. These activities may include tumbling, jumping, sprinting and straddling toys (rocking horse, seesaw, swing and bicycle or tricycle). Always ask your child’s provider whether it’s OK for them to return to these types of activities and any sports or exercise.
It’s important to remember that your child’s body is unique, so recovery times may vary. Follow your healthcare provider’s instructions on managing your child’s pain and discomfort.
Advertisement
Your child’s healthcare provider will give you instructions on what to expect, how to manage pain and how to care for the incision site after an orchiopexy. They may recommend:
Ask your provider when you can wash your child in a bathtub or shower. Sometimes, you can bathe the next day, or they might recommend waiting a week.
These are good guidelines to follow if you’ve had orchiopexy for testicular torsion, too. You also shouldn’t drive for a week or two after orchiopexy. Ask your provider when it’s OK to have sex.
Most children can go back to school or daycare three to five days after an orchiopexy.
Advertisement
Schedule a follow-up appointment with your pediatrician or surgeon two weeks after an orchiopexy. You may need to schedule another follow-up two to three months later.
Call your healthcare provider right away for any of these symptoms:
Any kind of surgery — especially for your child — can be scary. It may be comforting to know that an orchiopexy is a short, safe procedure that commonly has good results. If your child has an orchiopexy, they may sleep more than usual, but they should be back to many of their regular activities within a few days. Talk to your healthcare provider about your questions and concerns.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your urinary system, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
