Ringworm is an itchy, contagious fungal infection that causes a ring-shaped pattern on your skin. Over-the-counter and prescription treatments can stop the fungus from spreading to other parts of your body or to others.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
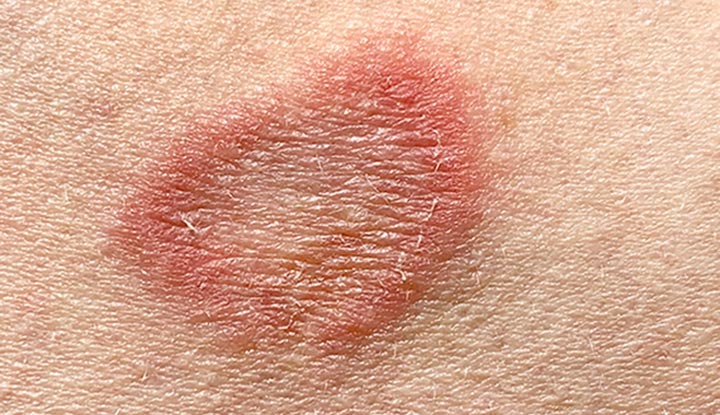
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4560-ringworm)
You might be surprised to learn that a fungus — and not a worm — causes ringworm. Fungi thrive in warm and humid areas such as locker rooms and public showers. This common and contagious skin infection gets its name from the red, itchy, ring-shaped skin plaque (a type of scaly rash). It spreads easily and through close contact.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You get ringworm from contact with an infected person, animal or object. Ringworm goes by different names depending on which body part it affects. Ringworm on your body is called tinea corporis. This type of ringworm affects your arms, legs, torso and face. Ringworm is treated with antifungal medication available either over the counter or as a prescription.
Ringworm has different names based on where it appears on your body — and it can appear just about anywhere. Ringworm infections include:
Advertisement
Ringworm typically begins as a flat, discolored patch, which may appear red in lighter complexions and brown in darker complexions. The patch has a ring-like or circular shape with a raised, scaly border.
Ringworm affects people of all ages. You’re more at risk for ringworm if you:
Ringworm is contagious and extremely common. It can affect 20% to 25% of the world’s population at any given time.
Signs typically appear between four and 14 days after your skin comes in contact with the fungi that cause ringworm, including:
Despite its name, a fungus causes ringworm. This type of fungus naturally lives on your skin, hair and nails. However, when their environment gets hot and damp, the fungi start growing uncontrollably. You can get this infection anytime your skin comes into contact with the ringworm fungus on someone else’s skin.
Ringworm is contagious. It can live on your skin, on surfaces and in soil. The main ways ringworm spreads are:
Your healthcare provider can diagnose ringworm by looking at your skin and assessing your symptoms. They may scrape the area to look at the skin cells under a microscope, too. Examining the scales typically confirms ringworm.
Several nonprescription (over-the-counter) and prescription antifungal medications are available to treat ringworm. Antifungals come in various forms like creams, gels or powders. Your healthcare provider can treat more widespread ringworm with oral antifungal medication.
Over-the-counter (OTC) antifungal creams, gels or powders typically work well. OTC products include:
If your symptoms get worse or don’t clear after two weeks, you may need an oral prescription medication from your healthcare provider.
Advertisement
Your healthcare provider may write you a prescription for oral antifungal medication if you have ringworm on your scalp or on many parts of your body. Most medications are prescribed for between one and three months. Oral antifungal medications include:
Antifungal shampoo, such as ketoconazole shampoo (Nizoral A-D®), may stop scalp ringworm from spreading. It won’t cure it, but it may help contain the infection. You also need to take a prescribed oral antifungal medication. Unaffected family members may benefit from using the shampoo as well.
Home remedies like apple cider vinegar or tea tree have little to no benefit. Apple cider vinegar may cause open sores or inflammation. Tea tree oil has antifungal and antimicrobial properties but its effects aren’t well-known.
Your home may require treatment as well. The ringworm fungus can live on surfaces for months. Disinfectant sprays like Lysol® or bleach can remove the fungus. Wash clothes, sheets and towels in hot water and detergent to prevent ringworm from spreading.
Corticosteroid creams may help reduce inflammation, but they shouldn’t be used to treat ringworm. In fact, they may worsen the infection.
Advertisement
Mild cases of ringworm clear up within a few weeks. More serious infections may require treatment for six to 12 weeks.
Some other things you can do to promote healing:
Although ringworm can go away by itself, it’s not common. While ringworm is present on your skin, you’re still contagious to others.
Yes, ringworm can come back. Ringworm will go away if you treat it appropriately. Follow your healthcare provider’s treatment plan until the infection clears completely. If you stop treatment or treatment ends too soon, the infection can come back.
If you suspect you or your child has ringworm, don’t use anti-itch creams containing corticosteroids. These creams weaken your skin’s defenses. They can allow the infection to spread and cover larger sections of skin. On rare occasions, the ringworm fungus goes deeper into your skin, making it even harder to treat.
Scalp ringworm can lead to a painful inflammation called kerion. With kerion, you may develop crusty, pus-filled sores, often with hair loss and scarring.
Advertisement
Ringworm thrives in damp, warm areas. The fungus can live on towels, clothes, sheets and household surfaces for months. Preventing ringworm involves:
A weak immune system or living in a damp, warm climate increases your risk of a fungal infection.
Call your healthcare provider if the ringworm infection:
You’re sure to have questions if you or your child develop ringworm. You might ask your healthcare provider:
No, ringworm isn’t a worm. It’s a fungal infection that gets its name from its ring-like border.
Ringworm fungus won’t affect your pregnancy. Still, you should check with your healthcare provider before using over-the-counter antifungal creams or powders. Oral antifungal medications appear to be safe to take during pregnancy. Your pregnancy care provider can discuss potential risks and benefits with you.
Yes, you can get ringworm from dogs, cats and other animals like cows, goats or horses. You can protect yourself by always washing your hands after playing with or petting animals. If your pet has ringworm, disinfect your pet’s bedding and take extra care to clean surfaces your pet has visited in your home.
Eczema and many other skin conditions can resemble ringworm. Both ringworm and eczema cause itchy, red skin. Unlike ringworm, eczema isn’t contagious and doesn’t spread from one area to another on your body. Ringworm has a unique, ring-like appearance. Contact a healthcare provider for an appropriate diagnosis.
Ringworm can be unpleasant, but antifungal medications will help you get rid of the fungus that causes ringworm. The treatment may take time, but it’s important to follow your healthcare provider’s treatment plan for as long as recommended. Ending treatment too soon can cause ringworm to return and make the infection harder to treat. Ask your provider about how you can keep ringworm from spreading to other parts of your body and to other people.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
