Athlete’s foot is a contagious fungal infection that causes different itchy skin issues on your feet. An itchy, stinging, burning rash forms on infected skin. Athlete’s foot treatment can stop the fungus from spreading and clear it up.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
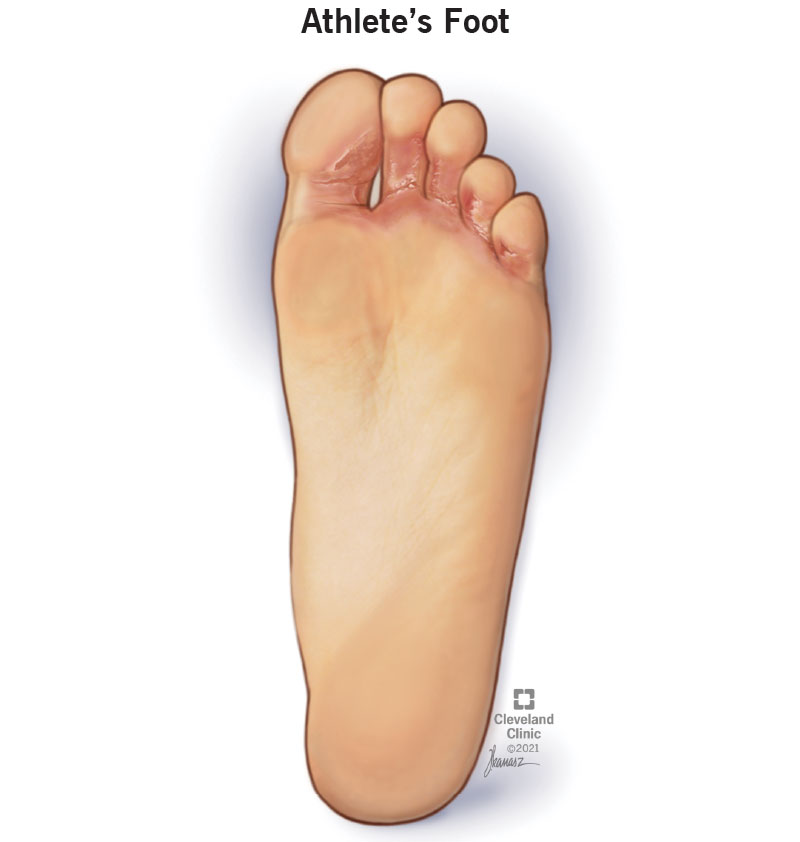
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22139-athletes-foot)
Athlete’s foot is a common fungal infection (caused by a fungus). Athlete’s foot causes an itchy, stinging, burning rash on the skin on one or both of your feet. Athlete’s foot is most common between your toes, but it can also affect the tops of your feet, the soles of your feet and your heels. Your skin may become scaly and cracked or develop blisters. Sometimes, your feet smell bad.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Athlete’s foot is a form of ringworm. “Tinea pedis” is another name for athlete’s foot. “Tinea” is another name for ringworm, and “pedis” means foot or feet.
Athlete’s foot can affect the skin between your toes, the bottoms of your feet, the tops of your feet, the edges of your feet and your heels. Your skin may appear irritated (red, purple, gray or white), scaly or flaky.
Athlete’s foot affects everyone. But it's most common in males and people over the age of 60. You may be more likely to develop athlete’s foot if you have:
Athlete’s foot is common. Estimates suggest that 3% to 15% of the population has athlete’s foot, and 70% of the population will have athlete’s point at some time in their lives.
Symptoms of athlete’s foot include:
Your symptoms depend on the type of athlete’s foot that you have.
Advertisement
Several different species of fungi cause athlete’s foot.
It commonly spreads through skin-to-skin contact or contact with a flake of skin. It spreads in areas used by large groups of people, like locker rooms, swimming pools and saunas.
It can also spread through contact with an infected surface. You can get athlete’s foot by sharing towels, socks or shoes with someone who has athlete’s foot.
Athlete’s foot is contagious. It’s a fungus that grows on or in your skin. Fungi (plural form of fungus) need warm temperatures and moisture to grow. People often wear socks and tight shoes every day, which keep their feet warm and moist. This is the perfect environment for athlete’s foot to grow.
Your healthcare provider can typically diagnose athlete’s foot by examining your feet and symptoms.
In some cases, your healthcare provider may remove a small piece of skin (biopsy) and test it in a lab. Several drops of a potassium hydroxide (KOH) solution dissolve the skin cells so only fungal cells are visible.
Over-the-counter (OTC) and prescription antifungal creams, ointments, gels, sprays or powders effectively treat athlete’s foot. These products contain clotrimazole, miconazole, tolnaftate or terbinafine.
Some prescription antifungal medications for athlete’s foot are pills. These pills contain fluconazole, itraconazole or terbinafine.
It’s important to finish your full course of medicine. If you stop too soon, your athlete’s foot may come back and be harder to treat.
Keep your feet dry, clean and cool. If possible, don’t wear socks or shoes. Avoid scratching your feet. Scratching your feet may cause the fungus to spread to other parts of your body.
With proper diagnosis and treatment, your athlete’s foot should go away in one to eight weeks. Follow your healthcare provider’s instructions.
It’s important to finish your full course of medicine. During the early healing stages, itchiness and irritation will fade. Even if your symptoms go away, you may still have athlete’s foot. If you don’t finish your full course of medicine, your athlete’s foot can come back and be harder to treat.
Athlete’s foot can spread across the bottom of your foot. This is moccasin athlete’s foot. In feet with moccasin athlete’s foot, the skin on the bottoms, heels and edges of your feet are dry, itchy and scaly.
In severe cases of athlete’s foot, you may develop fluid-filled blisters or open sores. Blisters often appear on the bottoms of your feet, but they may develop anywhere on your feet. Open sores often appear between your toes, but they may appear on the bottoms of your feet. Your feet may also smell bad.
Advertisement
Athlete’s foot doesn’t typically go away on its own. If it’s left untreated, it can spread to other areas of your body, including your:
With proper treatment, the outlook for people with athlete’s foot is good. Be sure to follow your healthcare provider’s instructions so you get rid of your athlete’s foot quickly and don’t pass it on to anyone else.
There are many ways to reduce your risk of getting athlete’s foot:
Advertisement
Call your healthcare provider if your athlete’s foot:
Athlete’s foot is an unpleasant condition. It’s itchy and annoying. It can also sting or burn and smell bad. However, antifungal medications or home remedies will help you get rid of athlete’s foot. Remember, you shouldn’t scratch your athlete’s foot, as it can spread to other parts of your body. It’s important to follow your healthcare provider’s treatment plan. If you don’t finish your full course of medicine, athlete’s foot can come back. Ask your healthcare provider how you can keep athlete’s foot from spreading to other parts of your body or other people.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
