Tinea manuum is a fungal infection that affects the outer layer of skin on one or both of your hands. Symptoms of tinea manuum include itchy, round patches on the back of your hands and dry, thickened skin on your palms. Treatment for a tinea manuum infection involves the use of a topical antifungal medication.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
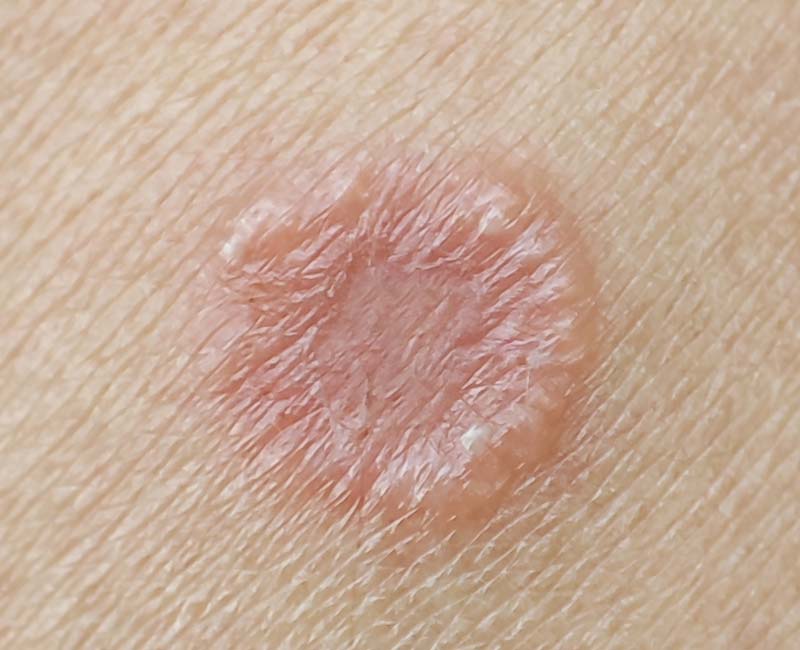
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24063-tinea-mannum)
Tinea manuum is a fungal infection that affects one or both of your hands. The infection affects the outer layer of your skin. Another name for tinea is ringworm. The names of the different types of ringworm refer to the location of the infection on your body. Tinea manuum affects:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Tinea manuum commonly occurs with athlete’s foot (tinea pedis). But it can affect your hands alone.
Despite its name, a worm doesn’t cause ringworm. The name comes from the appearance of the rash you may see. The rash has a ring- or circular-shaped pattern. The rash often has a raised, scaly border that wraps around like a worm.
Tinea manuum can affect anyone. But it most commonly affects male adolescents and adults.
Fungal infections affect up to 25% of the world’s population. Tinea manuum and tinea pedis are the fungal infections diagnosed most often. Depending on geographic location, tinea manuum is the diagnosis in up to 13% of fungal infections.
While tinea manuum can occur in both hands, more often it only affects one hand (tinea manus). “Two feet, one hand syndrome” is the informal name of the most common diagnosis of tinea on your hands and feet. This means tinea pedis affects both feet and tinea manus affects one hand. This condition occurs in 65% of cases. Fungal infections on both hands and feet occur in about 20% of cases. Tinea manus on one hand occurs in almost 12% of cases. Tinea manuum on both hands occurs in about 4% of cases.
Advertisement
The most common symptoms of tinea manuum are itchy, round patches on the back of your hands. On lighter skin, the patches may appear red or pink. On darker skin, the patches may look brown or gray. The patches may develop into a series of rings or circles with central clearings. The rings may have raised, scaly borders.
The skin on the palm of your hands may thicken. You may have intensely dry skin. You may notice deep cracks on your palms. Within the cracks, you may see white scaling. Your palms may or may not itch. You may have pain and swelling.
On the skin around your fingers, you may notice red patches with blisters and pimples. Frequently, the infection will spread to the fingernails of your affected hand.
A type of fungus causes tinea manuum. Fungi thrive in warm, humid environments. It commonly grows in tropical places. Moist areas such as locker rooms and public showers also harbor fungi.
Tinea manuum also spreads very easily. You can get tinea manuum from coming into contact with infected people, animals and soil. You can also get tinea manuum by using objects and touching surfaces that harbor the fungus. Tinea manuum can live for a long time on infected objects and surfaces.
Many people develop athlete’s foot (tinea pedis) before tinea manuum. Because the fungus is so spreadable, you can transfer the infection from your feet to your hands after scratching your feet.
Tinea manuum grow and thrive in moist, warm environments. The most common risk factors include:
Tinea manuum commonly affects people who work with their hands. This includes:
Tinea manuum has several other risk factors. These risk factors include:
Advertisement
Tinea manuum is extremely contagious. It spreads primarily through one of three ways.
You can get tinea manuum after coming into direct bodily contact with someone who has the infection. The person may or may not have symptoms. But if they’re a carrier of the infection, they can spread it.
You can get tinea manuum after touching an animal that has the infection. Many different animals can spread tinea manuum. This includes pets such as dogs and cats (specifically puppies and kittens). It also includes farm animals such as cows, horses, pigs and goats.
Fomites are objects or materials that are likely to carry an infection. You can get tinea manuum through indirect contact with fomites by sharing clothes, towels and bedding. The fungus can also live on hard surfaces in moist environments. This includes places such as locker rooms and public showers.
The fungus can also spread by touching soil and other objects in the environment infected by it. Tinea manuum can also spread from one part of your body to another.
Your healthcare provider will ask you about your symptoms and perform a physical examination. They’ll look at your palms, the back of your hands and your fingers. Your provider may also look at your feet. This is because many people with tinea manuum also have tinea pedis.
Advertisement
Your provider may want to collect a sample of the infected area. They may want to order other tests to confirm a tinea manuum diagnosis.
To confirm a tinea manuum diagnosis, your healthcare provider may order a test.
Your healthcare provider will gently scrape some of the skin from the infected area of your hand. In a lab, a technician will place the scrapings onto a microscope slide. The slide contains a drop of potassium hydroxide (KOH). They’ll look at the sample under a microscope. The KOH stain makes it easier for the technician to see if there’s a fungus present. The results are generally back within 24 hours.
If the KOH stain doesn’t provide accurate results, your healthcare provider may order a culture. A culture is a substance that allows fungi to grow. The technician can then identify the fungus causing your infection. A culture is more accurate and specific than a KOH stain, but it can take several weeks to get the results.
Your healthcare provider may use dermoscopy to confirm the presence of a fungal infection on your hand. They’ll use a handheld instrument called a dermoscope. The dermoscope has a magnifying lens and a lighting system. It can see details that aren’t visible to the naked eye. The dermoscope can often see white scales in the cracks of your palms if you have tinea manuum.
Advertisement
Your healthcare provider will recommend treating tinea manuum with an antifungal medication. You can typically treat a tinea manuum infection at home with an over-the-counter medication. You’ll apply the antifungal cream directly onto the infected area of your skin once or twice a day for up to six weeks. Topical antifungal medications include miconazole (Monistat 7®) and clotrimazole (Lotrimin®).
In some cases, your healthcare provider may recommend an antifungal medication taken by mouth. If your infection involves your nails or an extensive area of your body, you’ll need an oral medication. You may also need an oral medication if:
Oral medications include terbinafine (Lamisil®) and itraconazole (ONMEL®).
Tinea manuum infections cause dry, itchy skin on your hands. You may be able to treat the infection at home with an over-the-counter antifungal medication. But tinea manuum can be hard to treat. It’s important to use an antifungal medication the same way you’d use an antibiotic — you need to finish the treatment. The rash may look like it’s going away, but if you don’t complete the treatment, it will continue to come back.
You should call your healthcare provider if the infection persists. They’ll be able to properly diagnose your condition and recommend the appropriate treatment. You may need a prescription antifungal medication if the infection doesn’t go away. It can take some time, but tinea manuum infections do eventually clear up.
Fungal infections can be difficult to treat. It’s important you use any antifungal medication as directed. Your infection may look like it’s going away or even gone, but it will come back if the infection isn’t treated completely. You may need to use an antifungal medication consistently for up to six weeks, depending on the package directions. See your healthcare provider if your infection hasn’t cleared up within six weeks.
There are many steps you can take to prevent tinea manuum. These steps include:
Tinea manuum infections can be itchy and uncomfortable. With the help of an antifungal, you may be able to treat the infection at home. But it can take some time. It’s important to follow the package directions and complete the treatment. It can take up to six weeks for a fungal infection to clear. If you’re having trouble treating the infection on your own, reach out to your healthcare provider. They’re there to help you. You don’t have to suffer through the pain and itchiness.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
