Dialysis is a treatment for people whose kidneys are failing. There are two types of dialysis: hemodialysis and peritoneal dialysis. Both types perform the normal duties of your failing kidneys by filtering waste and excess fluid from your blood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
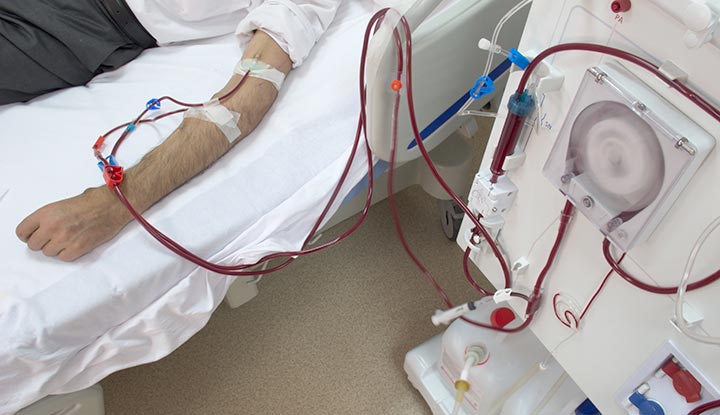
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/dialysis)
Dialysis is a treatment for people whose kidneys aren’t working. When you have kidney failure, your kidneys don’t filter blood the way they should. As a result, wastes and toxins build up in your bloodstream. Common wastes include nitrogen waste (urea), muscle waste (creatinine) and acids. They usually leave your body when you pee. Dialysis does the work of your kidneys by removing waste products and excess fluids from your blood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
People who have late-stage kidney disease, end-stage kidney disease (ESKD) or kidney failure may need kidney dialysis. The following diseases and conditions can damage your kidneys, leading to kidney disease:
Some people develop kidney problems for unknown reasons. Kidney failure can be a long-term condition, or it can come on suddenly (acute) after a severe illness or injury. Acute kidney failure may recover.
There are five stages of kidney disease. In stage 5 kidney disease, healthcare providers consider you to be in kidney failure. At this point, your kidneys only function at less than 15% of their normal rate. You may need dialysis or a kidney transplant to stay alive. Some people undergo dialysis while waiting for a transplant.
Yes, going on dialysis is serious. If you need dialysis and choose not to start or decide to stop, toxins will build up in your blood (uremia). Kidney failure is fatal without treatment. If you have kidney failure, you may survive a few days or weeks without dialysis.
Dialysis is common. Over 2 million people throughout the world treat kidney disease with dialysis or a kidney transplant.
There are two types of dialysis:
Advertisement
Hemodialysis is the most common type of dialysis. It utilizes a dialysis machine that:
You can get hemodialysis from a dialysis center or at home. Most people receive in-center hemodialysis at least three times per week. Depending on the type of at-home hemodialysis, you may need it three to seven days per week, and sessions may last between three and eight hours.
Before you start hemodialysis, a surgeon will enlarge some of the blood vessels (an artery and vein) in your arm to make dialysis access easier, as well as to allow blood to flow in and out of your body faster.
Peritoneal dialysis uses the inner lining of your abdomen (peritoneum) to filter your blood. You add a dialysis solution (dialysate) into your peritoneum that helps the blood vessels in the area filter your blood. Afterward, you drain the solution into a bag outside of your body. Healthcare providers call this process an exchange.
There are two main types of peritoneal dialysis:
Before you start peritoneal dialysis, a provider will surgically insert a permanent soft tube (catheter) into your abdomen. They’ll teach you how to add the dialysate and later drain the solution through the catheter.
It depends on the type of dialysis.
In-center hemodialysis takes about three to four hours to complete, and you’ll likely need it at least three times per week. Depending on the type of at-home hemodialysis, you may need it three to seven days per week, and sessions may last between three and eight hours.
Continuous ambulatory peritoneal dialysis usually takes about 40 minutes, and you’ll likely need three to five sessions each day. Automated peritoneal dialysis may take eight to 12 hours, and you may need to do it every day.
The primary benefit of dialysis is that it treats kidney failure by filtering waste products and excess fluid from your blood. Without dialysis — or a kidney transplant — kidney failure is fatal.
Both types of dialysis have distinct benefits. Talk to a healthcare provider — they can review both types of dialysis with you and recommend one that’s best for you and your lifestyle.
Dialysis can’t cure end-stage kidney disease or kidney failure. Unless you get a kidney transplant, you’ll need dialysis for the rest of your life.
Advertisement
Both types of dialysis have risks. They both increase your risk of infection.
Hemodialysis may eventually lead to poor blood flow or a blockage from scar tissue or a blood clot. Rarely, the dialysis needle may come out of your arm, or a tube may dislodge from the machine. But a detection system will temporarily shut down the machine and alert medical staff to protect you from blood loss.
Peritoneal dialysis increases your risk of peritoneum inflammation (peritonitis). Over time, it can weaken your abdominal muscles and increase your risk of developing a hernia.
Talk to a healthcare provider about the complete list of risks or complications for each type of dialysis.
You may feel a slight pinch during hemodialysis when a healthcare provider inserts a needle. But the process isn’t painful.
Peritoneal dialysis isn’t painful. But the dialysate in your abdomen can make you feel bloated, cold and uncomfortable.
Life expectancy varies from person to person, with some people living for many years on dialysis. Your outlook depends on many factors, including:
If you get a kidney transplant, you can stop dialysis when your new kidney starts working.
Advertisement
Many people on dialysis continue to live active lives, including working, raising families and traveling. When you travel, a healthcare provider can help arrange for you to get dialysis at a center at your travel destination. If you’re doing peritoneal dialysis, you can take dialysis solution bags and a portable home dialysis machine (if necessary) with you.
If you use peritoneal dialysis, you may need to limit your exercise or certain physical activities when your abdomen fills with dialysate. Otherwise, exercise is OK for people on dialysis. Talk to your provider about specific activities and sports.
Call your healthcare provider if you experience:
Dialysis is a lifesaving treatment if you have kidney failure or end-stage kidney disease. It can’t cure kidney failure or ESKD, but it can help you manage your condition.
It’s a frequent process, and it might feel like it’s taking control of your life by keeping you away from your normal activities. But no matter how much time it takes, it’ll keep you alive until you can get a kidney transplant. A healthcare provider can review dialysis options with you to find the type that works best.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
You can’t reverse chronic kidney disease (CKD), but you can manage it. Cleveland Clinic healthcare providers are here to help you keep your CKD under control.
