Hemodialysis is a type of dialysis that does the work of your kidneys. It removes your blood, filters out toxins and excess fluids and sends your filtered blood back into your body. You may receive hemodialysis in a special healthcare facility or at home.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
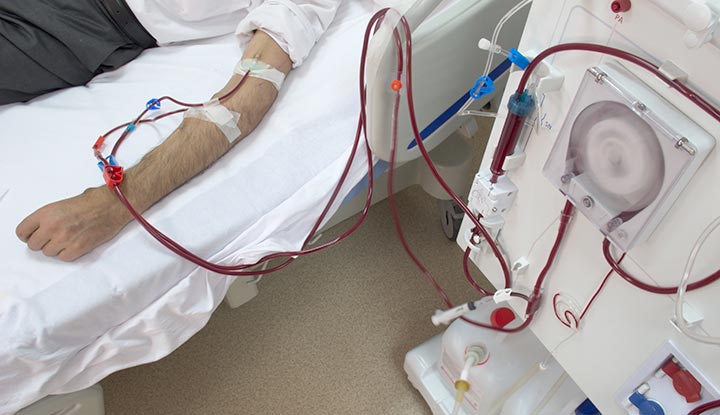
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/dialysis)
Hemodialysis is a type of dialysis that filters your blood to remove waste products and excess fluids. Your kidneys are part of your urinary system. Healthy kidneys filter your blood and make pee. But if they don’t work properly, dialysis does the work for them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
During hemodialysis (hee-moh-dahy-AL-uh-sis), a machine removes blood from your body. It filters your blood through an artificial kidney (dialyzer) to remove waste and fluid. It then returns the cleaned blood to your body.
You may need hemodialysis if you have very damaged kidneys that can no longer clean your blood properly. This usually happens in late-stage chronic kidney disease (CKD) or kidney failure. You may also need it if you’re waiting for a kidney transplant.
Hemodialysis (or haemodialysis) is the most common type of dialysis. Most people who need dialysis receive hemodialysis.
The dialyzer is the part of the hemodialysis machine that filters your blood. Your blood flows through tiny mesh tubes inside the dialyzer’s core. Waste products and excess fluids in your blood pass through the mesh tubes into dialysate. Dialysate is a fluid that consists of water, salts and electrolytes.
Your filtered blood returns to your body. The dialyzer then gets rid of the dialysate. The dialysate has your blood’s waste products and excess fluid.
There are two main types of hemodialysis. Your healthcare provider will review them and recommend the best type for you. They include:
For this type, you go to a healthcare facility that specializes in providing hemodialysis. A hemodialysis nurse or technician performs the procedure.
Advertisement
Most people get in-center hemodialysis at least three times per week. Each session takes between three and four hours.
This type takes place in your home. Over several weeks or months, your healthcare providers will teach you how to perform hemodialysis. They’ll also teach you how to fix common problems that may occur. You then perform hemodialysis yourself, on your own schedule.
There are three types of home hemodialysis:
You must prepare for your first hemodialysis session weeks or even months in advance.
If you can do hemodialysis at home, your provider will teach you how to properly perform it. They’ll also go over some common problems.
You’ll first have a minor surgery to make it easier to access your bloodstream. You may have one of the following procedures:
These procedures make the connection between your artery and vein easier to access during hemodialysis. They also help your blood flow in and out of your body faster.
In some situations, you may need to start hemodialysis quickly. Your provider may insert a temporary soft tube (catheter) into a vein in your leg, chest or neck.
Your provider will teach you how to clean your fistula or graft to prevent infections and feel for the vibrations (thrill) to ensure the access is working. They’ll also show you how to protect your fistula or graft. If you accidentally damage it, you may no longer be able to use it for hemodialysis.
Your hemodialysis nurse or technician will put two needles in your arm. Soft tubing connects both needles to the hemodialysis machine.
If you’re on home hemodialysis and have proper training, you may put the needles in yourself.
The hemodialysis machine:
Advertisement
During your hemodialysis session, the machine regularly monitors your blood pressure.
You may feel a slight pinch when the needles enter your fistula or graft. The needles are 15- or 16-gauge. They’re bigger than the needles that providers use for blood tests. The outer diameter of a 15-gauge needle is about 1.8 millimeters (mm). That’s about 2.5 times larger than the tip of a ballpoint pen. The outer diameter of a 16-gauge needle is slightly smaller — about 1.65 mm. But the hemodialysis process itself shouldn’t cause any pain.
Healthy kidneys work nonstop to filter your blood. They filter your blood even while you sleep. But even with advances in treatment, hemodialysis isn’t as efficient as healthy kidneys.
Healthy kidneys filter about 150 quarts of blood in a single day. Hemodialysis is only about 5% to 10% as effective as healthy kidneys.
You or your provider will remove the needles, apply pressure on the needle access site to stop it from bleeding and then clean your access areas. You may continue your everyday activities.
Advertisement
Many people feel tired or sick after hemodialysis sessions. Your symptoms may last a few hours. But others report having more energy with more frequent hemodialysis.
The main advantage of hemodialysis is that it does the work of your kidneys when they no longer can. Without it, toxins will build up in your blood (uremia). Uremia is fatal without treatment. Filtering out toxins that build up in your blood also helps many people feel better.
Another advantage is that sessions are usually only three times each week.
You may decide when and where to have your sessions for home dialysis. You may even choose to have your sessions overnight. Nocturnal home hemodialysis allows you to maintain a more consistent daily routine.
Hemodialysis also has some risks. Some people may have complications with their fistulas or grafts. These may include:
Rarely, the needles in your arm may come out, or a tube may disconnect from your hemodialysis. In these situations, the machine will alert you or your provider. The machine then shuts off to protect you from blood loss until someone fixes the problem.
Advertisement
Hemodialysis side effects may include:
If you’re on hemodialysis, the average life expectancy is five to 10 years. But some people have lived up to 30 years on hemodialysis. Your provider will give you a better idea of what to expect according to your situation.
Hemodialysis can’t cure late-stage CKD or kidney failure. Unless you get a kidney transplant, you’ll need hemodialysis for the rest of your life.
But sometimes, a sudden kidney failure only needs temporary dialysis. Your healthcare provider will stop dialysis once your kidneys start working again.
Most people start to feel better a few weeks after starting hemodialysis.
Reach out to your healthcare provider if you feel sick or tired after your session. They can prescribe medications or make adjustments to help you feel better.
If you choose not to start or decide to stop hemodialysis, you’ll develop uremia. Your kidneys will eventually fail. Over time, kidney failure is fatal. You may survive a few days or weeks without hemodialysis if you have kidney failure.
Refusing or stopping hemodialysis is a personal choice. Before making a decision, you should share your feelings with your provider, family and friends.
Managing CKD or kidney failure can be frustrating. The following tips may make hemodialysis easier:
Contact your healthcare provider if you experience:
During hemodialysis, your blood leaves your body and enters a machine that filters out waste products and extra fluid. Once the machine filters your blood, it goes back into your body.
During peritoneal dialysis, your provider attaches a catheter to your abdominal lining (peritoneal membrane). A bag with a dialysis solution then attaches to a catheter. The solutions flows from the bag into your peritoneal cavity. It absorbs waste products and extra fluid. About 60 to 90 minutes later, you drain the solution with the waste products and fluid into a clean, empty bag.
Hemodialysis is a time-consuming process. You may need regular sessions for the rest of your life. It can be frustrating and stressful. You may be upset about how it feels like it controls your life. These feelings are normal. It’s important to remember that you’re the most important person in charge of your care. You make the ultimate decisions about your health.
Providers are available to provide information and guidance. Talk to them if you have any questions or need support or advice.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your kidneys, you want experts by your side. At Cleveland Clinic, we’ll work with you to craft a personalized treatment plan.
