Dupuytren contracture is a genetic disorder that makes the tissue under the skin of your palms and fingers thicken and tighten. Symptoms take months or years to advance. There are lots of treatments. Surgery is an option, but it’s rare to need it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
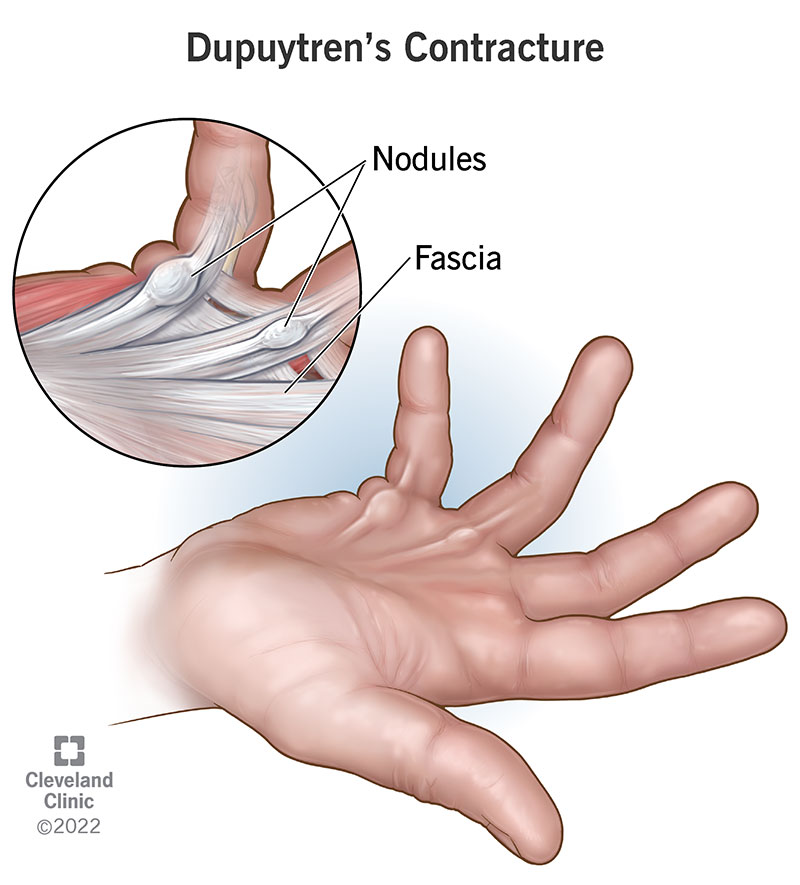
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/16941-dupuytrens-contracture.jpg)
Dupuytren contracture thickens and tightens tissue under the skin of your palms and fingers, which can make your fingers curl in toward your palm. It’s also known as Dupuytren disease or Viking’s disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Small bumps called nodules grow on the fascia in your hand. Fascia is the net-like tissue under your skin that supports your hand and fingers. Eventually, the nodules might form thick cords under your skin and bend your fingers so much that you can’t straighten them.
The growths that cause Dupuytren disease are always benign. This means they’re never a symptom or sign of cancer. You might need surgery. But more conservative treatments can manage many cases.
If you have mild symptoms, you may never even know you have Dupuytren contracture. It can take months (or even years) to develop. It most commonly happens to your ring and pinkie fingers. But it can affect any of your fingers, including your thumb.
Symptoms develop and progress in stages:
Advertisement
Other symptoms are rare, but can include:
Experts aren’t sure what causes Dupuytren disease. Healthcare providers consider it a genetic disorder. That’s because you’re much more likely to develop it if one of your biological family members has had it.
Dupuytren contracture can affect anyone. You may have a higher risk if you:
Having certain health conditions can increase your risk, including:
Dupuytren disease treatment complications are rare. But they can include:
A healthcare provider will diagnose Dupuytren contracture by looking at your hand and fingers. They’ll feel for nodules and cords under your skin. Your provider will measure the contracture if you have trouble straightening your fingers.
Your provider may suggest blood tests or an X-ray if they think you might have another condition that causes similar symptoms.
Which treatments you need will depend on how severe the symptoms are. If you only have mild symptoms, you might need:
It might take months or years for you to need the next level of treatment. That’s because Dupuytren contracture develops so slowly. But if you develop more severe symptoms, you may need:
Advertisement
Visit a healthcare provider if you think you have any Dupuytren contracture symptoms.
See your provider if it feels like the symptoms are getting worse. Or if they come back after you’ve started treatment.
The tabletop test is a good way to monitor symptom changes. Place your hand palm side down on a flat surface like a table. If any of your fingers aren’t lying flat, there’s a good chance the symptoms are progressing. Let your provider know as soon as possible.
Follow the instructions your provider gives you. Dupuytren contracture treatments take months. It’s important to do your stretches or physical therapy exercises as best you can, as often as you need to.
Following your therapy guidelines is especially important if you’ve had surgery. Some studies show that up to half of surgery’s benefits come from stretching and physical therapy after the operation itself.
You might have symptoms again in the future, even if you get better. If you have Dupuytren disease symptoms once, there’s a good chance the nodules or cords will grow back. Don’t be discouraged. But let your healthcare provider know right away if you notice symptoms again. The sooner you get treatment, the more likely it is you can manage symptoms before they advance.
Advertisement
Your hands are an important part of how you interact with the world and do the activities you love. Dupuytren contracture (Dupuytren disease) sounds scary, especially if you have more advanced symptoms. But it’s very treatable, and there are lots of ways to manage your symptoms. Your healthcare provider will help you find the right options to feel like yourself again.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Do certain health conditions seem to run in your family? Are you ready to find out if you’re at risk? Cleveland Clinic’s genetics team can help.
