
Danny Johnson had rarely been sick and didn’t spend much time in doctors’ offices. The 49‑year‑old London, Kentucky, grandfather considered himself healthy — until late 2024, when he began feeling persistently fatigued.
His wife, Holly Johnson, a respiratory therapist, noticed additional changes, including yellowing of his eyes and skin, and encouraged him to see a doctor.
“It took me a couple months to talk him into going,” Holly says. “But when he did, the blood work results came back, and they thought he had pancreatic cancer.”
Further testing ruled out cancer but revealed hepatic cirrhosis, a condition characterized by severe scarring of the liver, most likely caused by steatotic (fatty) liver disease. The diagnosis was unexpected. Danny had never faced a serious medical issue before.
Despite living more than six and a half hours away, the Johnsons decided to seek care at Cleveland Clinic, in Cleveland, Ohio, after one of Holly’s family members shared a positive experience.
Holly recalls, “My uncle says they’re the only reason he’s still alive at age 76. We went there, and we’re glad we did.”
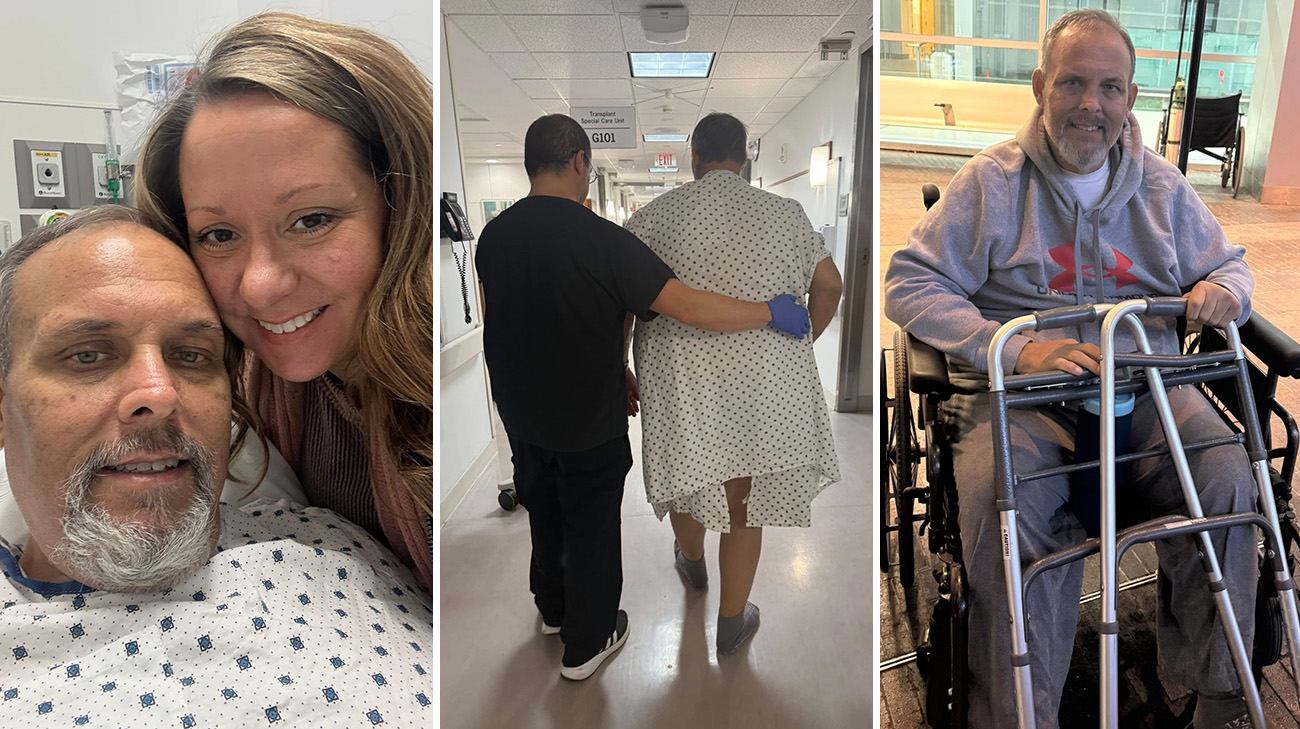
Danny needed a liver transplant after his condition progressed to end-stage liver disease. (Courtesy: Holly Johnson)
At Cleveland Clinic main campus, Danny met with hepatologist William Carey, MD, who confirmed the diagnosis. Dr. Carey and Holly also noticed signs of hepatic encephalopathy — mental confusion caused by declining liver function.
Additional testing in the weeks that followed confirmed Danny’s condition had progressed to end‑stage liver disease.
“A liver transplant was my only option. It was a shock,” Danny says. “I’ve never been sick in my life, and now I’ve got a life‑threatening disease.”
As he processed the diagnosis, Danny began thinking about what lay ahead. “I want to see my grandbaby grow up,” he told his doctors.
On December 18, 2025, Danny was placed on the liver transplant waiting list. Two days later, a deceased‑donor liver became available.
The Johnsons returned to Cleveland, where Danny became among the first patients at Cleveland Clinic to undergo a fully robotic liver transplant.
Danny’s transplant was performed by a surgical team led by Alejandro Pita, MD, a liver transplant surgeon at Cleveland Clinic and Director of Living Donor Liver Transplantation. Unlike traditional open liver transplant surgery, Danny’s procedure was completed fully robotically — an approach available at only a handful of hospitals nationwide for select patients.

Danny, Holly and Dr. Pita during a post-transplant follow-up appointment at Cleveland Clinic. (Courtesy: Cleveland Clinic)
“Among the most striking differences is the decrease in the patient’s post‑operative pain,” Dr. Pita explains. “The incisions we make are keyhole-size, so we don’t divide any muscle — except for one larger incision made low in the abdomen above the pubic area to remove the diseased organ and introduce the healthy one. The patient usually gets out of the hospital bed earlier and has less pain and a much shorter hospital stay.”
“Since I was a candidate for robotic surgery, my recovery was much easier than we expected. I was only in the hospital six days, instead of the two or three weeks we thought it would be,” says Danny.
While robotic surgery has been used for decades, applying the technology to liver transplantation has been especially challenging. The liver’s large size, combined with the complexity of liver disease — which often affects multiple organ systems — historically made open surgery the safer option.
Advances in robotic technology, along with extensive surgical training, have begun to change that.
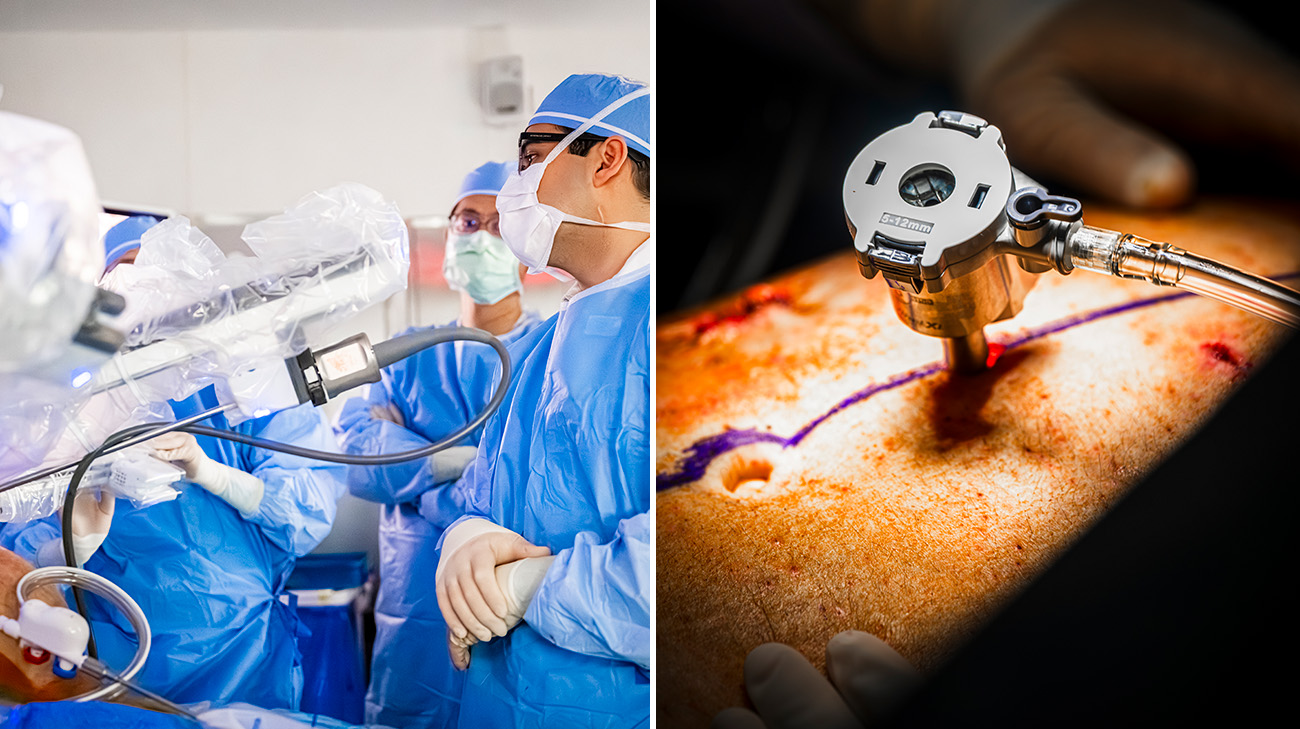
Dr. Pita and the surgical team performing a robotic liver transplant. (Courtesy: Cleveland Clinic)
“Liver transplant has been the ultimate challenge for robotic surgery,” Dr. Pita says. “We are very excited about the progress made by our surgical team, including our outstanding group of transplant surgeons and nurses who helped design both the workflow and the layout of the operating room. I am very appreciative of surgical leaders such as Dr. David Kwon and Dr. Jaekeun Kim, who were instrumental in the development of our robotic program.”
Because the approach is still in its early stages, only patients meeting strict criteria are eligible. Candidates must be otherwise relatively healthy, have an acceptable MELD (Model for End‑Stage Liver Disease) score, and have sufficient space within the abdomen — often affected by fluid buildup from liver disease. Danny met those criteria.
Three months after surgery, Danny is recovering at home and says he feels nearly back to good health. He’s grateful to Holly who helped care for him throughout recovery.
His 2‑year‑old grandson, Kade — affectionately known as “Baby Bubba” — now listens for Danny’s medication alarm and reminds him when it goes off.

Danny enjoying time with his grandson, Kade. (Courtesy: Holly Johnson)
Dr. Pita hopes more patients will benefit from similar outcomes as robotic liver transplantation continues to expand.
“This surgery has been a prime example of open surgical practice,” he says. “So, doing it robotically is a nice step forward.”
“There’s a lot of gratitude — for my care team and the advancements that made this transplant possible, and for the donor and their family who gave me this second chance. I carry that with me every day,” says Danny.
Related Institutes: Digestive Disease & Surgery Institute

