
“Before gene therapy, I felt like I was just existing. Now, I’m living,” says Annyanna Cash, reflecting on the innovative treatment she received for sickle cell disease. The 35‑year‑old mother says she can now focus on what matters most – raising her son and completing nursing school.
“So far, I haven’t had any hospitalizations since gene therapy. I’m able to go to work, attend school and come home to my son without worrying about health-related disruptions,” says Annyanna of Oakwood Village, Ohio.
Sickle cell disease is an inherited disorder that affects red blood cells. Typically, red blood cells are round and can move through small blood vessels to deliver oxygen to the body's tissues and organs.
In people with sickle cell disease, the genetic change in DNA causes a chemical alteration in hemoglobin and alters the shape of red blood cells into a sickle. These sickled blood cells can stick together and keep oxygen from getting to where it needs to go. This can lead to debilitating pain and life-threatening complications. Sickle cell disease most commonly affects people of African descent, but also impacts people with Hispanic, Middle Eastern, South Asian and Mediterranean backgrounds.
“Growing up, I remember not being able to go outside with the other kids at recess in the winter because the cold could trigger a pain crisis. Once I got to high school, I was in and out of the hospital more,” says Annyanna.

While sickle cell disease symptoms impacted Annyanna at a young age, she says her family helped keep her on track with her schoolwork and maintain a sense of normalcy. (Courtesy: Annyanna Cash)
Because of pain crises, pneumonia, low hemoglobin and other complications related to sickle cell, Annyanna was often hospitalized to receive pain medications, IV fluids, oxygen therapy and blood transfusions. At 25 years old, Annyanna began experiencing some of her worst symptoms during her pregnancy with her son.
“I needed regular blood transfusions to make sure I was OK and that he was OK, too,” says Annyanna. “My body just wasn’t responding the way it should, and I began developing avascular necrosis.”
Avascular necrosis (AVN) occurs when blood flow to bone tissue is blocked, and in sickle cell disease, the misshapen blood cells can restrict that blood supply. Without enough blood, bone tissue begins to die, and over time, this can weaken bones and joints and even lead to joint collapse. After giving birth to her son, Annyanna needed surgery on her hip and shoulder because of AVN.
“I was on crutches for months and had to relearn how to walk,” says Annyanna. “During that first year with my son, my health created challenges, and I leaned on a lot of support while I focused on caring for him. He learned how to walk alongside me in the hospital, with my IV pole. As he got older, I didn’t want all of his memories of me tied to hospital rooms. That’s when I knew something had to change.”
After seeing a news special on gene therapy years earlier, Annyanna knew it might hold promise for people with sickle cell disease, but she had to wait for the treatment to become available closer to home. That option became a reality for Annyanna at Cleveland Clinic Children’s, one of the sites participating in the multicenter RUBY Trial, which studied an experimental one-time gene editing therapy that used a patient’s own stem cells to help prevent red blood cells from sickling.
“Bone marrow transplant has long been an important curative option for some patients with severe sickle cell disease, but it requires a suitable donor and can carry risks such as rejection. One benefit of gene editing therapy is that it uses a patient’s own stem cells, so a donor isn’t needed and there’s no risk of rejection,” says Rabi Hanna, MD, Annyanna’s doctor and the chairman of the Division of Pediatric Hematology & Oncology and Bone Marrow Transplant at Cleveland Clinic Children's.
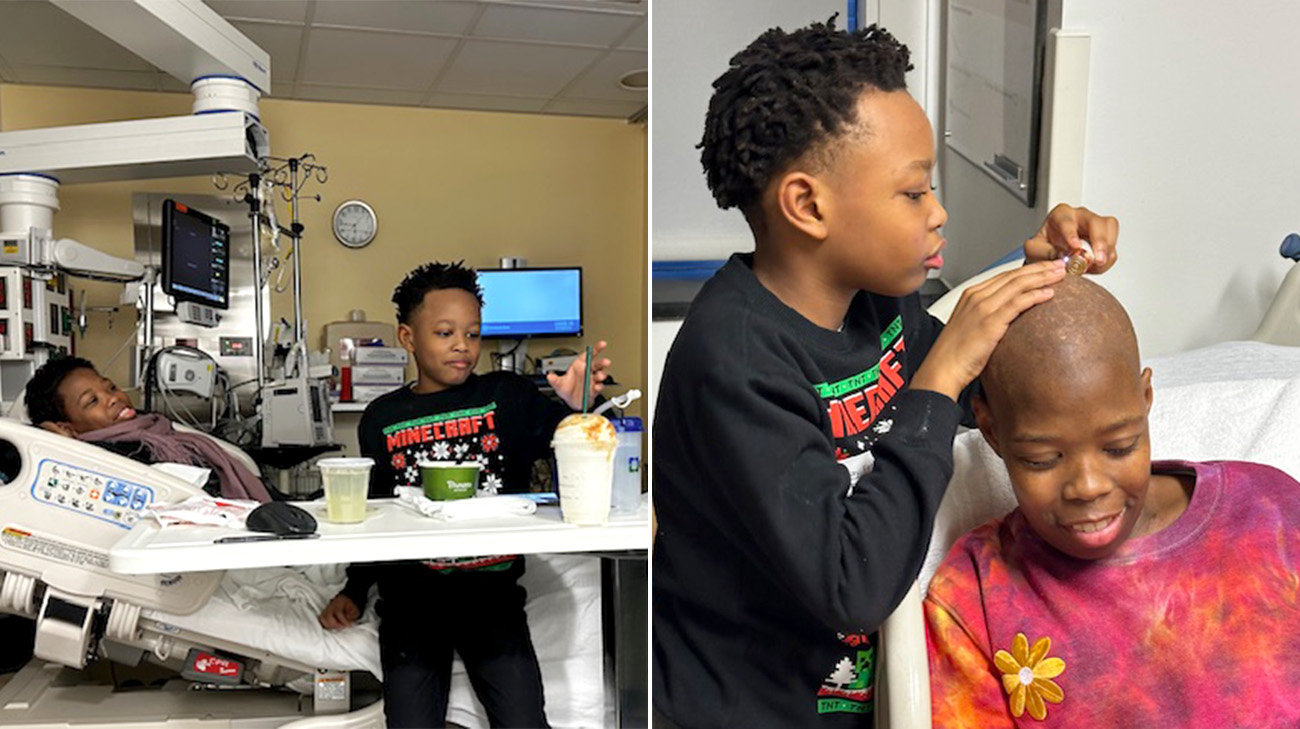
While the gene editing therapy process was long for Annyanna, she says her family’s support in the hospital helped her get through. (Courtesy: Annyanna Cash)
Because years of blood transfusions had caused iron to build up in her body, Annyanna needed to work with her care team to lower her iron levels before she could move forward with the treatment. She also underwent extensive testing to make sure she was a candidate for the trial.
Once she met the requirements, she was enrolled in the trial and began the treatment process, which started with stem cells being collected from her blood for gene editing. After the collection process, the stem cells were modified in a lab to help prevent sickling. Annyanna then underwent chemotherapy to make room in the bone marrow in order for the edited stem cells to take hold and start working. After that, the edited cells were infused back into Annyanna’s bloodstream in January 2024.
“Once those cells are returned to the body, the goal is for them to settle into the bone marrow and begin producing healthier red blood cells that are less likely to sickle,” says Dr. Hanna.
After receiving the edited cells, Annyanna spent about a month in the hospital for close monitoring and recovery. While the treatment process was long and challenging at times for Annyanna, she began noticing improvements fairly quickly.
“Having a great team of doctors and nurses throughout this process made a huge difference, and it was definitely a 180 for me towards the positive following gene therapy. About a month after treatment, I had my energy back and was soon able to do things both my son and I wanted to do without having to worry about getting sick,” says Annyanna.

Annyanna with her family and care team, which included Dr. Rabi Hanna. (Courtesy: Annyanna Cash)
Without the hospitalizations or pain she once experienced, Annyanna is now making more memories with her son. She can take him to his soccer games and travel to places like California, where she can swim alongside him without worrying about a pain crisis. She also enrolled in nursing school, became a licensed practical nurse and is now working toward becoming a registered nurse.
“I didn’t think this would’ve been possible before because in the past, I’d be taking classes and then have to stop because I’d get sick. Now, I currently don’t have any hospitalizations or emergency room visits interrupting my studies,” says Annyanna, who hopes to one day be a nurse at Cleveland Clinic.
Along with Annyanna, Dr. Hanna says the majority of patients in this trial did not have any painful sickle cell crises after treatment, achieving what he calls a functional cure.
“Our aim has been to achieve a functional cure to help prevent any future damage caused by sickle cell disease, and these latest results are compelling,” says Dr. Hanna.
The trial results, Dr. Hanna and colleagues published in The New England Journal of Medicine, also showed most patients saw key blood cells recover within a month after treatment. By six months, their average hemoglobin level had risen from 9.8 to 13.8 grams per deciliter, much closer to the range seen in people without sickle cell disease. Patients also maintained high levels of fetal hemoglobin, a form of hemoglobin that helps keep red blood cells from sickling.

After gene therapy, Annyanna says she celebrates what she calls two “born to be great” days: her birthday and the day she got her modified cells. She now looks forward to making new memories with her son and completing nursing school. (Courtesy: Annyanna Cash)
As for Annyanna, she’s continuing to undergo therapeutic phlebotomies for now to lower excess iron from years of prior blood transfusions. Her Cleveland Clinic Children’s care team, which she describes as a second family, will also continue monitoring her to ensure the one-time gene editing therapy remains successful. After seeing how much gene therapy has changed her life, she hopes her story can uplift others and encourage more people to explore clinical trials.
“Whether you’re dealing with sickle cell or another obstacle in life, it all starts in the mind. Try to remain hopeful and positive. I always knew things could change, and this trial showed me that. If those who were involved hadn’t volunteered to be part of it, we may not have known about the possibilities of this potential treatment option. Everyone in life has a purpose, and I feel like mine was to go through this trial and give hope to others,” says Annyanna.
Related Institutes: Cleveland Clinic Children's

