“I feel like I can just be a mom again,” says Jessica Krauser as she reflects on life after undergoing an innovative treatment for Parkinson’s disease. Following her diagnosis at just 37 years old, the mother of two turned to deep brain stimulation (DBS) as her symptoms progressed.
“I knew it was time for something else when I was at dinner with my family on vacation. I couldn't just sit in the chair and calmly eat my food. My body was all over the place,” says Jessica of Columbus, Ohio.
Looking back on her Parkinson’s journey, Jessica says her first symptom presented as a hand tremor in 2017. She would only get it at certain times, including when she was presenting at work or reading at church.
“My kids would always notice it and ask, ‘Are you nervous? Are you scared?’ But I wasn’t and thought it was just stress,” says Jessica.
She eventually brought it up to her primary care doctor, who recommended she see a neurologist if it got worse. “I didn’t connect shaking to neurology. I was also 35 at that point, and I was thinking why in the world would I need to see a neurologist?”
Along with the tremor, Jessica started noticing stiffness and rigidity in her leg. At the time, she was preparing for her first half marathon and thought this symptom was related to the training.
“Many nights someone would have to rub my calf muscle because it felt like there was a tight knot that I just couldn’t get out,” says Jessica.
As time went on, Jessica’s symptoms got more pronounced. Simple tasks like cutting vegetables and typing became difficult. Her one foot felt like it was dragging behind her, and she would shake uncontrollably when cold.

As her Parkinson’s progressed, Jessica found it harder to focus on the moment instead of her symptoms. (Courtesy: Jessica Krauser)
“I was at my yearly gynecologist appointment, and because it was cold in the office, my tremor was really obvious. She took notice and suggested I see someone about it,” says Jessica.
She followed up on her gynecologist’s advice and eventually went to a movement disorder specialist. Based on her symptoms and brain imaging, the doctor officially diagnosed Jessica with Parkinson’s disease in 2019.
“At this point, I had pretty much already diagnosed myself because I checked every box for Parkinson’s. But part of me was relieved. I was like, OK, I’m not crazy – there is something going on with me,” says Jessica.
With the average onset age of the disease being around 60 years old, Jessica says it was hard for her family and friends to accept the diagnosis. According to the Parkinson’s Foundation, young-onset Parkinson’s affects about 4% of the 1 million people living with the condition in the United States. Additionally, the symptoms Jessica was struggling with the most weren’t obvious to others.
"My Parkinson's isn't always something people can see. For me, it was the rigidity, tightness and stiffness in my arms and legs. It was constant and something only I could feel. People tend to think of Parkinson's as just shaking, but it presents itself in many ways depending on the person," says Jessica.
Jessica’s care team started treating her Parkinson’s with medication. And while they would provide relief for a few months, her symptoms would inevitably return – often with frustrating side effects. She kept having to change her medications in hopes of finding something that worked.
The active mom soon found simple things like going for a walk or cooking for her family more difficult, as the rigidity and stiffness took over her arms and legs. She also started having dyskinesias, which are involuntary movements that result as a complication from long-term use of certain Parkinson's medications.
“The dyskinesia made it uncomfortable to walk or even sit down. I was tired all the time because I was moving all the time. It was a roller coaster ride for those first few years,” says Jessica.

Jessica at an appointment with Dr. Richard Rammo before her deep brain stimulation surgeries. (Courtesy: Cleveland Clinic)
After her diagnosis, Jessica launched a podcast to create a space for herself and others to share their experiences with Parkinson’s disease. It was through conversations on this platform she discovered more about DBS as well as the team at Cleveland Clinic.
Described as a pacemaker for the brain, DBS involves implanting a device to deliver electrical currents to specific parts of the brain that control movement. This stimulation helps to modulate the abnormal brain signals that cause Parkinson’s symptoms.
“Most people with Parkinson’s see initial improvement from medications, but for patients like Jessica, some may go on to develop dyskinesia or notice symptom control becomes less consistent over time. When medications aren’t as effective, we can look at DBS as a potential treatment option,” says Cleveland Clinic neurosurgeon Richard Rammo, MD.
Since not everyone qualifies for DBS, Jessica first underwent testing to confirm the treatment would be effective for her. Once her care team determined she was a candidate, her first surgery was scheduled for July 2025.
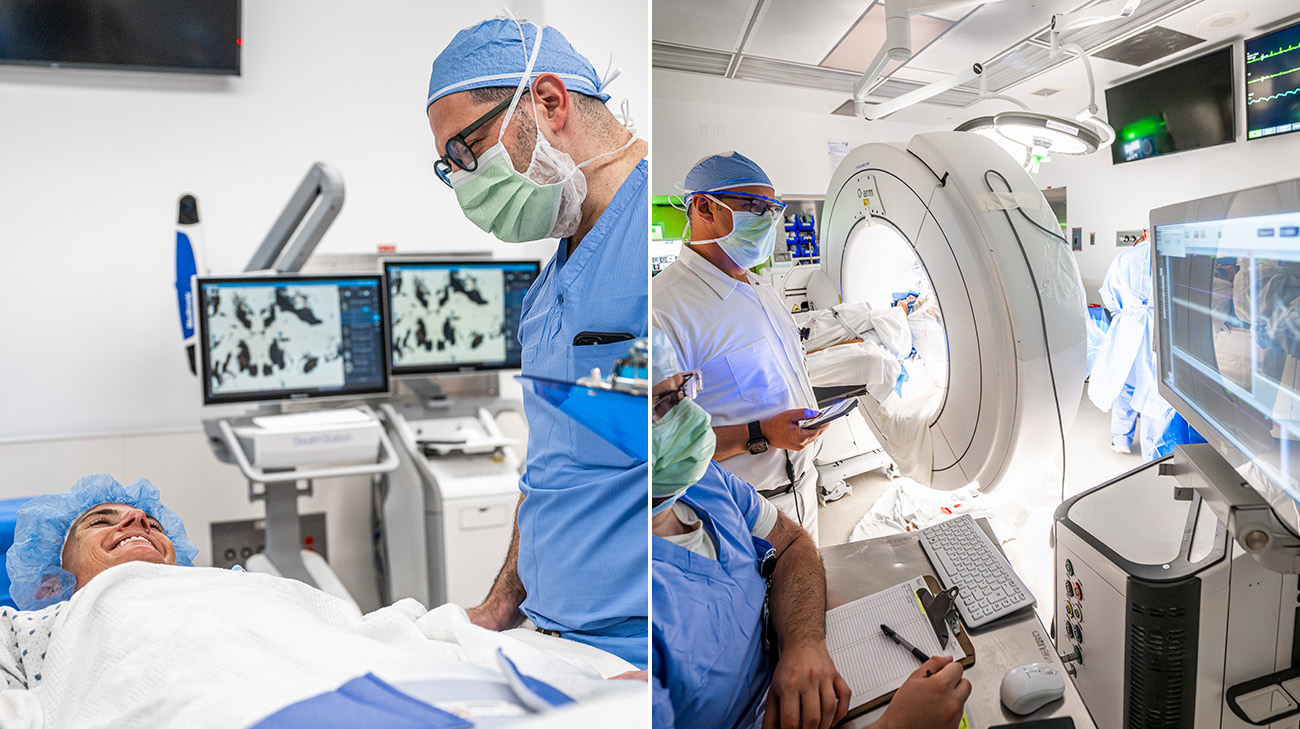
Jessica says her care team made her feel at ease throughout all phases of her deep brain stimulation surgeries. (Courtesy: Cleveland Clinic)
“For most patients, we do this procedure in three parts. During the first surgery, we place an electrode on one side of the brain. During the second surgery, we place an electrode on the other side of the brain. The final surgery involves placing the stimulator battery in the chest and connecting it to the DBS electrodes. This battery sends electrical pulses to the electrodes in the brain to help regulate abnormal brain activity for symptom relief,” says Dr. Rammo.
Following her successful surgeries, Jessica’s DBS device was turned on. She then had multiple programming sessions to get her stimulation perimeters just right. Depending on the specific DBS device used as well as the patient’s needs, they can either have traditional DBS, which gives the same stimulation to the brain 24/7, or adaptive deep brain stimulation (aDBS).
“Jessica has adaptive technology, which means it can adjust stimulation in real time based on her brain activity. If her medications start to wear off, it can sense that and increase the stimulation to better manage her symptoms. It can also reduce stimulation when less is needed, like when she’s sleeping,” says Ellen Walter, CNP, who has been programming Jessica’s DBS.
Jessica recalls noticing the biggest difference after her third programming session. Before, her legs felt like heavy weights while walking. With aDBS, she noticed that finally starting to ease.
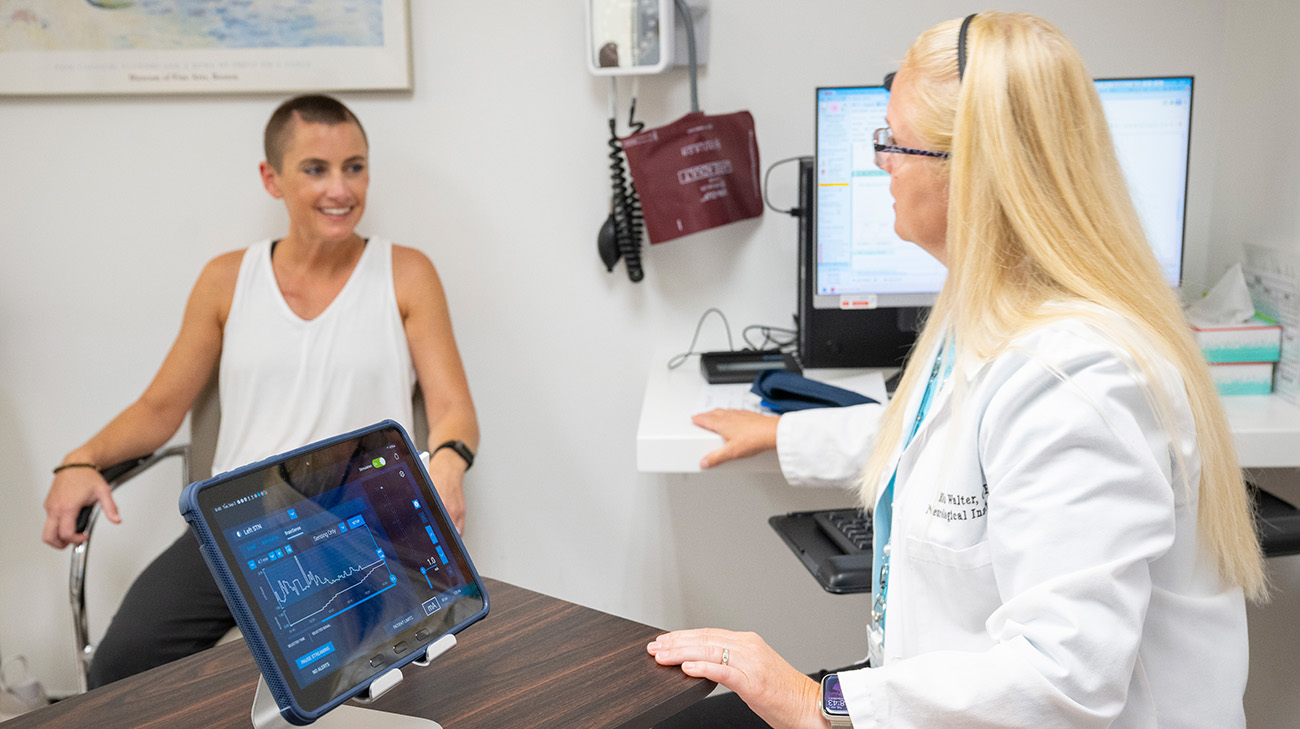
After her surgeries, Jessica underwent programming sessions with Ellen Walter to fine-tune her stimulation for optimal symptom control. (Courtesy: Cleveland Clinic)
“After the initial programming sessions, I was no longer feeling that constant tightness and tension that kept me up at night. I found myself just laying in bed in the morning because it felt so nice not to be stiff anymore,” says Jessica.
With aDBS, Jessica also went from needing to take medications every few hours to just once in the morning and once at night. While aDBS does not stop Parkinson’s from progressing, her symptoms overall are currently well controlled.
“Before deep brain stimulation, I was either feeling my symptoms or I was dyskinetic. Something was always going on, and I was constantly thinking about it. Now, my symptoms are so well controlled I wake up every morning and don’t have to think about Parkinson’s. I’m able to focus on other things, like my family and friends,” says Jessica, who will continue following up with her care team to adjust her aDBS programming and medications as needed.
Moving forward, Jessica is excited to continue her podcast and expand the nonprofit she helped found, which aims to support people with Parkinson’s through education, exercise and community. Jessica and her care team hope sharing her story offers reassurance to others that there are treatments available, and they don’t have to face Parkinson’s alone.

With deep brain stimulation and medication, Jessica says she’s better managing her symptoms and aims to keep raising awareness about Parkinson’s disease and available treatments. (Courtesy: Jessica Krauser)
“Many patients out there may not even know deep brain stimulation is a treatment option. We need to continue raising awareness about all the tools we have available to help patients with Parkinson’s live their lives to the fullest,” says Dr. Rammo.
“There are so many things you don’t know when you’re first diagnosed with Parkinson’s. For me, it was a lonely, hopeless feeling that was just as crippling as the disease can be itself. That’s why finding your community and support system is so important. Whether it’s a tip to manage symptoms or a new treatment, I’m always learning more from others about the disease. Just know you don’t have to face this alone,” says Jessica.
Related Institutes: Neurological Institute

