Pulmonary vein isolation ablation is a minimally invasive procedure to treat atrial fibrillation (Afib). Ablation therapy uses hot or cold substances to create scar tissue. The scars disrupt abnormal electrical signals that cause atrial fibrillation. This procedure may be right for you if other arrhythmia treatments aren’t successful.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pulmonary vein isolation is a procedure to treat atrial fibrillation (Afib). Atrial fibrillation is an abnormal heart rhythm (arrhythmia) that begins in your heart’s upper chambers (your atria). If left untreated, atrial fibrillation can lead to stroke.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pulmonary vein isolation treats Afib by targeting your pulmonary veins. These are the veins that bring oxygen-rich blood back to your heart’s left atrium. Your pulmonary veins are where the abnormal electrical signals that cause Afib usually begin.
The treatment is a type of heart ablation. That means it uses very hot or cold temperatures to create small scars. Scar tissue inside your pulmonary veins disrupts the electrical signals that cause Afib, preventing them from reaching your atria.
Pulmonary vein isolation may be the best treatment option for patients who:
Researchers are exploring whether some patients might benefit from pulmonary vein isolation as an initial (first-line) treatment.
Studies show higher survival rates with first-line pulmonary vein isolation ablation than with antiarrhythmic drugs. However, more research is necessary to determine whether this should become the standard of care.
You’ll need a thorough evaluation to determine whether you’re a good candidate for this treatment. Healthcare providers start by taking your medical history and performing a physical exam. You may also need heart tests, such as:
Advertisement
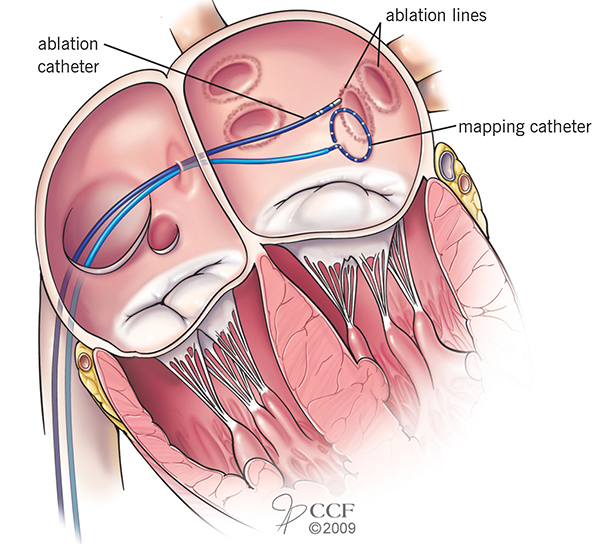
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/pvai-procedure.ashx)
Pulmonary vein isolation is a type of catheter ablation, which means it delivers ablation therapy through a long tube inserted into a vein.
There are two methods of creating scar tissue. They include:
Each option has risks and benefits. Research has demonstrated that radiofrequency and cryoablation produce similar outcomes with no significant difference in safety. Your healthcare provider will explain the risks and benefits of each method before the procedure.
Healthcare providers commonly place people under general anesthesia during pulmonary vein isolation. You’ll become relaxed and drift off to sleep. In some cases, your healthcare provider might use only a local anesthetic. They’ll tell you what to expect in your situation.
Here’s what to expect during pulmonary vein isolation ablation:
Your healthcare provider will apply several types of monitors to your body to keep track of your heart rhythms during the procedure. You’ll have:
Advertisement
The pulmonary vein ablation procedure may last four to six hours. Please let your family know that the preparation and recovery take several hours. They should plan to be at the hospital all day. You’ll stay in the hospital overnight.
After the procedure, your doctor will discuss the results with you and your family. You’ll stay in bed for four to eight hours after the procedure. Nurses will monitor your heart rate and rhythm overnight. Most patients go home the next morning. Your nurses will remove your catheters and bandage the incisions before you go.
Pulmonary vein isolation ablation is generally safe. As with any heart procedure, it comes with a low risk of certain complications, such as:
You may feel general soreness, fatigue or chest discomfort during the first 48 hours after the procedure. You can return to daily activities after that. However, you’ll need to wait a few weeks before resuming anything strenuous, like exercising.
Advertisement
It takes several weeks for the scarring from ablation to form and improve your condition. You’ll likely continue to have atrial arrhythmia for up to 10 weeks after the procedure. In rare cases, it may get worse before it gets better.
You’ll need to take certain medications for a few months, including:
You’ll also need to take periodic blood tests to reevaluate the dosage of anticoagulant medication you should be taking.
Your first follow-up appointment will be three to four months after your pulmonary vein isolation procedure. You’ll have another follow-up after a year. During your follow-up appointments, your healthcare team may use several tests to check on your heart, including:
Pulmonary vein isolation helps many people achieve lasting symptom relief. Sometimes, multiple ablation procedures are necessary. People with hypertrophic cardiomyopathy might not achieve the same outcomes as people without it.
This treatment reduces the impact of arrhythmias on daily life but doesn’t cure them. You’ll still need to take blood-thinning medication. Even if you feel better, you still face an increased stroke risk. Ongoing monitoring is necessary to detect arrhythmias that return after treatment.
Advertisement
Contact your healthcare provider if you start experiencing signs of complications, such as:
Pulmonary vein isolation disrupts an abnormal heartbeat. As a minimally invasive procedure, it’s gentle on your body, allowing you to recover quickly. You’ll get long-term relief from atrial fibrillation symptoms and an alternative to antiarrhythmic drugs. Ongoing care from your cardiologist can help you stay as healthy as possible.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart rhythm is out of sync, the experts at Cleveland Clinic can find out why. We offer personalized care for all types of arrhythmias.
