An adenoidectomy is surgery to remove your child’s adenoid glands. Your child may need this surgery if their adenoids have become swollen or enlarged because of an infection or allergies. Removing their adenoids can help if your child has breathing problems that keep them up at night or frequent sinus infections.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
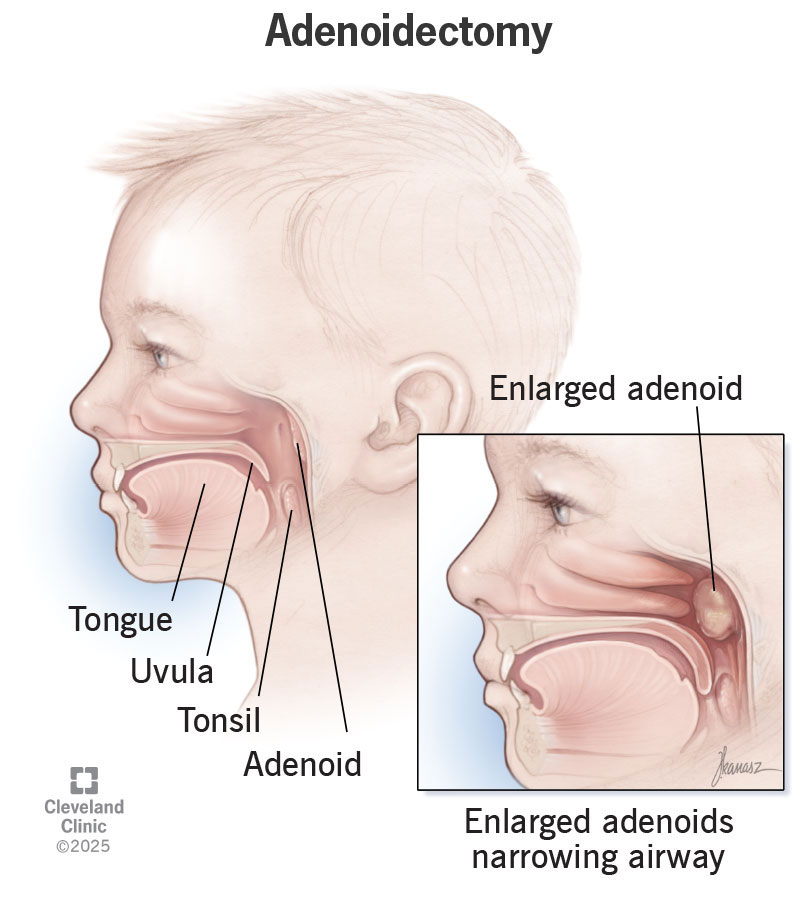
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15447-adenoidectomy-adenoid-removal)
An adenoidectomy, or adenoid removal, is surgery to remove your child’s adenoid glands. Adenoids are small lumps of tissue located behind your child’s nose in their upper airway. Like tonsils, adenoids are part of the body’s immune system. They fight germs you breathe in.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
While adenoids help protect your child from viruses and bacteria, these glands can become swollen. Infections and allergies can cause the swelling. Some children are just born with large adenoids.
Enlarged adenoids may need to be removed if they’re partially blocking your child’s airway. The procedure is mostly for children between 1 and 7 years old. This is because many children’s adenoids get smaller after age 7. Less often, adults need this procedure, too.
Adenoid removal surgery treats enlarged adenoids that are narrowing your child’s airway. This can cause a range of issues, including:
An adenoidectomy may help improve how your child’s ear functions. For example, it may be used to treat eustachian tube dysfunction. With this condition, the tubes that connect your child’s middle ear to their throat become blocked. This can cause pain and hearing issues.
Advertisement
Your child’s healthcare provider will tell you which medicines your child should or shouldn’t take leading up to surgery. They may tell you to avoid giving them medicines that can slow healing, like aspirin or ibuprofen.
Make sure your child fasts based on their provider’s instructions. Usually, children need to stop eating solid foods at least six hours before surgery. Their stomach should be empty for adenoid removal surgery.
You should also monitor your child for symptoms of a cold, flu or another respiratory infection. Their provider may need to postpone surgery if your child gets sick.
An ear, nose and throat (ENT) surgeon commonly performs this procedure. Here’s what’s involved:
The surgeon may also remove your child’s tonsils (tonsillectomy) if they’re causing symptoms. Adenoidectomy and tonsillectomy are often done together.
Sometimes, an adenoidectomy happens alongside the placement of tympanostomy tubes. These tubes drain ear fluid related to infections.
It’s a quick procedure. The surgery only takes about 30 minutes. Most children go home the same day.
An adenoidectomy is a safe surgery that can relieve your child’s symptoms. Although adenoids are part of your child’s immune system, adenoid removal won’t make their immune system weaker. Your child doesn’t need adenoids to fight germs. They’ll actually be healthier without enlarged adenoids.
Still, as with any surgery, there are potential (but rare) risks.
They include:
Sometimes, adenoids grow back. If the tissue continues to cause problems, your child may need surgery twice. But this is rare.
Your child’s care team will take them to the recovery room. Most children wake from the anesthesia within an hour or two. Once your child wakes up, a healthcare provider will make sure they can breathe, cough and swallow.
They’ll likely be able to go home that same day. If your child’s provider wishes to monitor them, they may need to stay in the hospital overnight.
Almost all children make a full recovery after an adenoidectomy.
Advertisement
Your child should recover within a week or two following surgery. During recovery, they may experience:
Your child may need pain medicine to help them rest during recovery. Usually, the pain lessens within the first two days after surgery. Their healthcare provider can prescribe pain medicine in liquid form that will be easy for your child to swallow.
Follow their healthcare provider’s guidance on how much rest your child needs. To prevent infections, avoid places where they can be exposed to germs. It’s also a good idea to avoid smoky environments. The smoke may irritate their nasal passages.
Steer clear of foods that are spicy, crunchy or acidic (like citrus), which may irritate their throat and nasal passages. Instead, give them:
You can also use a cool mist humidifier in their room to keep their nasal passages moist and healthy. Just be sure to clean it regularly to prevent mold.
Your child’s healthcare provider will let you know when they should return to school. Many children need at least a week out of school to rest as part of their recovery.
Advertisement
Watch your child closely after you take them home. Call their provider if you notice any of the following in your child:
There isn’t an ideal age for adenoid removal. But most surgeries happen between the ages of 2 and 7. This is when children are more likely to get sick and have enlarged adenoids.
It’s important not to delay care if doing so increases the risk of complications. Over time, sleep apnea related to enlarged adenoids can cause speaking and learning difficulties. Adenoids blocking your child’s nasal passages can lead to mouth breathing. This impacts how the bones in your child’s face develop.
Timely treatment reduces these risks.
Many parents find that the hardest part of adenoid removal is preparing their child emotionally for surgery. Helping them through recovery can be challenging, too. Working with their healthcare provider can help.
For example, some providers “perform” the surgery on a teddy bear or special toy beforehand. That way, a child having surgery can see there’s nothing to fear. Your child’s provider can walk you through every step of your child’s recovery timeline. That way, you know how to care for and comfort your child once they’re home.
Advertisement
An adenoidectomy is one of the most common surgeries children get. It can help them breathe and sleep better. And there are very few risks involved. Lean on your child’s healthcare provider for guidance if they recommend this surgery. They can help you and your child prepare for surgery and recovery.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Watching your child struggle to breathe and get a good night’s rest can be hard. Cleveland Clinic experts can treat their enlarged adenoids with an adenoidectomy.
