Kyphoplasty is a procedure to treat compression fractures, usually caused by osteoporosis or spinal tumors. This minimally invasive procedure takes less than an hour and offers pain relief within days. You’ll be able to get back to your regular activities shortly after you go home.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
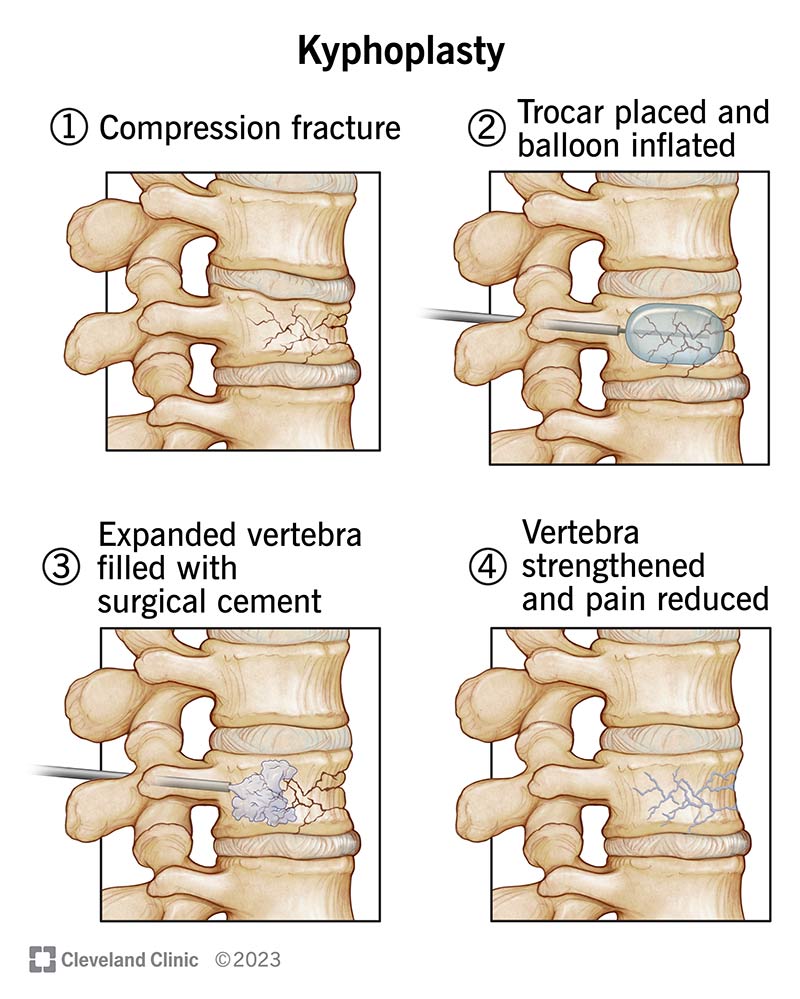
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/kyphoplasty)
Kyphoplasty is a minimally invasive procedure to treat compression fractures in your spine. These are painful breaks in the vertebrae (the bones that make up your spine). Compression fractures can cause the bones in your spine to collapse, leading to kyphosis, or a curve in your spine that makes it look like you’re hunched over. It can limit your breathing or the function of your abdominal organs. Kyphoplasty prevents this curve from happening.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may hear your healthcare provider refer to kyphoplasty as a balloon kyphoplasty.
Kyphoplasty treats vertebral compression fractures. The most common cause of these fractures is the thinning and weakening of bones (osteoporosis) or a spinal injury. This procedure can also treat pathologic fractures (a broken bone caused by an underlying condition) related to spinal tumors or multiple myeloma.
No. Kyphoplasty is minimally invasive because a surgeon will make a small puncture through your skin instead of an incision (cut).
Over 19,000 kyphoplasty procedures happen each year in the United States.
You may be a candidate for kyphoplasty if you have painful, worsening back pain caused by a compression fracture. You may not be able to move or function as well as you used to because of the fracture.
To be a candidate for kyphoplasty, your pain must relate to the compression fracture, not another condition like disk herniation, arthritis or stenosis.
A healthcare provider will perform imaging tests to confirm the presence of a vertebral fracture. If you have osteoporosis, your healthcare provider may order a dual-energy X-ray absorptiometry (DXA) scan.
At an appointment before your kyphoplasty procedure, your healthcare provider may do the following:
Advertisement
They’ll also schedule the date of your surgery during this visit so you have time to prepare for it. Your surgeon will give you specific instructions before your surgery, like:
On the day of your surgery, an anesthesiologist will give you moderate sedation or anesthesia. This depends on what your surgeon needs to do. With moderate sedation, you’ll feel minimal discomfort or you’ll be asleep with general anesthesia.
During the kyphoplasty procedure, you’ll lie on your stomach. Your surgeon will insert a hollow needle, called a trocar, through your skin and into the affected bone in your spine. A type of X-ray, called a fluoroscopy, guides the trocar into the proper position.
Once the trocar is in place, your surgeon will put an inflatable, balloon-like device into your vertebra through the trocar. As the balloon inflates, it helps regain vertebral height and opens a space for your surgeon to inject bone cement there. The cement prevents your bones from further collapsing.
Kyphoplasty is an outpatient procedure that a surgeon will perform in a hospital or outpatient clinic. You’ll go home the same day.
A kyphoplasty procedure takes less than an hour to complete for one section of your spine.
Your surgeon will give you specific instructions to take care of yourself after a kyphoplasty procedure. You’ll be able to go home the same day. Make arrangements to have someone drive you home when the procedure is over.
You can return to normal activities after kyphoplasty but try to avoid hard efforts like heavy lifting until your overall bone health improves.
Your surgeon will place a bandage over the area of the skin where they performed the procedure. Keep the bandage on for two days. You may need someone’s help to take the bandage off when your healthcare provider approves it. Your provider may recommend taking showers instead of baths as you heal.
Let your healthcare provider know if you experience swelling or severe pain after surgery.
Advertisement
The benefits of kyphoplasty include:
An estimated 92% of people who undergo kyphoplasty report better pain relief after the procedure.
You won’t feel strong, sharp pain during a kyphoplasty procedure since you’ll receive moderate sedation or anesthesia. You may feel sore after the anesthetic wears off. But, this should resolve within a couple of days. Applying ice to the area can help relieve any soreness.
Complications are rare for kyphoplasty procedures but could include:
To avoid these risks, especially your risk of additional fractures, your healthcare provider will ensure that you’re taking medications to improve your bone quality if you have osteoporosis.
Kyphoplasty usually provides pain relief and improved mobility (movement) within 48 hours of the procedure. In some cases, you may feel pain relief immediately. Pain caused by the procedure itself should go away within two to three days.
Advertisement
Your healthcare provider will advise you on when it’s safe to return to your regular activities. For most people, you can get back to your daily routine after your anesthetic wears off. Avoid strenuous activities for several weeks following kyphoplasty.
Contact your healthcare provider right away if you:
Kyphoplasty is a very low-risk procedure. Studies show that the success rate of kyphoplasty is very positive. You might feel pain relief right away, or it might take a few days for you to feel better. While side effects are possible, your risk is very low. If you have any questions about the procedure, talk to your surgeon or care team. They’ll be available to answer any questions you might have to help you prepare and recover.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
You might have brittle bones, but an osteoporosis diagnosis doesn’t mean you can’t keep having fun in life. Cleveland Clinic is here to help.
