Kyphosis is an excessive forward curve of your spine. This condition can cause you to lean forward like you’re hunching over. It might cause back pain and stiff muscles. There are nonsurgical and surgical treatment options available.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
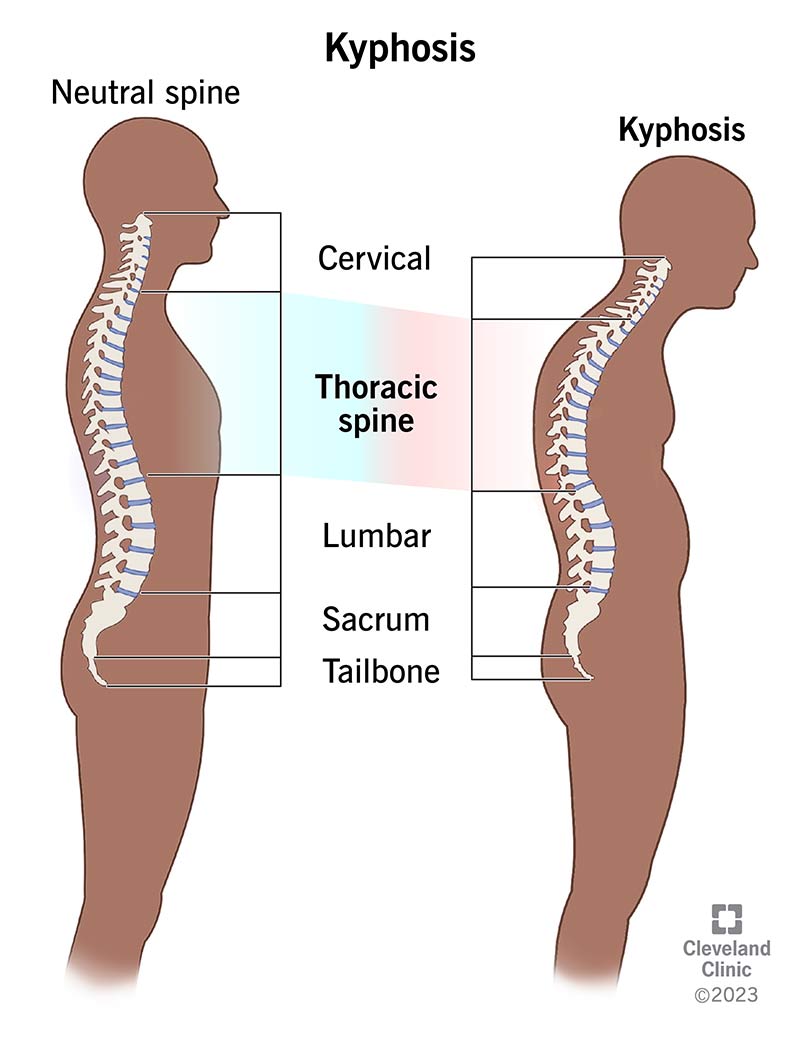
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17671-kyphosis)
Kyphosis is a condition where your spine curves outward more than it should. This causes your upper back around the thoracic region (the part of your spine between your neck and ribs) to bend forward. The curvature can make it look like you’re hunched over or slouching. People sometimes call it “hunchback” or “roundback.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your spine has natural curves. These curves support your posture and help you stand straight. But excessive curvature can affect your body and make standing difficult.
Most of the time, kyphosis doesn’t cause health problems or need medical treatment. But it may make you feel self-conscious about how you look. In severe cases, kyphosis can cause pain or breathing issues. Severe kyphosis may require surgery.
There are several types of kyphosis. Some of the most common include:
Advertisement
Less than 8% of school-aged children in the United States experience Scheuermann’s kyphosis.
Hyperkyphosis (severe kyphosis) affects an estimated 20% to 40% of adults over age 60. On average, the forward angle of your upper spine increases about 3 degrees each decade (10 years).
The main symptoms of kyphosis include:
Severe kyphosis may cause the following symptoms:
If you have difficulty breathing, contact 911 or your local emergency services number.
The cause of kyphosis varies depending on the type but could include:
No. Kyphosis and scoliosis are both conditions that affect your spine. They can happen together, but one doesn’t cause the other. Kyphosis is the abnormal curvature of the spine, from front to back. Scoliosis is the abnormal curvature of the spine, from left to right or sideways.
A kyphosis diagnosis is common between ages 13 and 16 for postural and Scheuermann’s kyphosis. This is because teenagers’ bones are growing rapidly. But it can develop in anyone at any age. As humans age, the vertebrae lose flexibility, and the spine may begin to tilt forward.
You can also be born with the congenital form of kyphosis. This can happen in addition to other underlying health conditions that affect your growth and development in the uterus.
Complications aren’t common for mild cases of kyphosis but they can happen when you have a severe spine curve. Complications may include:
Among children, you (your child’s caregiver) or a school physician (nurse) may notice symptoms of kyphosis, especially at school during a scoliosis screening. Your child’s school may recommend your child visit a primary care physician for an exam to confirm a diagnosis.
At any age, your healthcare provider will diagnose kyphosis after a physical exam. During the physical, your provider will ask you or your child to perform a bending test. You’ll stand with your feet together, knees straight and your arms hanging at your side. Then, you’ll gently bend forward, looking toward your feet. This test helps your provider see the spine curve or any other spine problems.
Advertisement
A spine X-ray helps your healthcare provider measure the curve of your spine to diagnose the condition. The natural curve is between 20 and 45 degrees. Your provider will diagnose kyphosis if the curve is greater than 50 degrees.
In addition, your healthcare provider will offer tests to determine if your symptoms are the result of an underlying condition or if the curve in your spine affects other parts of your body. Tests may include:
Treatment for kyphosis varies but could include:
Advertisement
A healthcare provider will examine your spine and offer treatment options based on your:
You may qualify for spine surgery if you have:
Each type of treatment comes with possible side effects. Talk to your healthcare provider before treatment begins to understand the risks and side effects. For example, side effects of surgery could include infection and bleeding at the incision site.
Kyphosis is a treatable spine condition. The curve may or may not cause you pain and you might not even notice it until a healthcare provider mentions it during an exam. The goal of treatment is to stop the curve from getting worse. In severe cases, you may need surgery. But most people with kyphosis don’t need surgery.
Kyphosis can return, even after treatment. You may need to make lifestyle changes to adjust your posture. This means being more aware of how you sit, stand and move throughout the day. For example, you might choose to use a roller bag instead of carrying schoolbooks in a backpack. Talk to your healthcare provider about what you can do to prevent kyphosis from coming back.
Advertisement
An early kyphosis diagnosis leads to the best outcome. Most people who receive an early diagnosis don’t need surgery and can manage the condition with nonsurgical options. Kyphosis can get worse if left untreated. This can cause health problems like difficulty breathing.
It’s important to monitor kyphosis regularly with a healthcare provider throughout your life, even after treatment.
You can’t prevent all types of kyphosis. You can take steps to prevent postural kyphosis by:
Talk to a healthcare provider if you notice a curve in your or your child’s spine that affects your or their posture. A healthcare provider can evaluate your symptoms and help you improve your posture, if necessary.
Visit the emergency room if you have difficulty breathing.
If you or your child have kyphosis, ask your provider:
Kyphosis, an excessive forward curve of your spine, is a treatable condition that usually doesn’t affect a person’s day-to-day activities unless the curve is severe. An early diagnosis and treatment can address this condition before it gets worse. There are noninvasive treatments that your healthcare provider will offer before surgery. Even after treatment, you’ll need to keep an eye on your posture to make sure the curve doesn’t return. If the curve makes you feel self-conscious, talk to a mental health provider.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.