Myoclonus is an uncontrollable muscle movement that’s sudden and brief. This can happen for a wide range of reasons. Many causes are normal and harmless. But myoclonus can also be a symptom of serious nervous system conditions. Depending why it happens, this symptom may be treatable. Some conditions that cause it may be preventable.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Myoclonus is a brief, sudden muscle movement (like a twitch, jerk or spasm). It happens when muscles incorrectly activate. It usually lasts just a fraction of a second. Myoclonus (pronounced “my-OCK-lon-us”) can affect a single muscle or a group of them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are two main ways it happens:
These muscle movements:
Myoclonus has several possible causes. It may be harmless and be the only symptom you have. It can also be a sign of several medical conditions, some of which are serious.
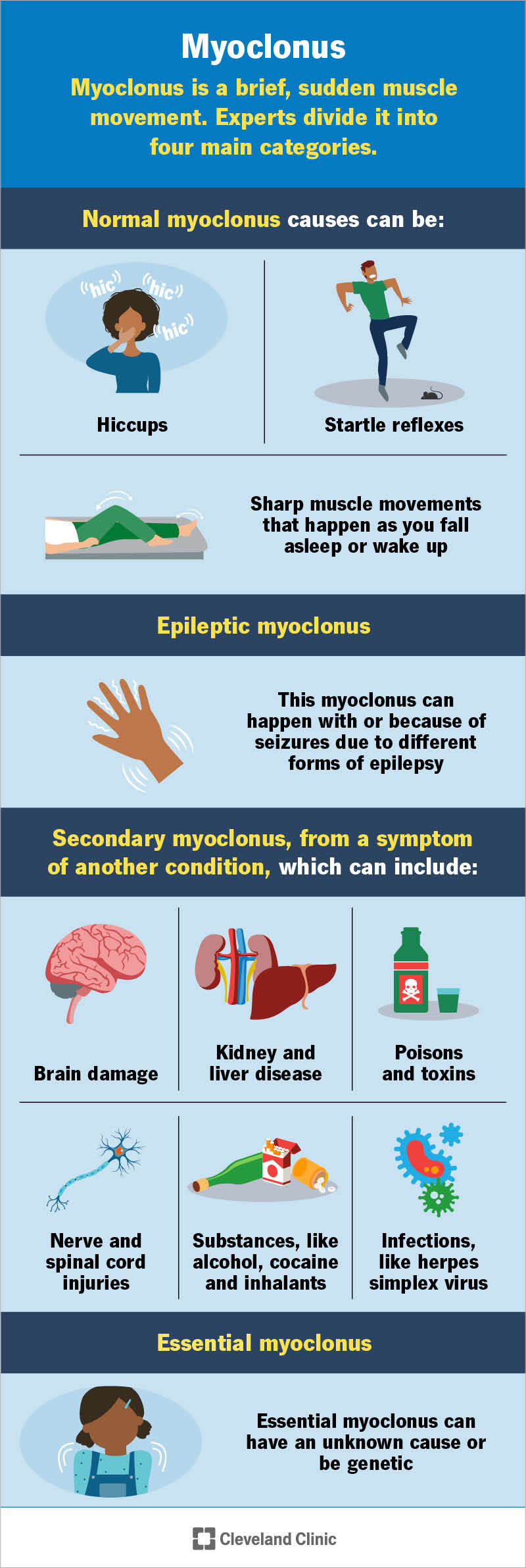
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/myoclonus)
Myoclonus can happen for many reasons. Experts divide it into four main categories.
Some muscle twitches happen for normal reasons. Experts call this physiological myoclonus. Examples include:
Myoclonus can happen as a result of abnormal electrical signals in your brain (also called myoclonic seizures). This type of seizure can occur in different forms of epilepsy, such as Lennox-Gastaut syndrome or juvenile myoclonic epilepsy.
Advertisement
When myoclonus is a symptom of another condition, experts call this secondary myoclonus. Several conditions can cause it, including:
Essential myoclonus happens by itself without an underlying condition or other symptoms. It isn’t harmful and usually doesn’t get worse over time. It can have an unknown cause or be genetic (runs in biological families).
Many other forms of myoclonus happen only in certain age groups or in very specific ways, including:
Typical forms of myoclonus don’t need care. For other types, the best approach can vary widely. Your provider will recommend treatment based on the underlying cause, your medical history and other factors. Because of this, a healthcare provider is the best person to tell you about your options and which ones they recommend.
Treatment may include:
Researchers are currently exploring precision medicine for certain causes of myoclonus. Ask your provider if a clinical trial is an option for you.
You can’t prevent the normal and essential forms of myoclonus.
But some of the secondary causes are preventable. You may also be able to reduce how often epileptic myoclonus happens or how severe it is. Some things you can do include:
Advertisement
If you notice muscle jerks that are new and/or getting more frequent, talk to a healthcare provider. They can help you discover why you’re experiencing this and what you can do about it. Many causes of myoclonus are treatable. Early diagnosis and treatment can make a big difference in keeping disruptions to a minimum.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
