Hypertension (high blood pressure) means your blood is pushing too forcefully against your artery walls. Many people have this condition but don’t know it because it usually has no symptoms. Without treatment, it can lead to a heart attack, stroke, dementia, kidney disease and other issues. Early diagnosis and treatment can be lifesaving.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
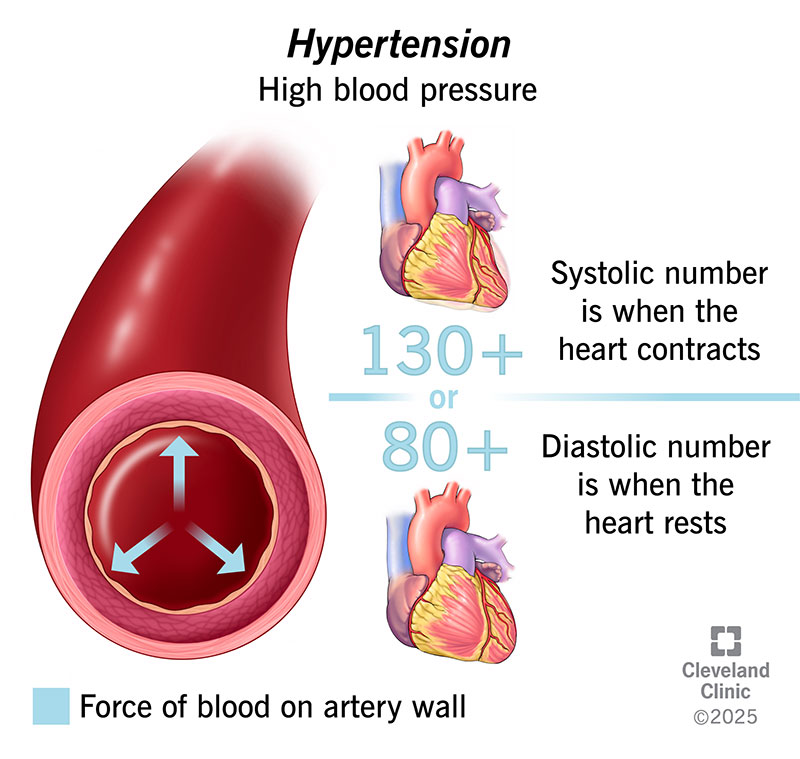
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4314-high-blood-pressure-illustration)
Hypertension, or high blood pressure, means the force of blood pushing against your artery walls is too high. This makes your heart work harder to pump blood through your body. Over time, hypertension damages your arteries and heart. It can lead to serious complications, like a heart attack or stroke. Because high blood pressure usually doesn’t cause symptoms, it’s often known as a “silent killer.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Healthcare providers measure blood pressure (BP) in millimeters of mercury (mmHg). Your reading has two numbers:
What’s considered high blood pressure varies slightly based on where you live. In the U.S., healthcare providers define it as:
In Europe, providers define hypertension as a top number of 140 or higher, or a bottom number of 90 or higher.
High blood pressure is very common. It affects nearly half of all adults in the U.S. It’s a major risk factor for cardiovascular disease.
There are two main types of high blood pressure, based on what’s causing it:
You might also hear about high blood pressure that occurs in certain situations. These types are:
Advertisement
Hypertension usually has no symptoms. You could have it for years without feeling any clues. In fact, the World Health Organization estimates that 46% of adults with hypertension don’t know they have it.
If your blood pressure is extremely high, you may have symptoms like:
This is called a hypertensive emergency. Call 911 or your local emergency services number right away if your blood pressure is 180/120 or higher and you have any of the symptoms above. If you’re pregnant, call for help if your BP is 160/110 or higher with symptoms.
Healthcare providers can’t find a single cause of hypertension for most people. Instead, many factors can come together to make your blood pressure higher. These include:
In some cases, providers can find a specific cause of your high blood pressure, like an underlying condition, medication or substance. Here are some examples:
Untreated hypertension damages your arteries and overworks your heart. Over time, it may lead to:
Advertisement
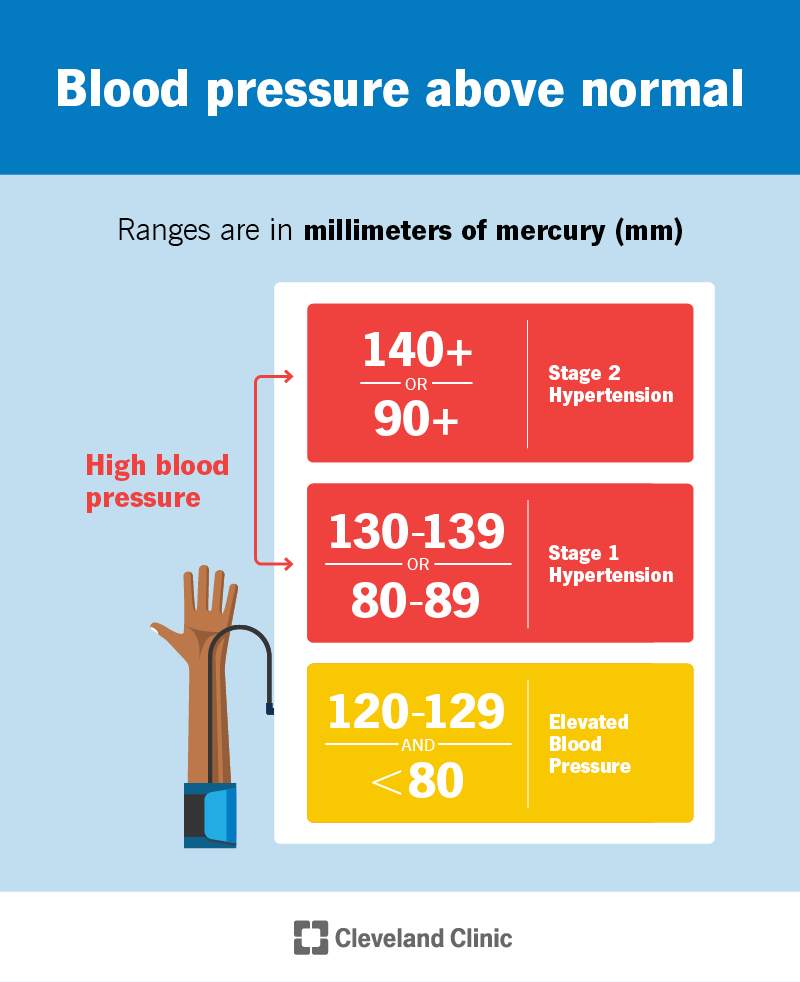
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4314-high-blood-pressure.ashx)
Healthcare providers measure your blood pressure at your yearly check-ups and other appointments. This lets them see if it’s normal or too high. They’ll diagnose you with hypertension if your numbers are high at two separate visits (with at least two readings taken each time).
There are two main stages of hypertension:
On either end of these stages, there are other categories that providers use to guide treatment decisions:
This chart lists these categories and the thresholds for each:
| Category | Top number (systolic BP), in mmHg | And/or | Bottom number (diastolic BP), in mmHg |
|---|---|---|---|
| Normal blood pressure | Below 120 | AND | Below 80 |
| Elevated blood pressure | 120 to 129 | AND | Below 80 |
| Stage 1 hypertension | 130 to 139 | OR | 80 to 89 |
| Stage 2 hypertension | 140 or higher | OR | 90 or higher |
| Severe hypertension | 180 or higher | OR | 120 or higher |
| Hypertensive emergency | 180 or higher, with symptoms | OR | 120 or higher, with symptoms |
| Category | |||
| Normal blood pressure | |||
| Top number (systolic BP), in mmHg | |||
| Below 120 | |||
| And/or | |||
| AND | |||
| Bottom number (diastolic BP), in mmHg | |||
| Below 80 | |||
| Elevated blood pressure | |||
| Top number (systolic BP), in mmHg | |||
| 120 to 129 | |||
| And/or | |||
| AND | |||
| Bottom number (diastolic BP), in mmHg | |||
| Below 80 | |||
| Stage 1 hypertension | |||
| Top number (systolic BP), in mmHg | |||
| 130 to 139 | |||
| And/or | |||
| OR | |||
| Bottom number (diastolic BP), in mmHg | |||
| 80 to 89 | |||
| Stage 2 hypertension | |||
| Top number (systolic BP), in mmHg | |||
| 140 or higher | |||
| And/or | |||
| OR | |||
| Bottom number (diastolic BP), in mmHg | |||
| 90 or higher | |||
| Severe hypertension | |||
| Top number (systolic BP), in mmHg | |||
| 180 or higher | |||
| And/or | |||
| OR | |||
| Bottom number (diastolic BP), in mmHg | |||
| 120 or higher | |||
| Hypertensive emergency | |||
| Top number (systolic BP), in mmHg | |||
| 180 or higher, with symptoms | |||
| And/or | |||
| OR | |||
| Bottom number (diastolic BP), in mmHg | |||
| 120 or higher, with symptoms |
It’s common for both your top number (systolic) and your bottom number (diastolic) to be too high. But it’s also possible for just one to be in the hypertensive range. You might hear your provider use these terms to describe your blood pressure:
Advertisement
Hypertension treatments include medications to lower your blood pressure and changes to your daily habits. Common medicines prescribed for high blood pressure include diuretics, beta-blockers, calcium channel blockers, ACE inhibitors and ARBs. Your provider will recommend the right treatment plan for you based on your blood pressure readings, the cause of your high blood pressure and any other conditions you may have.
In general, changes to your habits — sometimes called “lifestyle changes” — are a key part of treatment for everyone. This is true even if you’re taking medicine. In some cases, providers recommend making changes for a while before starting medicine. It depends on your medical history and risk for a heart attack or stroke.
Changes you can make to lower your blood pressure include:
Advertisement
Doing these things can also help prevent high blood pressure if your numbers are currently in the normal range.
See your healthcare provider for yearly check-ups. They’ll measure your blood pressure and look for changes over time. High blood pressure usually doesn’t cause symptoms or make you feel any different. So, these check-ups are crucial and even lifesaving.
Call your provider if you notice your BP is higher than usual when you check it at home. They may ask you to come in so they can measure it.
If you’re pregnant, call your provider if your BP is ever 160/110 or higher (but if you have symptoms, seek emergency care instead).
Once you’re diagnosed with hypertension, you’ll work closely with your healthcare provider to manage it. It’s important to:
If you have primary hypertension, you’ll need to manage it for the rest of your life. Your healthcare provider will help you do this. Secondary hypertension can often be reversed by treating or removing the underlying cause. Your provider will explain how treatment can help and what to expect.
The months and years go by fast. It’s easy to forget about conditions that you can’t feel. High blood pressure (hypertension) won’t make you feel any different until it starts to damage your body. But catching and treating it early can help you protect your arteries and heart for years to come.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
