Spider veins (telangiectasias) are damaged blood vessels just under your skin that look red, blue or purple. On their own, they’re harmless and don’t cause symptoms. But they may be an early sign of more serious blood flow issues, like chronic venous insufficiency. Your healthcare provider will tailor treatment to your needs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
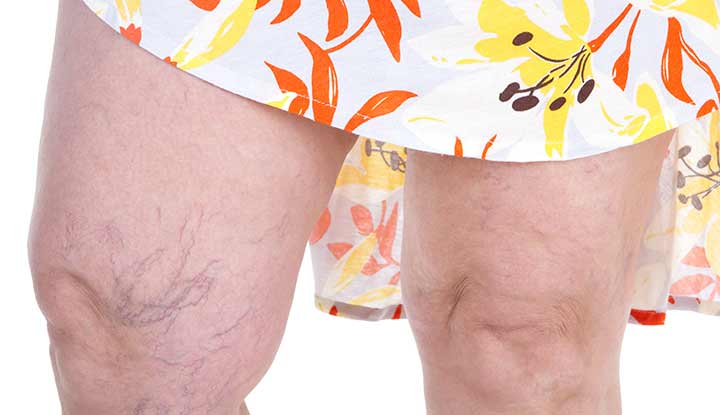
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24567-spider-veins.jpg)
Spider veins (telangiectasias) are damaged, visible blood vessels just beneath your skin’s surface. They typically look red, blue or purple. They may appear in clusters that look like spider webs or tree branches. Spider veins can form anywhere, but they usually develop on your legs, hands or face.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Despite their name, spider veins aren’t actually veins. They’re small, damaged blood vessels that connect to the veins and arteries in your body (otherwise known as capillaries, venules and arterioles).
Spider veins themselves aren’t dangerous. Having spider veins is mostly a cosmetic issue. That means you might not like their appearance, but they won’t harm you. Sometimes, though, spider veins are an early sign of chronic venous insufficiency (CVI). This is a vein disease that can affect your quality of life and lead to complications.
That’s why it’s important to tell a healthcare provider if you notice spider veins. This can help you catch signs of blood flow problems early and get any treatment you need.
Spider veins usually don’t cause symptoms. Even though you can see them on your skin as branch-like clusters of red, blue or purple lines, you probably won’t know that the damaged vessels are there unless you look at them. But it’s common to have spider veins plus varicose veins or other blood flow issues. In those cases, you might experience symptoms, especially after standing for a while. These include:
Advertisement
Treating the spider veins won’t improve these symptoms. Your healthcare provider will discuss treatments for CVI or other blood flow issues that can help you feel better.
In people with darker skin tones, spider veins may look different. The color of the classic blue and red may be more subtle or mistaken for other skin conditions.
Spider veins form when small blood vessels just under your skin weaken and expand. It’s not always clear what causes this to happen. Some known causes include:
You’re more likely to get spider veins if you:
Spider veins on their own rarely lead to complications. But if you also have other conditions, like CVI, you may be at risk for:
To diagnose spider veins, a healthcare provider will:
Your provider will look for signs of CVI to determine if the spider veins signal a more serious blood flow problem. They may run some noninvasive tests, like a vascular ultrasound, to see how blood moves through your legs or other parts of your body.
If you have CVI, your provider may refer you to a vascular surgeon for further evaluation and treatment.
Spider veins don’t necessarily need treatment. But treatments are available if you don’t like how they look. Procedures can close off or get rid of the damaged blood vessels. Options include:
For either treatment, you might need multiple sessions.
It’s important to know that your healthcare provider will treat more serious issues before treating the spider veins. For example, if you have CVI, they’ll suggest medications, procedures and/or surgeries. These treatments can improve blood flow and prevent complications.
Advertisement
Call a healthcare provider if:
If you have spider veins, it may help to ask:
Spider veins usually don’t lead to serious problems. Treatment can get rid of them and help you feel better about your skin’s appearance. You may need treatment again if new spider veins form.
Talk with your healthcare provider about your prognosis (outlook) if you have CVI. They’ll help you understand which treatments you might need and what you can expect.
Self-care can often improve blood flow and prevent new spider veins from forming. Tips include:
Advertisement
Telangiectasia is the medical term for a small, dilated (widened) blood vessel that can form just beneath the surface of your skin or mucous membranes. When telangiectasias appear on your skin, most people call them “spider veins.” But certain medical conditions can also make telangiectasias appear in other areas, like your tongue or the whites of your eyes.
Telangiectasias are sometimes a main sign of a condition. In those cases, the term is built into the condition’s name. Examples include:
Reticular veins, like varicose veins, are actually damaged veins. This makes them different from spider veins. But they’re smaller than varicose veins — around 1 to 3 mm wide. They look bluish in color just beneath your skin. They often twist and turn in different directions or have a zigzag appearance.
Spider veins are common and, on their own, harmless. But they can be a sign of blood flow problems that need treatment. Let your healthcare provider know if any of your blood vessels look or feel different. They’ll find the cause and talk with you about next steps.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Vascular disease may affect your life in big and small ways. Cleveland Clinic’s specialists treat the many types of vascular disease so you can focus on living.
