“Ectropion” is the medical term for outward-turning eyelids. This means your eyelid droops away from your eyeball, which exposes your eye, leading to dryness and irritation. There are several types and causes of ectropion. Treatment for all of them will likely start with some sort of artificial tears or lubrication.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
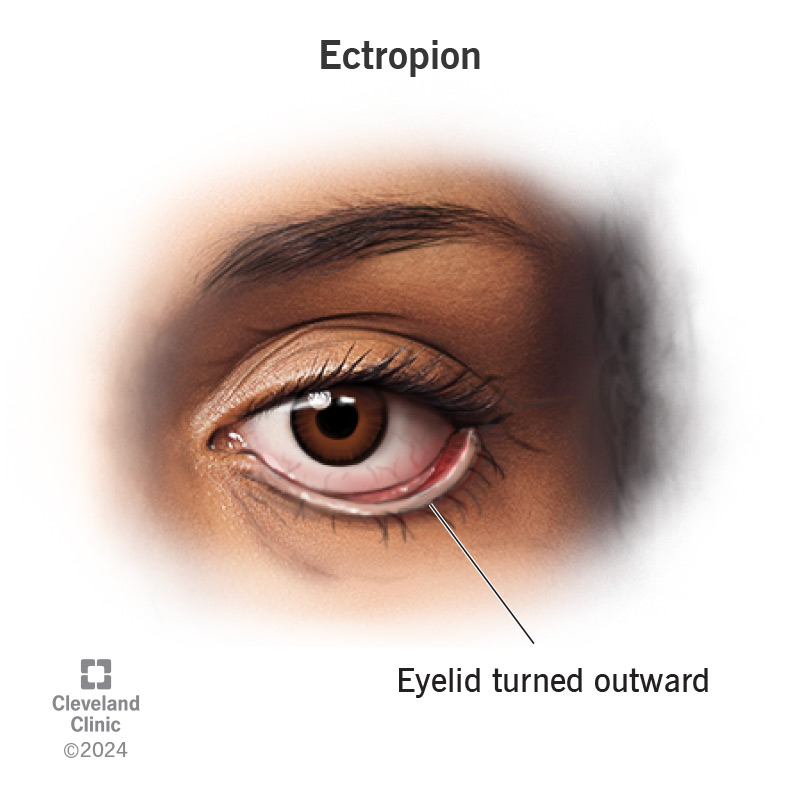
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/ectropion)
Ectropion is a condition that occurs when your eyelid turns outward away from your eyeball. This drooping of your eyelid exposes your eye, causing issues with the drainage of your tears and irritation to the front of your eye. When your eyes aren’t fully lubricated, it can lead to severe dryness and inflammation. Ectropion is the opposite of entropion, the inward turning of your eyelid.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Ectropion can happen to your upper or lower eyelid, but it most often affects your lower lid. It can occur in one or both eyes. If you’ve developed the condition, treatment is available. An eye care specialist may recommend a noninvasive option, like artificial tears. If the problem persists, they may recommend surgery.
There are a variety of types of ectropion that can affect your eyes. They’re broadly divided into groups called congenital (something you’re born with) and acquired (something that happens over time). The congenital type is the least common. There are four acquired types:
Your eyelids protect your eyes and keep them clean. The signs and symptoms of eyelid ectropion happen when your lid droops down, exposing your eye. There’s more opportunity for irritation to occur. Signs and symptoms of ectropion may include:
Advertisement
Causes of ectropion differ based on the type. The types and causes of ectropion are:
Risk factors for ectropion may include:
A healthcare provider will start by asking you about your medical history and performing an eye exam. They’ll probably be able to see ectropion of your eyelid. Sometimes, the diagnosis is subtle, but other times, it may be obvious.
Your lower lid may appear to be lower in position than it should be. The lid may appear to be inside out. Your eye may look redder than it should, especially where the exposure is occurring. Your lower cornea may be visible and may seem irritated or inflamed, a condition called keratitis.
Your provider may pull your eyelid even farther away and count how long it takes to return to its position. This is called the snap-back test. If ectropion is severe, you might have to blink repeatedly to get it to return to position.
Your provider will almost always begin your treatment by prescribing artificial tears or other types of drops or ointments to add moisture to your eye. If lubrication alone doesn’t clear up the condition, they may recommend other treatment options, including:
Advertisement
Some ectropion surgeries may require a skin graft, like surgery to correct scarring that causes ectropion. In some cases, you may need more than one surgery to fix the ectropion completely.
Ectropion is a very treatable condition. If necessary, surgery can cure the condition and make your eyelid muscles stronger.
Without treatment, severe ectropion can lead to scarring or ulcers (sores) on your cornea. This can cause permanent vision loss and even loss of an eye in the worst cases.
Most of the time, you can’t prevent ectropion. But you can take some steps to protect your eyes and eyelids. For instance, you can be careful about how often and how firmly you rub your eyes, taking care not to stretch your skin. Avoid sleeping on your stomach with your face in the pillow, as this will increase the laxity of your eyelids. If you have sleep apnea, wear your CPAP machine. If you think you may have sleep apnea, talk to your primary care doctor to arrange a sleep study.
Advertisement
You can also protect your skin and eyes from harsh sunlight and wear sunglasses. Always wear safety glasses when you need them for work.
If you wear contact lenses, make sure you clean them properly and dispose of them when you should. Always make sure your hands are clean when you’re putting lenses in and taking them out. Try to be gentle with your lids.
Keep regular eye care appointments. Contact your provider about any changes in how well you see or how your eyes look or feel. Signs and symptoms that could cause concern include:
Questions you may want to ask your eye care specialist include:
Your eyelids are an important part of your eye. They protect your eyes and keep them from drying out. If you notice anything different about them, you should contact an eye care specialist. An outward-facing eyelid may not seem significant, but ectropion can cause uncomfortable symptoms in the short term and issues with your vision in the long term. Treatment may be as simple as artificial tears, but see a provider to discuss the best option for you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s ophthalmologists and optometrists have the highest training available. We provide exams, vision correction and care for many eye conditions.
