Tietze syndrome is pain and swelling in the cartilage in your rib cage, at the junction where one of your ribs meets your sternum (costochondral junction). Treatment is with rest and pain relievers. It may take a few weeks to months to heal.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
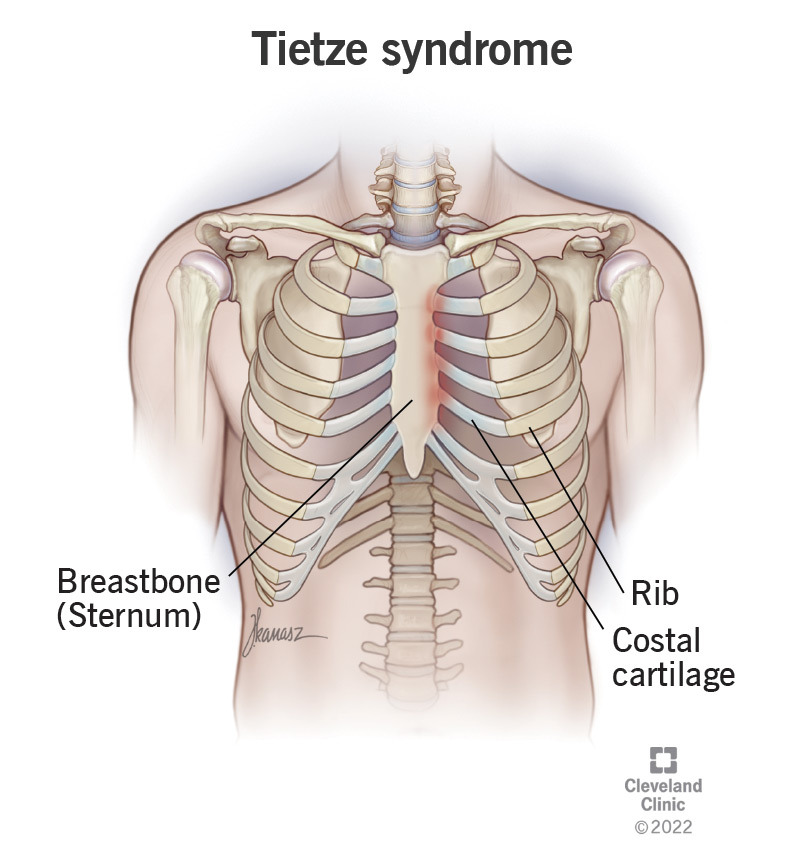
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/tietze-syndrome)
Tietze syndrome (Tietze’s disease) is a rare inflammatory condition that affects the cartilage in your rib cage. It causes musculoskeletal chest pain and swelling at the front and top part of your chest wall.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your upper ribs (the first 10) have cartilage tips (costal cartilage) where they connect to your sternum (breastbone). The joints where these tips connect (costochondral joints) also have cartilage in them.
General inflammation of the cartilage in your rib cage is called costochondritis. But Tietze syndrome is more specific. It typically affects just one of your top four ribs. It’s also distinctive for causing noticeable swelling.
Healthcare providers aren’t sure what causes Tietze syndrome (also called costochondral junction syndrome). But it doesn’t seem to be serious. You can treat it at home with rest and pain relievers.
The most obvious way Tietze syndrome will affect you is by the pain in your chest, which can come on suddenly or gradually. Some say it’s like a dull ache when you’re still, but sharp and gripping when you move or twist your upper body. Coughing, sneezing and exercise can make it worse. You’ll feel it in the front and top of your chest, often on one side. It may also radiate to your arm, shoulder and neck.
Localized swelling is the other major symptom of costochondral junction syndrome. You may see a small, puffy shape somewhere near your upper sternum — most often at your second or third rib. Some people describe it as a “mass” that’s firm to the touch. It may also feel warm and look red or discolored. These are all symptoms of inflammation. Swelling is a distinctive feature of Tietze’s disease, and often the last to fade.
Advertisement
The symptoms of Tietze syndrome happen because the cartilage at that painful spot in your rib cage is irritated and inflamed. But healthcare providers don’t know what causes this, or why it happens in the particular way that it does. Why does it affect just one of your top few ribs, or produce that characteristic swelling? These are things that distinguish Tietze syndrome from regular costochondritis.
Some of the suggested causes include:
You might be more likely to develop Tietze’s disease if you’re recovering from another condition or you have a chronic condition that irritates or weakens the cartilage in your rib cage. Examples include:
If you go to your healthcare provider with chest pain, they’ll check first to make sure it isn’t a heart attack. After ruling that out, they’ll carefully review your symptoms and examine your chest. They’ll follow up with imaging tests to look for inflammation and signs of injury inside your chest. Healthcare providers diagnose Tietze’s disease when they’ve ruled out other possible causes for your symptoms.
Tests might include:
When your soft tissues are inflamed, they need time and rest to recover. Healthcare providers usually suggest just that. Over-the-counter pain relievers can help relieve the pain and swelling. Providers often recommend NSAIDs (nonsteroidal anti-inflammatory drugs). You shouldn’t need to miss school or work, but take it easy and avoid vigorous activities while you recover. You can gradually increase your activity as you start to feel better.
Consult your provider if you still feel you need to take NSAIDs after 10 days. Taking them for too long can have side effects. They might suggest switching to acetaminophen, or they might give you a cortisone injection at the site of the inflammation. Some people might need treatment to stop sneezing, coughing or vomiting before their chests can heal. Keep in touch with your provider about your recovery.
Advertisement
Costochondral junction syndrome is a temporary condition, and you can expect to make a full recovery. Most people recover in a few weeks, but some bodies take longer. Sometimes, the swelling lingers for several months after the pain goes away. Occasionally, Tietze’s disease comes back after seeming to go away. Different causes and risk factors might make Tietze syndrome more persistent in some cases than others.
It’s scary to experience chest pain, especially when you don’t know the cause. But Tietze syndrome isn’t cause for worry. It might be uncomfortable for a while, but you can treat it at home until it gets better.
The biggest challenge with Tietze’s disease may be getting the right diagnosis. It’s rare and resembles many other conditions. Your provider will have to rule these out before diagnosing Tietze syndrome.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From sudden injuries to chronic conditions, Cleveland Clinic’s orthopaedic providers can guide you through testing, treatment and beyond.
