Chronic limb-threatening ischemia is an advanced stage of peripheral artery disease. It means very little blood can reach part of your leg or foot due to plaque buildup (atherosclerosis) in your arteries. Symptoms include leg or foot pain while resting, skin wounds and gangrene. You need treatment right away to restore blood flow.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
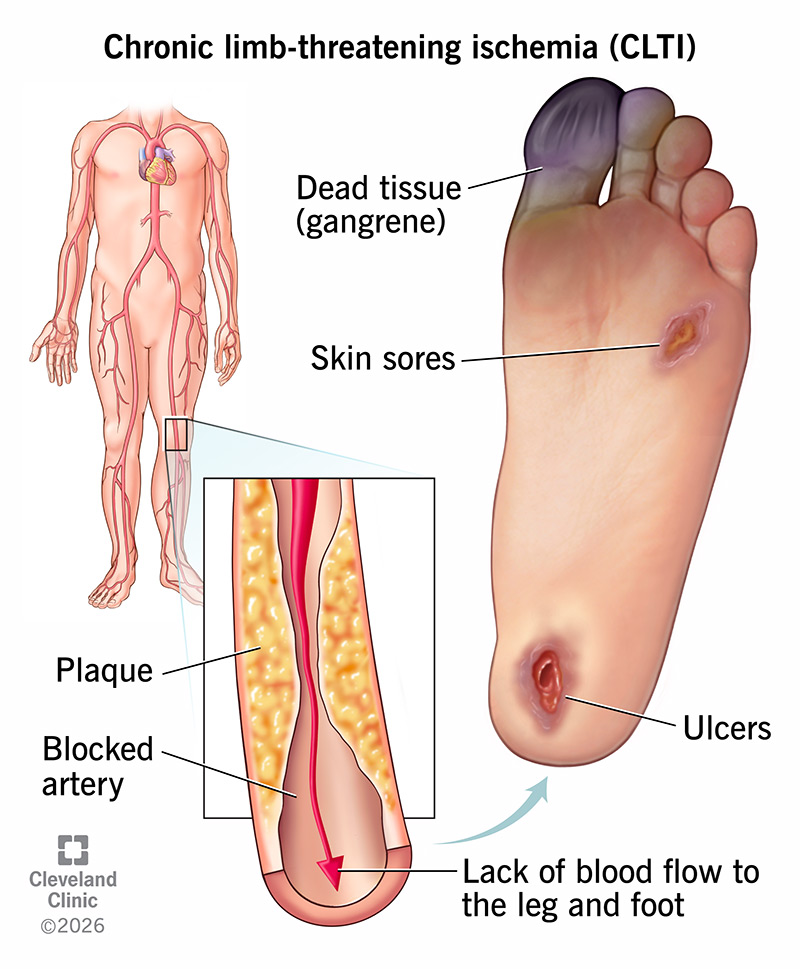
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23120-chronic-limb-threatening-ischemia-illustration)
Chronic limb-threatening ischemia (CLTI), formerly called critical limb ischemia, is severely blocked blood flow to your leg or foot. It’s an advanced stage of peripheral artery disease (PAD). You may have intense pain even when you’re resting and open wounds on your affected limb.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
About 1 or 2 out of every 10 people with PAD develop CLTI. This serious condition increases your risk of heart complications, amputation and death.
Seek medical care right away if you think you have CLTI. Prompt treatment can save your limb and your life.
The most common symptom is foot or leg pain that occurs at rest. Often, this pain is worse when you elevate your leg or lie flat. It may wake you up at night. You might find that if you hang your leg off the edge of your bed or get up and walk around a small amount, it may relieve the pain.
Some people don’t feel any pain but have other symptoms, like:
Healthcare providers call this condition “chronic” because symptoms are present for more than two weeks. But you shouldn’t wait to seek care. If you have any of these symptoms, seek medical attention immediately.
Severe plaque buildup in your peripheral arteries (in any of your limbs, but typically your legs) causes CLTI. This process is called atherosclerosis. As your arteries narrow, less blood can reach certain tissues in your leg or foot. It’s harder for these tissues to remain healthy and strong, or to heal, without enough blood flow.
Advertisement
Plaque buildup is also responsible for the earlier stages of PAD, like leg cramps or achiness when you’re walking or exercising. But with CLTI, the plaque severely restricts blood flow. This means very little blood can get where it needs to go. That’s why CLTI symptoms are much more severe. Body tissues can even begin to die, or they won’t heal when damaged.
Anyone with PAD can develop chronic limb-threatening ischemia. You have an increased risk if you:
You can lower your risk of CLTI by working with a healthcare provider to manage peripheral artery disease in its earlier stages. This may involve:
Without treatment, CLTI can lead to limb loss (amputation). Having CLTI also raises your risk for a heart attack, stroke or dying. That’s because the same kind of plaque that builds up in your leg arteries can also build up in other arteries — including those that supply blood to your heart or brain.
Your healthcare provider will do a physical exam and talk with you about your symptoms. They’ll check your pulse at several different points along both arms and legs. If your provider thinks you may have critical limb ischemia, they’ll run some noninvasive diagnostic tests, like:
To help plan treatment, your provider may do imaging tests like a vascular ultrasound, CT angiogram, MRA or catheter angiogram.
To treat CLTI, your healthcare provider will do one or more procedures or surgeries to restore blood flow and heal skin wounds. If there’s severe tissue damage that isn’t salvageable, you may need surgery to remove toes or even some or all of a limb. In addition to treatment for the affected limb, you’ll likely also need to take some medicines and change some habits to lower your risk of future complications.
Advertisement
Your provider may recommend one or more of the following treatments:
Your provider may prescribe medicines to help keep the arteries open and lower your risk of a heart attack or stroke. Possible medicines include:
Advertisement
If you smoke, your provider will give you guidance on how to quit and suggest programs or medication to help.
Your provider will also talk with you about footwear and how to care for your feet. They may recommend using orthotics, like custom-made shoe inserts. These can help relieve pressure on certain parts of your foot. This promotes wound healing and prevents new wounds from forming.
Contact a provider right away if you think you have CLTI. The sooner you get treatment, the better.
Treating CLTI takes time. You’ll have many appointments and follow-up visits — often with different types of providers, like vascular surgeons, podiatrists, dietitians and physical therapists. These visits are all crucial for your healing. Be sure to tell your providers if it’s hard for you to stick with your treatment plan or get to your appointments. They can offer resources to help.
Treatment can help save your limb and your life. But each person is different, and many factors affect your outlook. These include:
Your healthcare provider can help you understand what’s possible in your situation. It’s important to know that chronic limb-threatening ischemia is a serious condition that can lead to limb loss or death. For example, up to 1 in 3 people with CLTI need a major amputation (above the ankle) within one year of diagnosis.
Advertisement
But there are also many reasons to have hope. Treatments continue to improve. Surgeons are finding more and better ways to restore blood flow in people who have this condition. This means it’s often possible to heal tissue damage, feel better and keep your limb.
If you need an amputation, your care team will be there for you. They’ll connect you with resources to help you adjust both physically and emotionally.
Learning you have a condition that threatens the health of your leg or foot can feel terrifying. You might find yourself thinking about all the “what-ifs.” Or wondering how your daily life might change.
As with any new diagnosis, there’s a lot to take in. But you don’t have to try and figure it all out on your own. Your care team is prepared to help you understand what’s happening. They’ll help you develop a new routine as you go through treatment and recovery. Even something as small as writing out an hourly schedule — like when to take your medicines or do foot care — can offer some comfort and a sense of control.
Remember, too, that it’s common for conditions affecting your body to take a toll on your mental health. If you’re feeling very sad or anxious, you don’t have to keep carrying those thoughts alone. Your provider can connect you with counselors, support groups and others who can help.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Plaque in your blood vessels can cause tingling, pain and numbness. Cleveland Clinic’s experts treat circulatory problems, including peripheral artery disease.
