Onycholysis is when your nail separates from its nail bed. It often appears after an injury to your nail, but it may have other causes, including fungi. Treatment may only involve cutting away the separated nail as it grows out, or you may need to take antifungal medications or stop using certain nail products.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
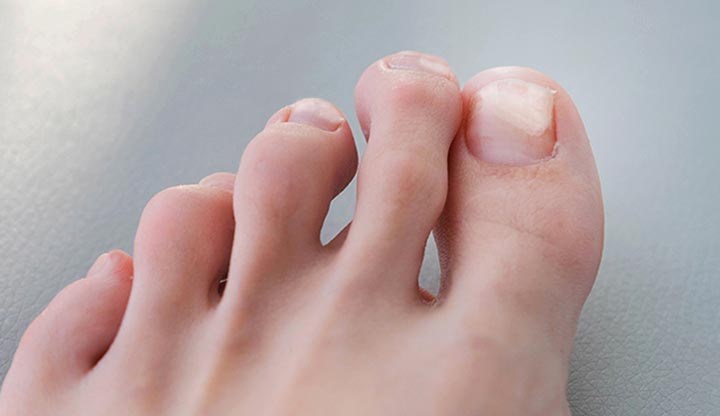
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22903-onycholysis_1365915666)
Onycholysis (on-uh-coll-uh-sis) is when a nail (nail plate) on your fingers or toes separates from the skin on which it rests (the nail bed). It typically only affects one nail.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Onycholysis affects everybody. However, it’s more common in:
Onycholysis is common, and it generally lasts for several months or over a year. Any conditions that affect the skin underneath your nails eventually cause onycholysis.
Onycholysis causes your nail to peel away from the nail bed. It usually doesn’t cause any pain.
Symptoms of onycholysis include:
Onycholysis usually isn’t painful, but what causes your onycholysis may be painful or irritating. If you have onycholysis due to injuries or fungal infections, you may experience pain and irritation.
The following are common causes of onycholysis:
Advertisement
Onycholysis rarely affects all of your nails. The following may cause onycholysis in all of your nails:
No, onycholysis isn’t a fungal infection. However, fungal infections can sometimes cause onycholysis.
Depending on what causes your onycholysis, it may be contagious. Onycholysis caused by an injury, nail psoriasis or reaction to a medication or chemical isn’t contagious. However, onycholysis caused by a fungus may be contagious.
A person with an infection can spread the fungus to someone else through skin-to-skin contact. You can also get nail fungus by touching an infected surface (indirect contact), like walking barefoot around public pools or showers or by sharing items like towels, nail clippers and nail scissors.
Onycholysis is easy to recognize, so you don’t necessarily need a healthcare professional to diagnose it, especially if you know its cause.
If you don’t know what’s caused your onycholysis, seeing your healthcare provider is a good idea. They’ll look closely at your affected nails to evaluate your symptoms.
Your healthcare provider may perform several tests to diagnose onycholysis. The tests may include:
Advertisement
There isn’t a cure for the section of your nail that’s detached from the nail bed — you can’t reattach it. But treatment can keep new nail growth attached to your nail bed.
If you have onycholysis because of an injury, the detached part of your nail will eventually grow out. Use nail clippers or nail scissors to remove your affected nail as it grows out.
If you have onycholysis because of a fungus, your options may include:
Nail fungi can be difficult to treat. It’s important to finish your full course of medicine. If you stop too soon, the fungus that caused your onycholysis may come back and be harder to treat.
The following tips can help you take care of your nails if you have onycholysis:
Advertisement
While essential oils are safe for most people, it’s a good idea to check with your healthcare provider before trying them. You may be at risk of developing an allergic reaction.
If you and your healthcare provider can determine the cause of your onycholysis, your nails will slowly but surely regrow. Your fingernails grow slowly, and your toenails grow even slower. It may take up to six to nine months for your fingernails to grow completely out, and it may take 12 to 18 months for your toenails to grow completely out.
The following tips can help you prevent onycholysis:
Advertisement
Contact your healthcare provider if:
Onycholysis causes your nails to pull up from nail beds. It usually isn’t painful, but can be contagious if a fungus is the cause.
It’s important to pay attention to your nails. If you haven’t experienced an injury or trauma to your affected nails, it’s a good idea to contact your healthcare provider as soon as you notice onycholysis. You may have a fungus, or your onycholysis may be a symptom of a more serious condition.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
