Nail psoriasis is an autoimmune condition. It causes discoloration, pitting and changes in your fingernails and toenails. There isn’t a cure, but treatments can alleviate related symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Nail psoriasis is an autoimmune disease that causes your skin cells to reproduce quickly. It’s a type of psoriasis that affects the nails on your fingers and toes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Nail psoriasis typically appears along with a psoriatic rash on other parts of your body.
Anyone can get nail psoriasis. However, you may be more likely to develop nail psoriasis if you:
Nail psoriasis is common. It affects over 50% of all people with psoriasis and around 86% of all people with psoriatic arthritis.
No, nail psoriasis isn’t a fungus. Nail psoriasis is an autoimmune disease. Your immune system overreacts, which leads to new skin cells growing too fast.
Symptoms of nail psoriasis include:
Advertisement
Some of these symptoms may result in discomfort, tenderness or pain that can affect your comfort or ability to stand, walk or use your hands.
Nail psoriasis is an immune system problem. Typically, new skin cells grow every 28 to 30 days. However, in people with psoriasis, new cells grow and move to the skin surface every three to four days, which creates a skin rash. In some people with psoriasis, it affects their nails in addition to their skin or other parts of their bodies.
Nail psoriasis isn’t contagious. You can’t spread nail psoriasis to another person through skin-to-skin contact.
Your healthcare provider can typically diagnose nail psoriasis after a physical exam. They’ll examine your affected areas to look for common signs of nail psoriasis. They’ll also ask about your symptoms and your family history.
Once your healthcare provider has diagnosed nail psoriasis, they may use the nail psoriasis severity index (NAPSI) to grade its severity. The NAPSI uses imaginary lines to divide your nail into four even sections (quadrants). Your nails receive a 0-4 score based on the presence of any nail psoriasis symptoms in each of the quadrants. Your healthcare provider will then add the scores together. A low number means your nail psoriasis is mild, and a high number means your nail psoriasis is more severe.
People with nail psoriasis may develop a number of symptoms. Providers use NAPSI to determine the severity of the condition.
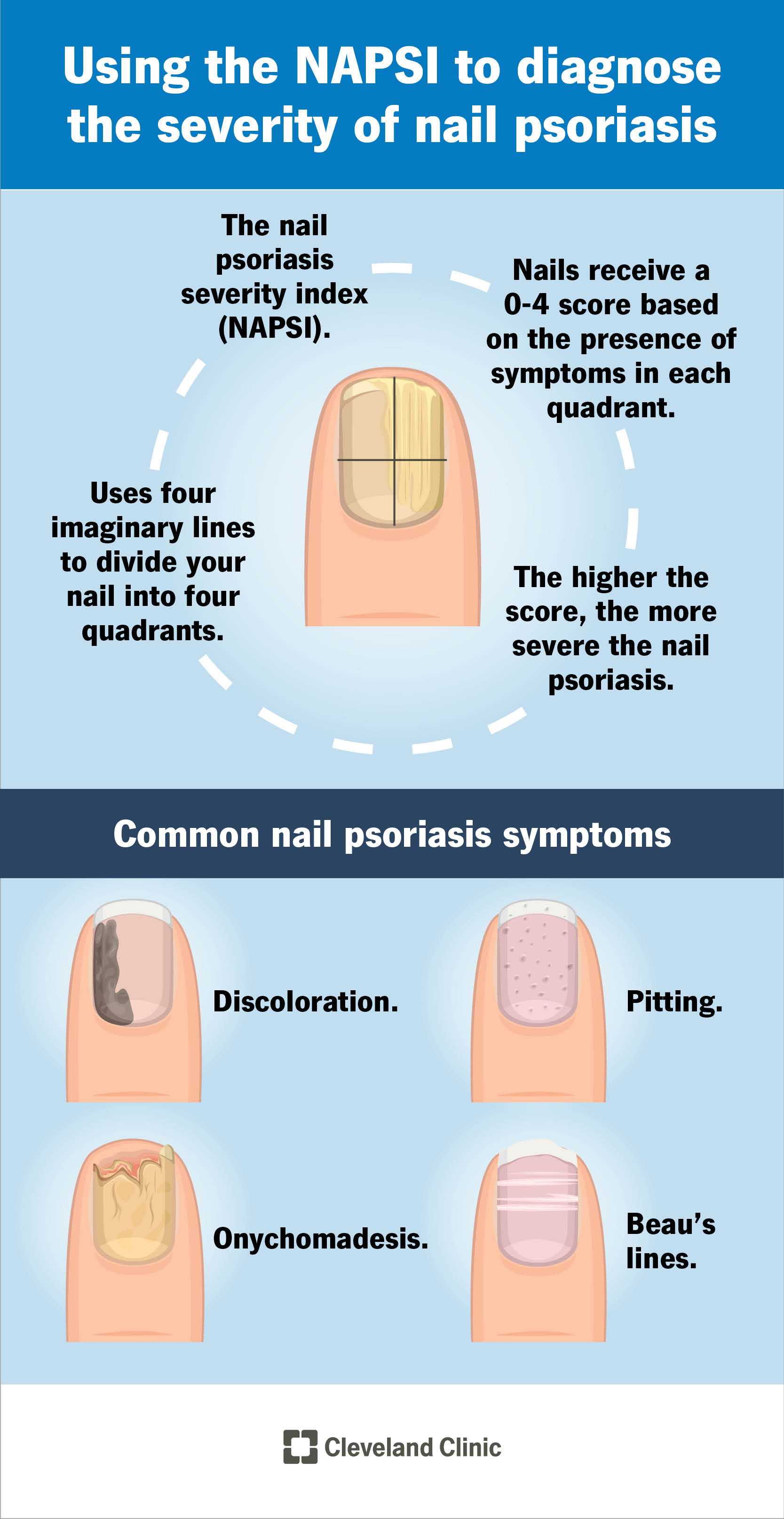
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22841-nail-psoriasis.jpg)
If there’s any doubt about your symptoms, your healthcare provider may order a potassium hydroxide (KOH) preparation or fungal culture to rule out a fungus as the cause of your symptoms. If those test results aren’t clear, a fungus test known as a periodic acid-Schiff (PAS) stain can also determine the presence of a fungus.
There isn’t a cure for nail psoriasis. It’s a long-lasting (chronic) condition, which means flare-ups can occur throughout your life. You may have flare-ups and times when the symptoms go away (remission). Treatments can provide relief for your symptoms.
Nail psoriasis is often resistant to some treatment options, so it can be challenging to manage without standard treatment. You and your healthcare provider may have to explore different treatment options, including:
Advertisement
There are several home remedies and tips that can help manage the symptoms of nail psoriasis.
While home remedies are safe for most people, it’s a good idea to check with your healthcare provider before trying some of the following options. You may be at risk of developing an allergic reaction.
Advertisement
It’s also a good idea to:
If your nail psoriasis makes you feel self-conscious or embarrassed, you may gently buff your nails and apply nail polish to hide any pits or discoloration and improve your nails’ appearance. However, avoid using fake nails. Fake nails can damage your actual nails.
Nail psoriasis may flare up and go into remission throughout your life. However, it can generally be well managed with treatment.
If you have nail psoriasis, you may be at a higher risk of:
There isn’t any way to prevent nail psoriasis. If you have nail psoriasis, it may come and go throughout your life. Treatments can reduce symptoms, even in people with severe nail psoriasis.
If you have nail psoriasis, the best way to take care of yourself is to:
Advertisement
Contact your healthcare provider if:
Nail psoriasis is an autoimmune disease that causes discoloration, pitting and changes in the structure of your nails. It can make you feel self-conscious, though you can buff your nails and apply nail polish to improve their appearance. Nail psoriasis isn’t contagious, and treatments can help your symptoms improve.
It’s important to pay attention to your nails. Contact your healthcare provider as soon as you notice changes to your nails.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Coping with psoriasis can be frustrating and distressing. Cleveland Clinic experts offer personalized treatment to help you manage this chronic condition.
