Medulloblastoma is a cancerous brain tumor that starts near your brainstem in your cerebellum. The tumor is fast-growing and can spread to other areas of your brain and spinal cord. Medulloblastoma is more common in children than adults. Treatments include surgery, radiation therapy and chemotherapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
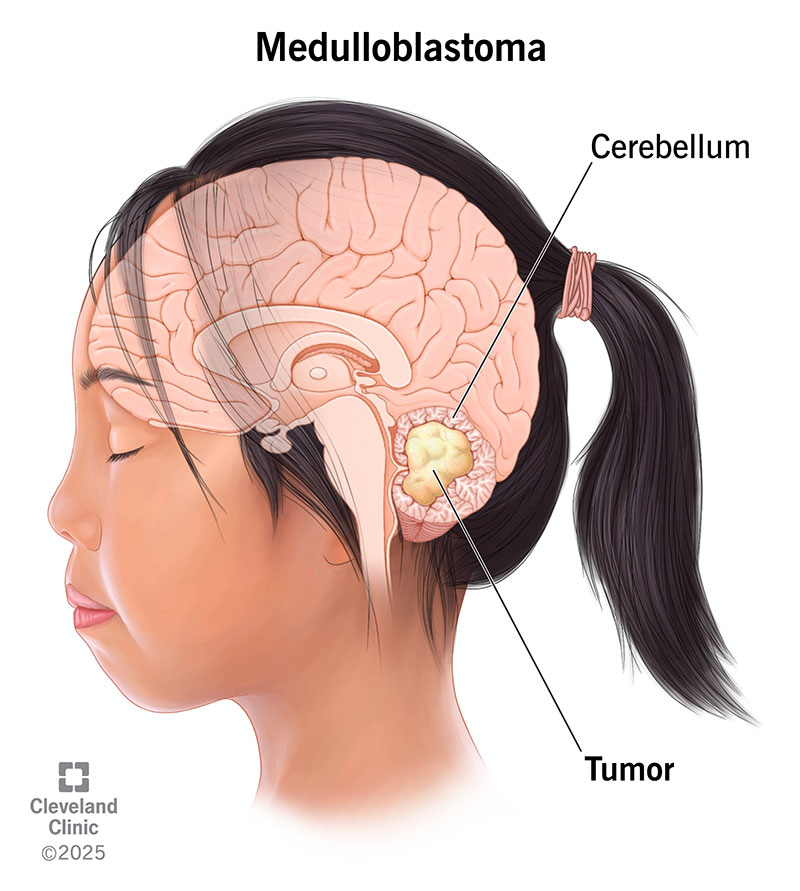
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/medulloblastoma)
Medulloblastoma is a cancerous tumor of your central nervous system (CNS). It forms in the cerebellum, an area near the back of your brain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Medulloblastoma mostly affects children and teens under the age of 16. Though rarer in older individuals, it can occur in adults as well. Medulloblastoma in adults is usually diagnosed between the ages of 20 and 45.
This type of cancer is rare, affecting about 437 children and adults in the U.S. each year. But it is the most common type of brain tumor in children. Most cases are diagnosed between the ages of 5 and 9.
Medulloblastomas usually grow quickly. The cancer can spread to other parts of your brain and spinal cord through cerebrospinal fluid (a clear fluid that protects your brain and spinal cord from injury).
Medulloblastoma symptoms can vary depending on several factors, including your age, the size of the tumor and its stage of development. These symptoms may depend on the location of the tumor or because of pressure buildup inside of your skull. Warning signs may include:
Researchers don’t know exactly why medulloblastoma happens. But there are certain genetic disorders that could increase your or your child’s risk for developing the condition, including:
Advertisement
Your healthcare provider will talk with you about symptoms and review your medical history in detail. If they suspect medulloblastoma, they’ll recommend tests to confirm your diagnosis.
There are a few different tests that can help your healthcare provider make a diagnosis. These tests, from least to most invasive, might include:
It depends on many factors, including your age, overall health and the size of the tumor. The most common medulloblastoma treatment involves surgery followed by chemotherapy, radiation therapy or both.
Length of treatment can vary from person to person. Those who undergo any type of brain surgery usually need at least four to eight weeks to recover. For chemotherapy or radiation therapy, treatment could last several weeks or several months, depending on the case. To learn more about your or your child’s estimated treatment or recovery time, talk with your healthcare provider.
If you or your child develops a combination of symptoms like headaches, nausea, confusion or vision changes, schedule an appointment with a healthcare provider. Those who are already undergoing medulloblastoma treatment should inform their healthcare provider about any side effects. They can help you manage your symptoms and ease your discomfort.
Advertisement
Your team of medical experts may include:
They’ll create a personalized treatment plan according to your specific needs.
In many cases, yes. While medulloblastoma has the potential to spread throughout your entire nervous system, many people can be cured. There’s a higher chance of survival if the medulloblastoma hasn’t spread to other parts of your brain and spinal cord.
The five-year medulloblastoma survival rate is over 80%. This means that over 80% of all people diagnosed with medulloblastoma are still alive five years later. Researchers base these numbers on medulloblastoma outcomes in the past.
But keep in mind, survival rates can’t tell you what will happen in your situation. To better understand survival rates and what they mean for you, talk to your healthcare provider.
A brain tumor diagnosis is physically, mentally and emotionally taxing. And when it affects your child, it’s unthinkable. But there are effective treatments that offer hope. Ask your healthcare provider about clinical trials, which are new treatments that aim to improve outcomes. Also, talk to your healthcare provider about the resources available to you and consider joining a support group. Being around others who are going through the same thing can offer insight and comfort as you navigate this difficult time.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you learn you have a skull base tumor, you’ll want the best care from the best providers. Cleveland Clinic is here to help.
