Mirizzi syndrome is a rare complication of chronic gallstone disease. It happens when a large gallstone or cluster of stones gets stuck in the gallbladder or cystic duct. This causes swelling that can block the flow of bile. Mirizzi syndrome can cause jaundice, inflammation and infection. Treatment usually involves laparoscopic surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
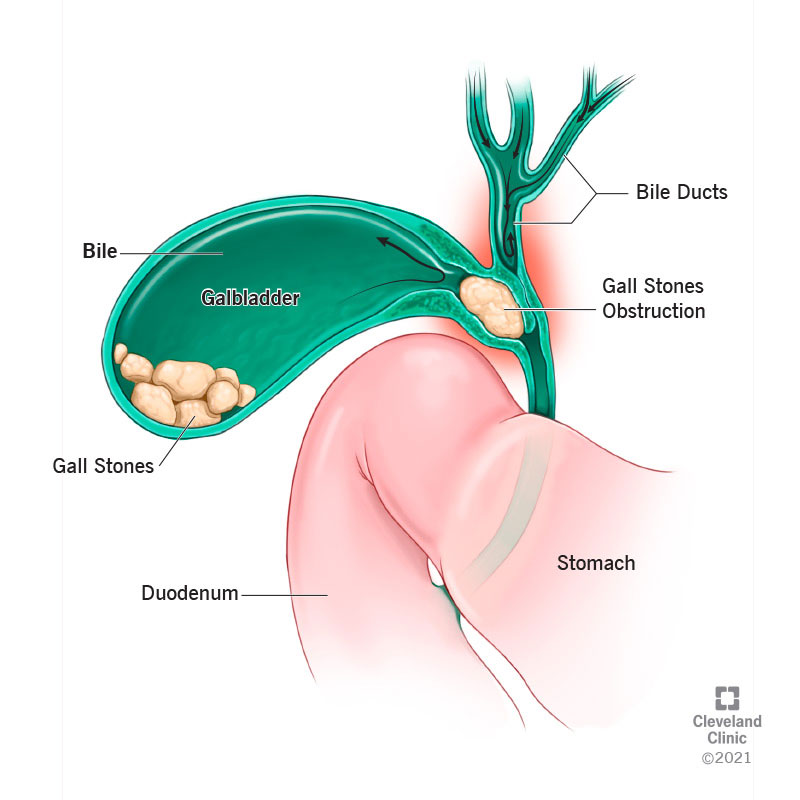
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22092-mirizzi-syndrome.ashx)
Mirizzi syndrome is a rare complication of gallstone disease. Gallstones are concentrated bile crystals that form in your gallbladder. They usually don’t cause symptoms. But in some cases, gallstones can block your bile ducts — the passageways that lead from your gallbladder to your liver.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Mirizzi syndrome causes this blockage in a particularly unusual way:
Your gallbladder receives and stores bile from your liver and releases it into your small intestine through branching passageways called ducts. Sometimes, gallstones wander into the ducts and grow big enough to block the flow of bile. With Mirizzi syndrome, a duct becomes blocked from the outside when a gallstone within your gallbladder or one of the other ducts becomes so enlarged that it presses on the duct next to it.
Healthcare providers classify Mirizzi syndrome into five types:
| Mirizzi syndrome type | What it means |
|---|---|
| Type I | One or more gallstones stuck in your gallbladder or in your cystic duct (the tube that carries bile from your gallbladder) press on a nearby duct, blocking the flow of bile. |
| Type II | You have a fistula (hole) in your bile duct. The hole is less than one-third of your bile duct’s circumference. |
| Type III | You have a fistula in your bile duct. The hole involves up to two-thirds of your bile duct’s circumference. |
| Type IV | You have a fistula in your bile duct that completely destroys your bile duct wall. Your gallbladder fuses (sticks) to your bile duct. |
| Type V | You have a fistula in your bile duct in addition to any other Mirizzi type (I - IV). |
| Mirizzi syndrome type | |
| Type I | |
| What it means | |
| One or more gallstones stuck in your gallbladder or in your cystic duct (the tube that carries bile from your gallbladder) press on a nearby duct, blocking the flow of bile. | |
| Type II | |
| What it means | |
| You have a fistula (hole) in your bile duct. The hole is less than one-third of your bile duct’s circumference. | |
| Type III | |
| What it means | |
| You have a fistula in your bile duct. The hole involves up to two-thirds of your bile duct’s circumference. | |
| Type IV | |
| What it means | |
| You have a fistula in your bile duct that completely destroys your bile duct wall. Your gallbladder fuses (sticks) to your bile duct. | |
| Type V | |
| What it means | |
| You have a fistula in your bile duct in addition to any other Mirizzi type (I - IV). |
Mirizzi syndrome is rare. Because it’s so rare — and because it shares symptoms with other common conditions — surgeons don’t often diagnose it until they do gallstone surgery. Surgeons identify Mirizzi syndrome in up to 2.5% of people having their gallbladder removed.
Symptoms of Mirizzi syndrome fall into three categories:
These symptoms aren’t specific to Mirizzi syndrome, but they’re enough for your provider to suspect gallstones with complications. Not everyone will have all of these. If you do, it points to an issue with your biliary system, but not necessarily Mirizzi syndrome.
Advertisement
Mirizzi syndrome happens when a gallstone blocks a bile duct from the outside. Here’s how it works: A stuck gallstone (or cluster of gallstones) causes so much swelling that it presses on your common bile duct (the tube that carries bile from your liver and gallbladder to your small intestine) or your common hepatic duct (the tube that carries bile from your liver to your small intestine).
To visualize how this happens, think of your gallbladder as a pear. A pear has a bulb-like body that tapers at the top, puffs out at the neck, then continues into a stem. The bulb-like body is your gallbladder’s pouch, the neck is your infundibulum (Hartman’s pouch), and the stem is your cystic duct.
Your gallbladder’s pouch, neck and cystic duct are all narrower places where a gallstone could get stuck. These structures also lie close beside each other — closer in some people than in others.
Mirizzi syndrome can lead to complications like:
Healthcare providers use a variety of tests to diagnose gallstone disease. First, they’ll do a physical exam by pressing on your belly to feel for signs of swelling. They’ll also ask about your symptoms and health history.
If you have signs of infection or jaundice, your provider may run blood tests like:
Your provider will also need to run some imaging tests, which might include:
Surgery is the go-to treatment for Mirizzi syndrome. But there isn’t a standard procedure to manage it. Instead, surgery will be specific to your condition.
In most cases, Mirizzi syndrome management involves gallbladder removal and repair of the blocked duct. In some cases, your surgeon may also remove blocked bile ducts or use stents to open them up. Your surgeon may use a minimally invasive (laparoscopic) or open surgery (laparotomy) approach.
Surgery for Mirizzi syndrome can be challenging because inflammation makes it difficult to see. Accidental injury to your bile ducts during surgery could lead to complications like:
Advertisement
General surgical complications may include:
Mirizzi syndrome prognosis (outlook) is usually good with surgery. The key is to treat it early enough to avoid long-term effects.
More damage to your organs and bile ducts means a more complicated surgery. And the more complicated your surgery, the more likely there will be a longer recovery time. But overall, most people live well without their gallbladder.
You can’t always prevent Mirizzi syndrome. But you might be able to reduce your risk by limiting things that cause gallstones like high-cholesterol foods. Ask your healthcare provider if there are any other specific things you can do to prevent bile duct blockages.
Tell your healthcare provider if you develop sudden, severe abdominal pain along with chills, nausea, fever or signs of jaundice (like dark pee or light-colored poop).
Symptoms of sepsis, like fast heart rate, sweaty skin and shortness of breath, also warrant immediate medical care. Sepsis is a life-threatening emergency that can happen after surgery. If you develop these symptoms, don’t wait. Seek medical care right away.
Mirizzi syndrome is associated with an increased risk of gallbladder cancer. But it’s not necessarily a contributing cause.
Advertisement
Experts suspect that the same conditions that lead to Mirizzi syndrome — that is, chronic inflammation and sludgy bile that sits too long in your gallbladder — also lead to cancer. Statistically, between 5% and 28% of people with Mirizzi syndrome turn out to have gallbladder cancer.
Mirizzi syndrome is treatable, but your risk increases the longer you wait to start treatment. Mortality (death) associated with Mirizzi syndrome is between 5% and 30%. It can come from systemic infection (sepsis), liver failure or associated gallbladder cancer.
Maybe you have the occasional upset stomach, especially after eating. But waking up with persistent abdominal pain, fever and nausea could mean there’s something bigger at play. It’s possible to have gallstones and not know it. But when they grow large enough to block a bile duct, symptoms can get worse and much more frequent. If something doesn’t feel right, don’t wait. The sooner you seek medical care, the better.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have issues with your digestive system, you need a team of experts you can trust. Our gastroenterology specialists at Cleveland Clinic can help.
