Gardner syndrome (Gardner’s syndrome) is a rare inherited disorder. People with Gardner syndrome typically have hundreds of colon polyps that may become colon cancer. They often have extra teeth and noncancerous tumors in their bones and intestines and on their skin.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
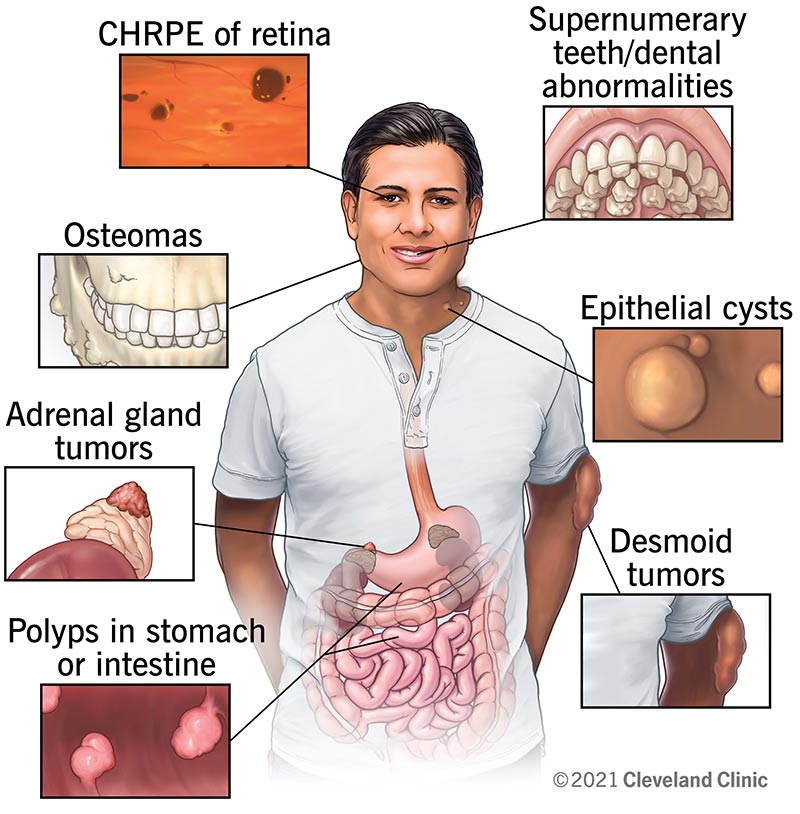
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/22013-gardner-syndrome)
Gardner syndrome (Gardner’s syndrome) is a rare inherited disorder. People with Gardner syndrome have unusual growths throughout their bodies, including hundreds of colon polyps that may become colon cancer. Without treatment, nearly everyone with Gardner syndrome develops colon cancer. They may also have noncancerous tumors that may appear in their bones, intestines, skin and other soft tissues. They’re also at risk for several other conditions, including other cancers.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Gardner syndrome is rare. It affects 1 in 1 million people in the U.S.
Gardner syndrome is an inherited disorder. Most people with Gardner syndrome have at least one biological parent who also has the condition.
Gardner syndrome symptoms change over time. People with this condition may develop symptoms as children, including:
Multiple colon polyps are a common Gardner syndrome symptom. Colon polyp signs may not develop until people are teenagers and the condition is very advanced.
People with Gardner syndrome have an increased risk of developing the following conditions:
Experts know Gardner syndrome is an inherited disorder that happens when people inherit an abnormal APC gene. This gene is a tumor suppressor gene that regulates cell growth and prevents cells from dividing and multiplying too quickly. Most people with Gardner syndrome have at least one biological parent who also has the condition.
Advertisement
Gardner syndrome causes many different symptoms. Healthcare providers may do the following tests to diagnose Gardner syndrome:
That depends on your signs and symptoms. For example, having extra teeth is an early sign of Gardner syndrome. If you have extra teeth, you may need dental procedures to remove extra teeth and realign other teeth.
If you have desmoid tumors, you may receive chemotherapy to shrink them or treatment to keep these noncancerous tumors from growing. If genetic tests show mutated APC genes, providers may recommend specific cancer screening tests.
Most people with Gardner syndrome have colon polyps that may become colon cancer. If that’s your situation, your provider may recommend medication to slow down polyp growth. If you have many colon polyps, your provider may recommend one of the following surgeries:
No, there’s no cure for Gardner syndrome. But there are treatments and other steps to help manage it, including catching cancer early on when it’s easier to treat.
Surgery to remove your large intestine and most of your rectum is the only treatment to keep colon polyps from developing and becoming colon cancer.
Yes, you can, but surgery to treat Gardner syndrome may change your lifestyle. Colectomies change how food travels through your gastrointestinal (GI) tract. Some versions of colectomy may affect the way you go to the bathroom. If you have a proctocolectomy, you’ll have a new pathway for your poop to come out.
That depends. Gardner syndrome causes many different medical issues, some more serious than others. Left untreated, Gardner syndrome causes colon cancer that may be life-limiting. But surgery to remove colon polyps may eliminate the risk of colon cancer. For example, studies show 100% of people who had proctocolectomieswere alive five years after diagnosis.
Gardner syndrome is an inherited condition you can’t prevent. But certain cancer screening tests and interventions like certain surgeries may reduce your risk of developing colon cancer and other related cancers. If you have Gardner syndrome, ask your healthcare provider about appropriate screening tests.
Advertisement
If you’re living with Gardner syndrome, you’re living with the knowledge you’re likely to develop colon cancer and other cancers while you’re still young. That means living with uncertainty. Regular cancer screening tests and treatments help reduce your risk of developing cancer. They also help to catch cancers at early stages when they’re easier to treat.
Living with Gardner syndrome isn’t easy. You may need regular cancer screenings. You may need treatment that will change your lifestyle. If you’re concerned about the ways Gardner syndrome may change your life, ask your healthcare provider about support programs.
Contact your provider if you notice changes in your body that may be new signs or symptoms of Gardner syndrome, such as a new lump or changes in how you go to the bathroom, like blood in your poop.
Some questions to consider include:
Gardner syndrome is a rare inherited condition that may affect you in many different ways. Gardner syndrome causes many symptoms, from having extra teeth and noncancerous bone tumors to developing hundreds of colon polyps that become colon cancer. People with Gardner syndrome have an increased risk of other cancers. If genetic tests show you have Gardner syndrome, you’ll need regular screening tests to catch cancer and other issues early on. If you have many colon polyps from Gardner syndrome, you may need surgery that can eliminate the risk of colon cancer but may also affect your lifestyle. Your healthcare providers may not be able to predict all the ways that Gardner syndrome may change your life. But they can recommend screening tests to catch issues early on and treatments to reduce your risk of serious illness and support you throughout.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Colorectal cancer can turn your world upside down. At Cleveland Clinic, our experts will craft a treatment plan to help you get the best care possible.
