Postpartum preeclampsia is a condition that can happen up to six weeks after your baby is born. It causes you to have high blood pressure and high levels of protein in your pee. Without treatment, it can lead to dangerous problems like brain damage, stroke or even death.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
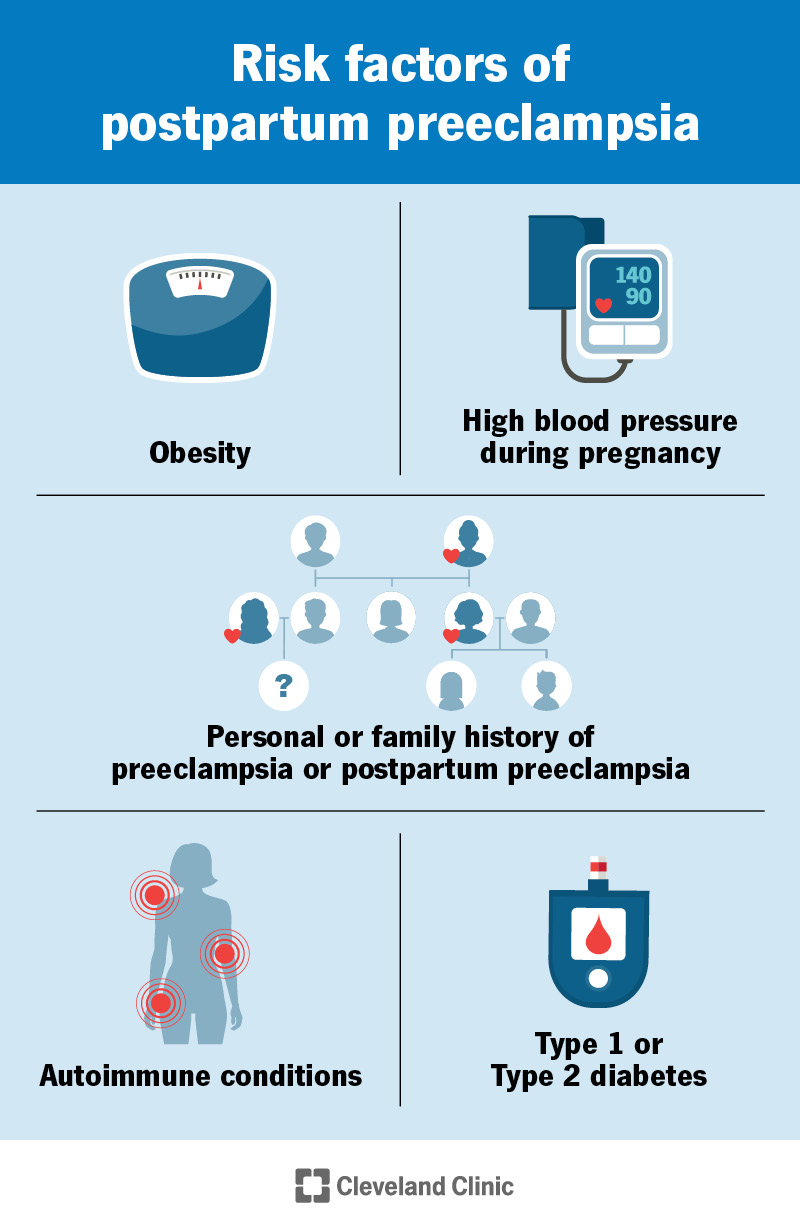
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17733-postpartum-preeclampsia)
Postpartum preeclampsia is a serious condition related to high blood pressure after you give birth. It’s most common within 48 hours of delivery, but it can occur up to six weeks after your baby is born. It can lead to strokes, seizures and other complications if left untreated.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Postpartum preeclampsia is different from preeclampsia. Postpartum preeclampsia only happens after your baby is born. Even if you’ve never had high blood pressure or preeclampsia, you can get postpartum preeclampsia.
If you have symptoms of postpartum preeclampsia, you need immediate medical attention. Treatment usually involves medication to lower blood pressure and prevent seizures and blood clots.
Postpartum preeclampsia occurs in 0.3% to 27.5% of all pregnancies in the U.S. The wide range likely happens because mild cases go unnoticed.
You could have postpartum preeclampsia if you have any of the following symptoms in the hours or weeks after delivery:
If you’ve recently given birth and are experiencing any of these symptoms, you should seek immediate medical care.
The exact cause is unknown. Healthcare providers know that certain factors increase your risk. Be sure to share your medical history with your provider, attend all prenatal and postnatal appointments, and discuss any symptoms you’re having. This can help your provider detect postpartum preeclampsia.
Advertisement
Certain factors increase your risk of having the condition. You may be at a higher risk if you have any of the following:
People who are younger than 20, older than 40, or pregnant with twins or more are also at a higher risk.
The best thing you can do is discuss your complete medical history with your healthcare provider. They can help you understand the risk factors and symptoms.
Postpartum preeclampsia can lead to these complications without treatment:
Your provider may order the following tests to check for postpartum preeclampsia:
If your healthcare provider thinks you have postpartum preeclampsia, they may prescribe:
Tell your healthcare provider if you’re breastfeeding. They can make sure the medicine is safe for your baby.
No. It requires immediate medical attention. If you have any symptoms of preeclampsia after childbirth, contact your provider immediately or go to the nearest emergency room.
Watch for warning signs of the condition and trust your instincts. Seek help when you’re not feeling well or when something feels off.
Contact your healthcare provider right away if you have symptoms like a headache, swelling in your hands and face, or changes in vision. You may need immediate medical attention at the nearest emergency room if you have a seizure or shortness of breath.
It could take several days to a few weeks for the medication to lower your blood pressure to a safe level. Once your blood pressure is manageable, you’re less at risk for other complications.
Recovering from childbirth is hard. Do your best to meet your needs and your baby’s during this time. If you have this condition, you may need extra time in the hospital for closer monitoring. Rest as much as you can and try to focus on your health. Be sure to keep all postnatal appointments, and don’t be afraid to ask for help when you need it.
Advertisement
You’re at a higher risk of developing it again. Your healthcare provider may want to monitor you more closely in a future pregnancy for signs of preeclampsia.
Having preeclampsia raises your chance of having heart problems later in life.
Knowing the signs of postpartum preeclampsia can save your life. Pay attention to your body and how you feel after you have your baby. Tell your healthcare provider if you have symptoms of postpartum preeclampsia, like headaches, swelling and blurred vision. It’s a serious condition that can lead to permanent organ damage, stroke or death.
Early detection and prompt medication treatment are the best ways to help your body heal.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
You’ve had your baby, but your care doesn’t end when you leave the hospital. Cleveland Clinic offers expert postpartum care during the fourth trimester.
