Dyshidrotic eczema makes tiny, itchy blisters appear on your hands and feet. They can crack and peel as they heal. Healthcare providers aren’t sure what causes dyshidrotic eczema. Triggers may include allergies, stress and frequently moist or sweaty hands and feet. Effective management includes at-home treatments and prescription medicines.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
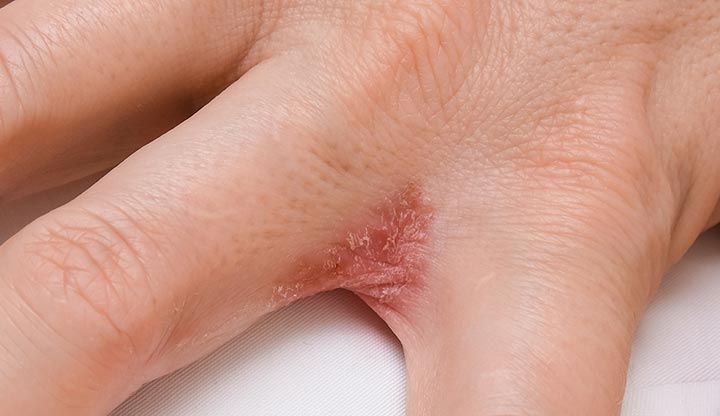
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17728-dyshidrotic-eczema-1303919728)
Dyshidrotic eczema, also called dyshidrosis or pompholyx, is a type of eczema that causes tiny, itchy blisters and dry skin. It usually affects the skin between your fingers, on your palms and on the soles of your feet.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The fluid-filled blisters look like small, cloudy beads. They’re about 1 to 2 millimeters wide — the size of a pinhead. Sometimes, they join together to form a larger blister. When the blisters dry out, your skin may turn scaly and crack.
Out of all people with hand eczema, 5% to 20% have dyshidrotic eczema. A healthcare provider can help you treat and manage it.
Dyshidrotic eczema causes symptoms that come and go. These may last for several weeks at a time. The most common symptoms affect your skin and may include:
In severe cases, blisters may get bigger and spread to the backs of your fingers, hands and feet. They won’t spread to other parts of your body.
Healthcare providers don’t know exactly what causes dyshidrotic eczema. They believe that both genes and the environment play a role. This condition can run in biological families. So, if your parent or sibling has it, you might get it, too. Certain things in your environment, like allergens or stress, can also trigger symptoms.
Dyshidrotic eczema isn’t contagious. You can’t catch it from someone else. And you can’t spread it through physical contact.
Advertisement
A combination of triggers can cause a flare-up, like:
Dyshidrotic eczema can affect anyone. But it’s more common if you:
If you scratch the blisters, you might break your skin open. This can lead to an infection. Contact a healthcare provider if you notice an infection. They may give you antibiotics to clear it up.
As the blisters heal, your skin may become dry, peel or form deep, painful cracks. Scratching a lot can also make the skin on your fingers, hands and feet thicker over time.
Because you can see this condition on your skin, it might make you feel self-conscious and make daily tasks harder. This can cause stress. Stress may make your symptoms worse, since it’s a trigger. A provider can help you manage both your skin and your mental health, because your emotional well-being is just as important as your physical health.
Your healthcare provider will look closely at the affected areas on your skin. They’ll also ask about your health history.
Tell your provider if you started using any new skincare products, wearing new jewelry or eating new foods. This information can help them figure out what might be triggering your symptoms.
Your provider may also suggest tests to confirm the diagnosis, like:
These can also help rule out other conditions that look similar, like:
Treatment for dyshidrotic eczema may include:
Advertisement
You can do a few things at home to make your blisters more comfortable, including:
It can be tempting to pop your blisters, but avoid doing this. The skin over your blisters helps protect the deeper layers from infection.
In addition to caring for blisters, you can try these steps to ease symptoms and help your skin heal:
Your provider might recommend starting with treatments you can get at your local pharmacy, including:
For more severe cases, your provider may prescribe:
Advertisement
Call your healthcare provider if you feel new or worsening symptoms. Let them know right away if you notice signs of an infection, like:
Dyshidrotic eczema symptoms usually flare up and last about three to four weeks before clearing up. This condition affects everyone differently. You might only have symptoms once. Or you might have frequent flare-ups when you contact triggers like allergens, sweat or stress.
If you have repeated flare-ups, the condition may change your skin over time. Your skin could become dry, cracked or thicker. It can even affect your mental health if flare-ups keep happening. Treatment can help you avoid triggers and manage symptoms so they’re less uncomfortable.
Taking good care of your skin is a great first step to help you feel better. Your healthcare provider can work with you to manage this condition and keep your skin as healthy as possible.
To lower your risk of new symptoms or flare-ups:
Advertisement
A flare-up of dyshidrotic eczema can make everyday tasks painful and uncomfortable. Simple things like holding a coffee mug, typing or shaking someone’s hand can hurt and disrupt your day.
But symptoms don’t have to keep you from your daily activities. Your provider can help you find what causes your symptoms. They can also suggest treatments to calm your skin so you can feel better and get back to the things you enjoy.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
