Rosacea is a skin condition that causes redness on your face. The most common places to find symptoms of rosacea include your nose, cheeks and forehead. Rosacea can flare throughout your life and usually starts after age 30. Medicines, creams and lotions help reduce symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
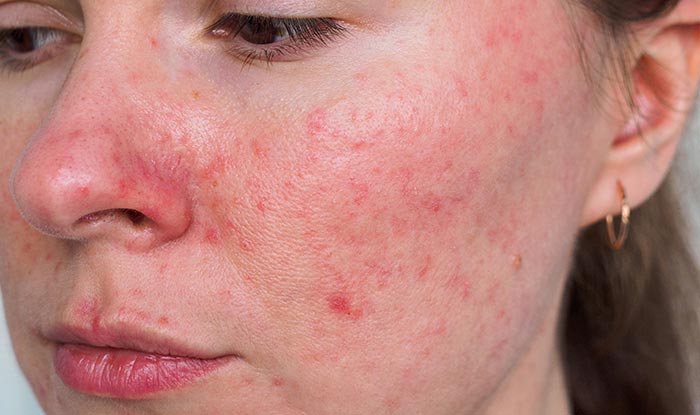
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12174-rosacea)
Rosacea (pronounced “row-ZAY-sha”) is a common inflammatory skin condition that causes redness on your face or other parts of your body, including your eyes. Different types of rosacea may cause pimples and swelling on your skin. This is a lifelong condition without a cure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The four different types of rosacea include:
Rosacea affects more than 14 million people in the U.S. It can affect anyone, but it most often affects women and those with fair skin. Symptoms usually arise after age 30. The condition can affect children and adolescents, but it’s very rare. You’re more likely to have rosacea if someone in your family has it.
Studies suggest that men with rosacea may have more severe symptoms as a result of delaying treatment until the condition becomes advanced.
Rosacea’s appearance can vary greatly from one person to another. Most of the time, not all of the potential signs appear. Rosacea always includes at least one of the primary signs, like:
Advertisement
In addition to signs of rosacea, symptoms of rosacea include:
Symptoms of rosacea can affect several different parts of your body, including your:
Each person diagnosed with rosacea has triggers that cause their symptoms to flare. Possible rosacea triggers could include:
If you’re not sure what triggers your rosacea symptoms, write down a list of foods, beverages, skincare products and activities for a few days to a few weeks and how those things affected your skin that day. This can help you narrow down what could cause your symptoms to flare. When you identify what triggers your symptoms, you can reduce the frequency of your flares by avoiding your triggers.
The cause of rosacea is unknown. Studies suggest rosacea could be a symptom of:
Advertisement
Research is ongoing to learn more about the causes of rosacea and if it’s an autoimmune condition. Some types of rosacea occur as a result of your immune system overworking. Your immune system’s job is to protect your body from foreign invaders that make you sick, like bacteria. A certain type of bacteria (Bacillus oleronius) that’s common among people diagnosed with papulopustular rosacea can cause your immune system to overcompensate for the bacteria and attack healthy skin cells. This is an autoimmune response that causes symptoms of rosacea.
Other cases of rosacea could be the result of your immune system being highly sensitive to changes in your environment. These changes could include sunlight exposure or temperature fluctuations that trigger your symptoms. As a result, your immune system overworks to adjust to the changes in your environment, which causes symptoms.
To diagnose rosacea, your provider will conduct a thorough exam of your signs and symptoms and will take a medical history. During your exam, you should tell your provider about any problems you’re having with your skin (redness, bumps or pimples, burning, itching, etc.). There’s no specific test to diagnose rosacea. Your provider might recommend you visit a dermatologist, who specializes in skin conditions.
Advertisement
Treatment of rosacea varies for each person and focuses on relieving or reducing symptoms and preventing them from getting worse. Treatment options for rosacea could include:
Your provider might offer medications to treat your symptoms of rosacea, including:
Before starting a new medicine, talk to your provider about the dosage, when to take it and the side effects. Also, discuss the medicines you currently take to avoid any drug interactions.
Some studies suggest that spicy foods, like hot wings and jalapeño peppers, can trigger symptoms of rosacea. Every person diagnosed with the condition will have unique and personal triggers in their environment and there’s no guarantee that spicy foods will cause a flare of rosacea. If you have a flare of symptoms after eating spicy foods, avoid eating these types of foods to prevent future flares.
Advertisement
It could take several weeks to a few months before your symptoms reduce. If your provider prescribed medicines, they’ll monitor your treatment to make sure the medicine is effective. Your provider will likely reduce the dosage as your symptoms start to clear up.
Rosacea is a chronic condition, and symptoms can come and go unexpectedly. If you know certain things in your environment trigger your symptoms, avoid those triggers to prevent a flare.
Rosacea is a harmless condition and only causes skin discomfort and appearance changes. Severe and untreated cases can lead to skin disfiguration that most often affects your nose. Surgery treats severe cases of rosacea, but many people find relief from mild symptoms with prescribed medicines or over-the-counter (OTC) creams, gels or lotions.
There’s no cure for rosacea, but treatment options are available to reduce symptoms and flares. Talk to your provider about your symptoms and they’ll help you manage your condition and keep symptoms in remission (keep them from returning).
Since the cause of rosacea is unknown, you can’t prevent it. However, you can reduce your risk of having a rosacea flare by identifying and avoiding things in your environment that trigger your symptoms.
Always use caution when going outdoors and exposing your skin to the sun’s UV rays. Sunlight can trigger symptoms of rosacea and sun damage can make it difficult for your skin to heal after a flare. Wear sunscreen daily and reapply sunscreen often throughout the day. You can also wear UV-protective clothing and accessories to cover your skin from the sunlight.
Over-the-counter makeup products can help cover rosacea. This could include:
Visit your healthcare provider if you have signs or symptoms of rosacea, especially if they cause pain and discomfort.
Symptoms of rosacea and a rash caused by a lupus are similar. Both conditions can affect the skin on your face, especially your cheeks and your nose. Both conditions can flare with sun exposure. The major difference between a lupus rash and rosacea is the texture and appearance of the rash. A lupus rash causes red, scaly, itchy patches of skin. Rosacea causes your skin to appear red, swollen and bumpy. Rosacea is a harmless condition, but lupus rashes can cause long-term damage, like scarring and hair loss.
Rosacea is a harmless skin condition that causes redness, most often on your face. Some people diagnosed with this condition benefit from talking with a mental health professional if they have concerns about their self-esteem and emotional well-being based on how symptoms affect their appearance. Your provider will help you find treatment options to reduce flares and help you feel better.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
