Frostbite occurs when your skin freezes during exposure to freezing temperatures. Frostbite symptoms can include pain, numbness, swelling, blisters and skin discoloration. It’s most common on your fingers, toes, nose and ears. Treatment for frostbite varies based on the stage.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Frostbite is skin damage caused by freezing temperatures below 32 degrees Fahrenheit (0 degrees Celsius). You’re more likely to get frostbite in any situation that leads to prolonged cold exposure:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can get frostbite even under cold-weather clothing.
Frostbite may lead to permanent, irreversible tissue damage (necrosis). A way to prevent frostbite is to limit your time outdoors and warm up your body often if you’re exposed to freezing temperatures.
If you believe you have frostbite, go inside or seek shelter from the cold. Then, call your healthcare provider or visit the emergency room immediately to reduce your risk of tissue damage.
Frostbite can affect anyone with exposure to cold temperatures. It’s most common on your fingers, toes, nose and ears. You’re more likely to get frostbite with prolonged cold exposure, especially if you:
Frostbite is common, but it’s less common than it used to be. This is because people have better access to cold-weather clothing and know more about the dangers of frostbite and how to prevent it.
Advertisement
Frostbite symptoms appear in three stages that include feeling:
If you notice any of the symptoms of the second or third stages of frostbite, get immediate medical treatment to prevent long-lasting damage.
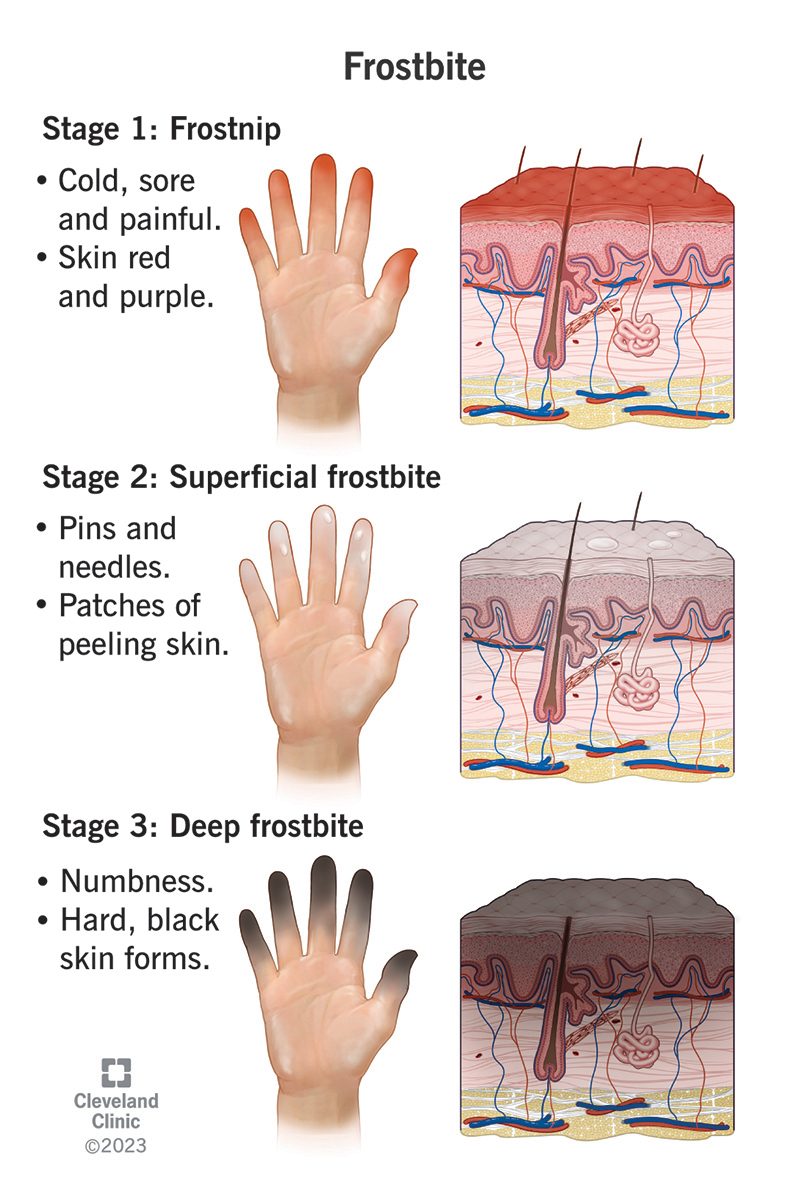
Symptoms of frostbite vary based on what stage you’re in and the severity of skin damage that the cold caused.
Frostbite is dangerous because it often numbs your skin so you may not feel that anything’s wrong at all. Contact a healthcare provider if you believe you have frostnip or frostbite.
Yes. Many people who get frostbite are completely unaware that they have it. This happens because frostbite numbs your nerves and can cause damage deep inside your skin. You might not notice any symptoms after coming in from the cold. It’s important to limit your time outdoors in freezing temperatures to prevent frostbite.
Frostbite can affect any part of your skin, but you’re more likely to get frostbite on your extremities. These are parts of your body that are the most exposed to cold temperatures, even if they’re bundled up and include your:
It can be difficult to tell if your child has frostbite. Infants don’t shiver like adults because they don’t have as much energy stored up. Older children are usually too busy having fun outside to notice they’re frostbitten.
If your baby or toddler is outside in the cold for even 10 minutes, it’s time to check on them. If you notice parts of their skin are lighter than their natural skin tone, red, white or gray, contact their healthcare provider.
Advertisement
If your children are older and they’ve been outside for more than half an hour in freezing temperatures, even with cold weather clothing on, ask them to come inside and remove their wet clothing. They should put on dry clothes and warm their body under blankets. A warm bath may also help your child warm up from the cold. Always use lukewarm, never hot, water.
Freezing temperatures cause frostbite. Cold temperatures (slightly above freezing) for long periods of time can also cause frostbite. You can get frostbite by:
Even if you’re wearing protective clothing like a hat, boots and gloves, you can still get frostbite through your clothing.
When you get frostbite, the water within your skin freezes and crystalizes. Over 60% of your skin contains water. This damages your skin cells and tissues, which prevents blood flow to these areas of your body. Severe frostbite can damage your muscles, nerves and joints.
You can get frostbite in 30 minutes or less when the wind chill is -15 F (-26 C) or lower. If you live or work in cold climates, try to limit your time outdoors to prevent skin damage.
Advertisement
Freezing temperatures cause frostbite. It needs to be colder than 32 F or 0 C for you to get frostbite. Remember that the temperature may be significantly colder if there’s wind, which can increase your risk of getting frostbite.
A healthcare provider will diagnose frostbite after a physical exam and possible imaging tests. During your exam, your provider will look for skin discoloration or other skin symptoms like mottling or blisters. Your provider will also ask you questions about your cold exposure. For example, how long were you exposed to freezing temperatures and what was the temperature during exposure?
Depending on the severity of your symptoms, your provider may take an imaging test like an X-ray to look beneath your skin for tissue damage.
Your healthcare provider will let you know whether or not your skin damage is permanent. An indication that you have temporary skin damage is the presence of clear blisters. If you have blood-filled blisters, you may have permanent damage. If your skin turns black or darker than your natural skin tone, that’s a sign of severe tissue damage. In that case, you may need surgery to remove your damaged skin to prevent secondary infections or gangrene.
Advertisement
Treatment for frostbite varies based on the stage.
If you show signs of frostnip, go indoors or find shelter to get out of freezing temperatures, if possible. Next, take these steps to warm your affected skin:
If you have signs or symptoms of surface or deep frostbite, which are the second and third stages of frostbite, visit a healthcare provider immediately for treatment. Time is critical with frostbite. You may experience severe pain with frostbite as your skin thaws.
To treat frostbite, a healthcare provider will:
For severe cases of frostbite, your provider may need to perform surgery to remove any dead skin and tissue after you heal. It may take days or even months to determine if you need surgery. Surgeons may need to remove (amputate) the fingers or toes if your tissue died or if you develop gangrene.
You should seek care from a healthcare professional if you have frostnip or frostbite. If you’re in a remote area or you’re unable to go to the hospital right away, you can take steps to treat frostbite at home to prevent it from damaging your skin and tissues. Your priority is to make sure you stay warm. You should find shelter and prevent warming and refreezing of your body, which can cause more severe skin damage. To warm up, follow these steps:
You may experience pain during the thawing process. This is normal. You may take over-the-counter pain relievers as directed by your healthcare provider.
If you think you have frostbite, go inside and contact a healthcare provider or visit the emergency room.
The amount of time it takes after treatment for your frostbitten skin to feel better depends on which stage of frostbite you were in and for how long. If you have very mild frostnip, you may heal within a few days to a few weeks. Second-stage frostbite can take up to six months for your skin to heal. You may experience skin scabbing and skin discoloration throughout the healing process. The third and most severe stage of frostbite can cause permanent skin damage. You may need surgery to repair this type of skin damage. A healthcare provider can give you the best timeline of when you can expect your skin to heal based on the severity of your symptoms.
Complications from frostbite are possible. When frostbite continues past the first stage (frostnip), it can have long-term side effects including:
You’re also more likely to get frostbitten again once it’s happened.
Severe complications of frostbite can include:
Here are a few tips for preventing frostbite:
When traveling in cold weather, always bring your phone with you. It’s your lifeline to medical help if you have an accident or get stuck on the road. Finally, pack a car emergency kit in your vehicle. That way, you’re prepared with first aid, food and water, gloves, boots and blankets whenever the weather turns bad.
If you think you have frostbite, don’t wait to seek help. Immediately contact a healthcare provider or visit the emergency room. Acting quickly and removing yourself from freezing temperatures can prevent severe complications.
Chilblains (pernio) are patches of inflamed skin that develop after cold air exposure. This condition isn’t the same as frostbite. Frostbite is skin damage as a result of freezing temperature exposure. The main difference between both conditions is the temperature. Freezing temperatures below 32 F or 0 C cause frostbite and requires immediate medical attention. Cool or cold temperatures above 33 F or 1 C cause chilblains and it usually clears up on its own.
Frostbite happens when part of your body freezes, damaging your skin cells and tissues. Just like ice coating your windshield, your skin becomes hard and changes color when you get frostbite.
Hypothermia happens when your body temperature drops below 95 F (35 C). Your normal body temperature is about 98.6 F (37 C). Hypothermia is more serious and widespread in your body than frostbite, which only affects specific parts of your body (localized).
You can get both hypothermia and frostbite at the same time. Both are medical emergencies.
Stay safe inside or make sure everyone dresses warm whenever cold weather arrives. Not only will you feel more comfortable, but you’ll also help protect yourself and your loved ones against frostbite and all the serious health risks that go along with it. If you have cold exposure for more than half an hour in freezing conditions and you think you may have frostbite, seek immediate medical attention.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.

Last reviewed on 02/22/2023.
Learn more about the Health Library and our editorial process.