Seborrheic dermatitis is a common skin condition that makes your skin itchy, flaky and scaly, especially on your scalp and face. It isn’t contagious and can come and go throughout your life. Treatments like medicated creams and shampoos can help you keep it well managed.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
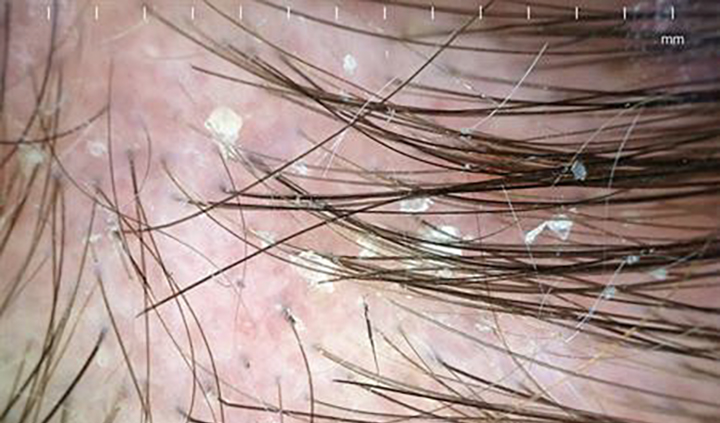
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14403-seborrheic-dermatitis)
Seborrheic dermatitis (pronounced seb-o-REE-ik dur-muh-TAI-tuhs) causes scaly, flaky and itchy patches on your skin. It often shows up on parts of your body with a lot of oil glands, like your face and scalp. It’s a common skin problem.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When it happens on a teen’s or adult’s scalp, it’s usually called dandruff. In babies, it’s called cradle cap.
Seborrheic dermatitis is a lifelong condition. It can come and go over time with flare-ups. There’s no cure, but there are over-the-counter (OTC) and medicated treatment options that can help you manage it.
Symptoms may include:
Babies may have a thick, yellow, crusted scalp rash (cradle cap) and/or a diaper rash.
This condition usually shows up in areas of your body that have more oil (sebaceous) glands. It can affect your:
Researchers aren’t sure of the exact cause. But studies show that too much yeast on your skin could cause it. There’s a type of yeast called Malassezia that lives on everyone’s skin. It’s usually harmless. But when there’s too much of it, a skin reaction happens.
Advertisement
The yeast grows well in oily areas of your body. It makes a substance that turns oil into a fatty acid. Your skin doesn’t like this fatty acid and reacts to it, causing discoloration, itching and flakes. Over time, this weakens your skin’s outer barrier. It makes it easier for the yeast to keep growing and for moisture to escape.
You might notice symptoms get worse if you’re:
No, it isn’t contagious. It doesn’t spread from person to person.
You may be more at risk of developing this condition if you have:
It’s also more common among:
Scratching your skin can break it open, which may lead to bleeding and infections.
Living with a long-term skin condition can be hard, especially if the patches show up on visible parts of your body. This can affect your self-esteem. If you need help coping, consider talking to a mental health provider for support.
Your provider will look at your skin to make a diagnosis. The patches (plaques) are usually easy to recognize, so they don’t need to do any testing.
But if you don’t get better with treatment, your provider may order a skin biopsy. This is to make sure it isn’t another condition.
It’s important to see a healthcare provider if you notice changes to your skin. They can make a clear diagnosis. The following may look like seborrheic dermatitis:
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_rzfaco1p/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Learn three effective ways to manage dandruff.
Seborrheic dermatitis usually doesn’t go away on its own. Treatment depends on where it is on your body and how serious it is. The goal is to reduce flakes and itching. You may need to keep using treatments to prevent flare-ups.
If you have a mild case of dandruff on your scalp, you can try an OTC dandruff shampoo. Look for ones with:
For long-term management, your healthcare provider might prescribe stronger antifungal shampoos. These include:
If your case is moderate to severe, your provider may suggest shampoos with steroids like:
Your provider will give you instructions on how often to use these. You should also talk to your provider about side effects and what to look out for while using these shampoos.
Advertisement
If you have seborrheic dermatitis on your face or body, there are different treatment options:
Your provider will tell you how often to use your medicine and exactly how to apply it. Some medicines come as a cream or ointment that you put on your skin. Others are pills that you take by mouth. Your provider will also explain what side effects to watch for.
Talk to your provider if your symptoms get worse or you have a flare-up. They may need to change your dose, add another medicine or try a different treatment.
You should also see a provider if:
Advertisement
You may want to ask your provider:
Seborrheic dermatitis usually comes and goes. It isn’t dangerous and doesn’t harm your overall health. It’s manageable. Once you start treatment, symptoms usually improve quickly.
But if itching and scaling don’t go away with OTC options, see your provider. They may prescribe stronger medications to help.
If you have seborrheic dermatitis on your scalp, you can try some of the over-the-counter dandruff shampoos. If one shampoo doesn’t work, look at the active ingredient and try another product with a different active ingredient. Shampoos should stay on your scalp for at least five minutes before rinsing off.
If you think you have seborrheic dermatitis on your face or body, see your healthcare provider or dermatologist. They’ll offer an exam to determine the extent and severity of your condition. You’ll work together to develop the best treatment approach to manage flare-ups.
Advertisement
Follow all instructions and never hesitate to call your healthcare provider if you have questions or concerns.
There isn’t much you can do to completely prevent seborrheic dermatitis. Some healthy things you can do to lower your risk include:
Always stick to your healthcare provider’s instructions when using medicated shampoos and skin products. This can make managing your condition easier to prevent flare-ups.
Nothing’s more frustrating than picking out the perfect shirt, feeling an itch on your scalp and realizing your outfit is now covered in flakes. That’s the reality of living with seborrheic dermatitis. It can flare up without warning. It’s a common condition and nothing to feel embarrassed about.
The good news is that treatment can make your symptoms go away fairly quickly. A healthcare provider can help you find a plan that works best for your skin, so you don’t have to worry about itching, scaling or flaking ruining your day.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
