Hemophilia is a rare, genetic blood disorder that happens when your blood doesn’t clot enough to make your bleeding slow down or stop. Hemophilia happens when you don’t have the normal amount of clotting factors. Clotting factors help blood clot. Healthcare providers treat hemophilia by replacing missing clotting factors.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
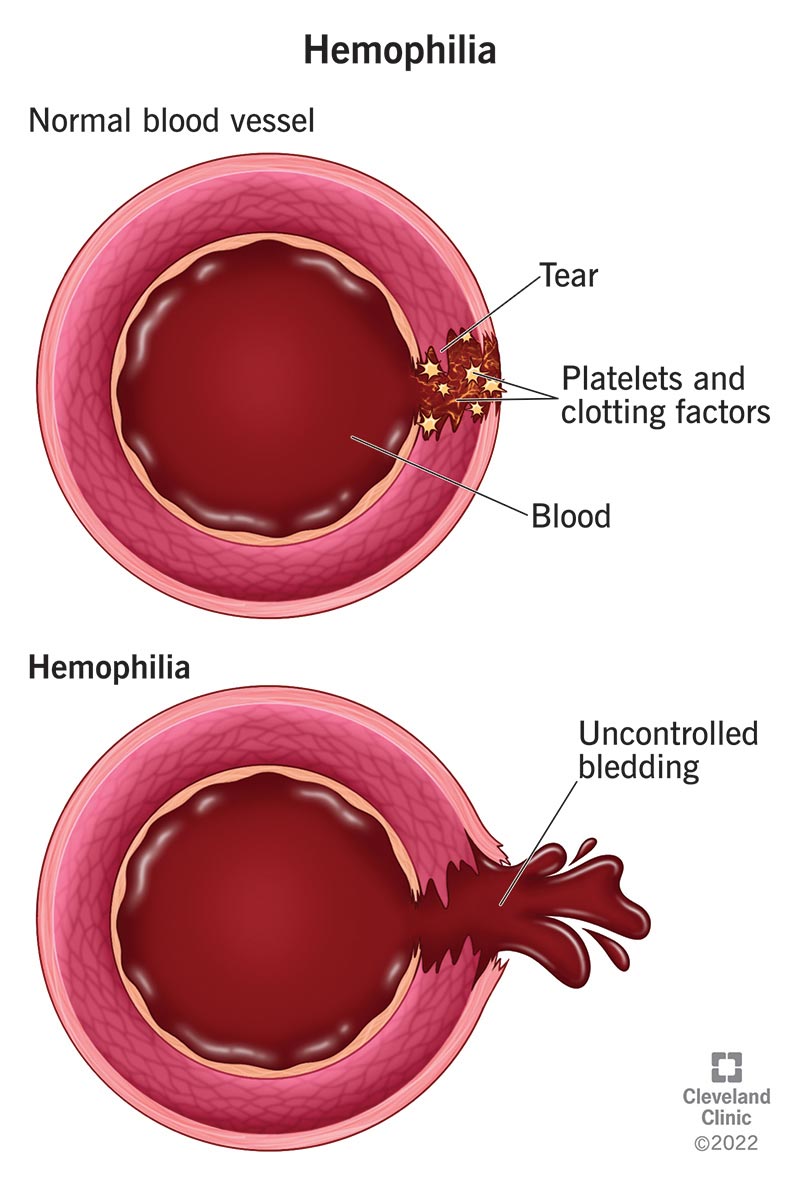
Hemophilia is a rare, inherited blood disorder that causes your blood to clot less, which results in an increased risk of bleeding and bruising.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Hemophilia happens because your body doesn’t make enough clotting factors, proteins that help your blood form clots. Clotting factors work with your platelets to form blood clots that control bleeding. Low clotting factor levels increase your bleeding risk.
There are several types of hemophilia. Hemophilia may be severe, moderate or mild based on the amount of clotting factors in your blood.
Healthcare providers treat this condition by replacing the missing clotting factors. There isn’t a cure for hemophilia, but people who receive treatment generally live about as long as people who don’t have hemophilia. Providers are researching gene therapy and gene replacement therapy as new ways to treat and possibly cure hemophilia.
Yes, but it rarely happens. Acquired hemophilia, or hemophilia that isn’t inherited, develops when autoantibodies start to attack a specific clotting factor in your blood. (Antibodies are protective proteins your immune system makes. Autoantibodies attack antibodies, essentially attacking your body’s own cells, tissues and proteins.)
No, it’s not. According to the U.S. Centers for Disease Control and Prevention (CDC) in August 2022, about 33,000 people in the U.S. have hemophilia. Hemophilia typically affects men. Rarely, women may have clotting factor levels that are low enough to develop symptoms like heavy periods.
Advertisement
There are three types of hemophilia:
It can be. People with severe hemophilia may develop life-threatening bleeding (hemorrhage), but they’re more likely to develop bleeding in their muscles and joints.
The most significant symptom is unusual or excessive bleeding or bruising.
How much bruising or bleeding you have depends on whether you have severe, moderate or mild hemophilia.
Other symptoms may include:
Sometimes, male babies are diagnosed with hemophilia because they bleed more than usual after circumcision. Other times, children develop symptoms a few months after they’re born. Common symptoms include:
Advertisement
Certain genes create clotting factors. In inherited hemophilia, the genes carrying instructions for making normal clotting factors mutate or change. The mutated genes may give instructions that end up making abnormal clotting factors or not enough clotting factors. That said, about 20% of all hemophilia cases are spontaneous, meaning you have the disease even though there’s no family history of abnormal bleeding.
Hemophilia A and B are both sex-linked disorders that are inherited in an X-linked recessive manner. Here’s how that happens:
Advertisement
They can, but those symptoms tend to be mild. For example, a woman carrying the hemophilia gene may not have the normal clotting factors or not enough clotting factors. If that happens, she may have unusually heavy menstrual periods or may bruise easily. She may bleed more after childbirth, or she may develop joint problems from internal bleeding in her joints.
A healthcare provider will start by doing a complete history and physical examination. If you have hemophilia symptoms, your provider will ask about your family’s medical history. They may do the following tests:
Clotting factors help control bleeding. Healthcare providers categorize hemophilia as being mild, moderate or severe based on the levels or amount of clotting factors in your blood:
Advertisement
Healthcare providers treat hemophilia by boosting clotting factor levels or replacing missing clotting factors (replacement therapy).
In replacement therapy, you receive human plasma concentrates or lab-made (recombinant) clotting factors. In general, only people with severe hemophilia need regular replacement therapy. People with mild or moderate hemophilia who need surgery may receive replacement therapy. They may also receive antifibrinolytics, medications that keep blood clots from breaking down.
Blood factor concentrates are made from donated human blood that’s been treated and screened to reduce the risk of transmitting infectious diseases, such as hepatitis and HIV. People receive replacement factors via intravenous infusion (IV).
If you have severe hemophilia and frequent bleeding episodes, your healthcare provider may prescribe prophylactic factor infusions to prevent bleeding.
Some people who have replacement therapy develop antibodies (called inhibitors) that attack the clotting factors. Healthcare providers address this with a technique called immune tolerance induction (ITI). ITI involves giving clotting factors given on a daily basis to bring down inhibitor levels. ITI may be a long-term treatment, and some people may need this treatment for months or years.
If you have hemophilia, you’ll need medical treatment for the rest of your life. How much treatment you’ll need depends on your condition type, severity and if you develop inhibitors.
According to 2012 data from the World Federation of Hemophilia, the lifespan for men with hemophilia is about 10 years fewer than for men without hemophilia. The federation also states that children diagnosed with and treated for hemophilia have a normal life expectancy.
But everyone is different. What’s true for one person with hemophilia may not be true for others. If you or your child has hemophilia, ask your provider what you can expect. They know your/your child’s situation, including overall health, and they’re your best resource for information.
No, they can’t. If you have hemophilia and have children, your healthcare provider may recommend genetic testing so you and your children know whether they might pass hemophilia on to their children.
People with hemophilia may need ongoing medical treatment to prevent bleeding. They may need to avoid certain activities and medications. But there are many things you can do to manage the impact hemophilia may have on the quality of your life.
Bumps, falls and hard knocks that other people shake off may be serious issues for people with hemophilia. They may need to avoid activities that increase their risk of being hit or falling down after being hit. Examples include:
Participating in other sports such as soccer, basketball and baseball may increase your risk of injuries. Ask your healthcare provider what you can do, like using protective gear, so you can play these sports.
Pain medications like aspirin, ibuprofen and naproxen keep your blood from clotting well. You should also avoid anticoagulants such as heparin or warfarin.
There are many things you can do to limit the impact hemophilia may have on your quality of life:
Contact your healthcare provider if you notice changes in your body, like increased bleeding or bruising.
You should go to the emergency room if:
If you or your child is diagnosed with hemophilia, you may want to ask your provider some of the following questions:
Hemophilia is a rare, inherited blood disorder that can seriously impact your life. People with hemophilia may need medical treatment for the rest of their lives. Parents of children with hemophilia may feel anxious about protecting them from accidental injuries. They may worry about helping their children learn to live with hemophilia. At this time, healthcare providers can’t cure hemophilia. They can provide treatment to prevent or reduce hemophilia symptoms. And they can make recommendations for steps you can take to limit hemophilia’s impact on daily life.
When you have a lifelong bleeding disorder like hemophilia, you want the best care. Cleveland Clinic has the support and treatments you need.

Last reviewed on 11/14/2022.
Learn more about the Health Library and our editorial process.