Chorioamnionitis is a serious condition in pregnancy when the membranes that surround the fetus and the amniotic fluid are infected by bacteria. It can cause complications for both you and the fetus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
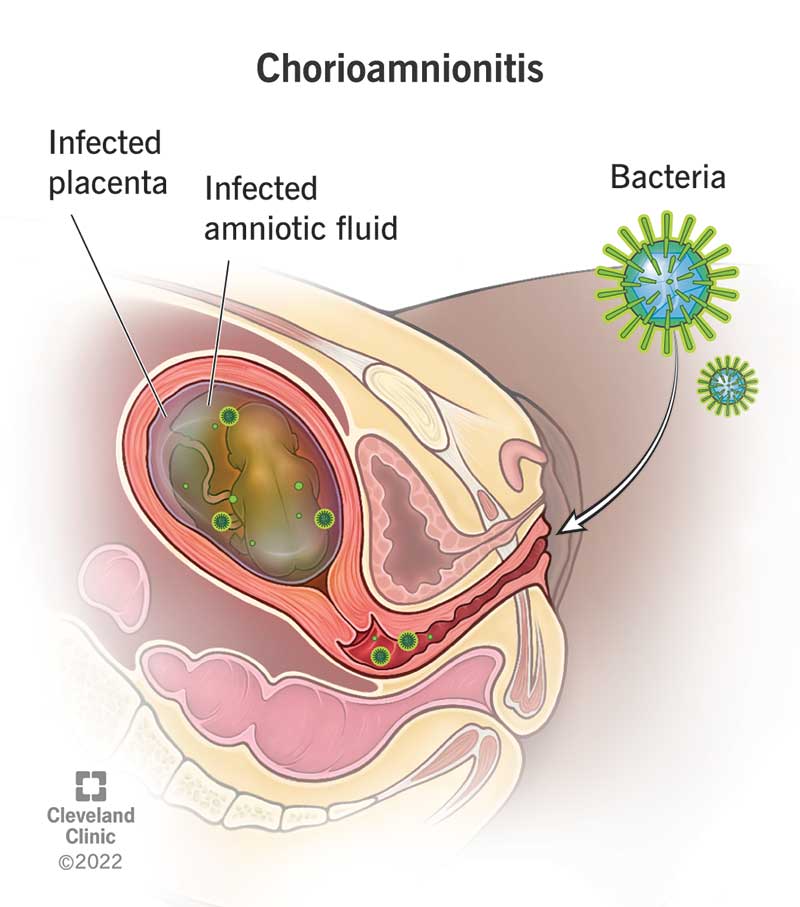
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12309-chorioamnionitis)
Chorioamnionitis (intra-amniotic infection) is a serious infection that affects a person during pregnancy. It gets its name from the two membranes that surround a fetus in your uterus: the chorion and the amnion.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This infection occurs when bacteria enter any of the tissues or membranes around a fetus. This includes:
Treatment usually involves antibiotics, but it may also mean your pregnancy care provider delivers your baby early. It can lead to life-threatening complications in both you and your baby if it’s left untreated.
Chorioamnionitis occurs in about 1% to 5% of births in the United States and is one of the causes of premature labor and delivery.
Symptoms of chorioamnionitis vary. Some of the most common are:
A bacterial infection causes chorioamnionitis. The infection can start in your vagina, anus or rectum and spread up to your uterus. Conversely, it can begin in your uterus if the amniotic sac ruptures or tears. The bacteria can infect your placenta or the fetus.
Infection can also spread if you have too many vaginal exams after your water breaks or after a procedure like amniocentesis.
The most common bacteria that cause chorioamnionitis are E.coli and group B strep.
Advertisement
Yes, chorioamnionitis can affect the fetus. Some of the complications include severe infection and brain or lung problems.
Your pregnancy care provider diagnoses chorioamnionitis with a physical exam and discussion of your symptoms and health history. They may also:
If your provider diagnoses chorioamnionitis, they’ll give you antibiotics to help treat the infection. Antibiotics are typically given through an IV (medication through a needle directly into your vein).
In some cases, providers recommend an early delivery. This can prevent additional issues for you and your baby. If your newborn baby has an infection, they will be given antibiotics as well.
If you have a serious case of chorioamnionitis or if it goes untreated, some of the complications include:
Your newborn baby could also have complications from a bacterial infection, including:
Certain factors might create a higher risk for chorioamnionitis, including:
While some factors are out of your control, there are a few things you could do to reduce your risk of chorioamnionitis. These include:
If you’re concerned about chorioamnionitis, ask your pregnancy provider about your risk of developing the condition so they can evaluate your situation.
Call your pregnancy care provider if your membranes rupture (water breaks). You should also call them if you:
No, a fetus can’t survive without amniotic fluid. Amniotic fluid plays an important role in protecting the fetus. Without it, the fetus is susceptible to infection as well as other life-threatening complications. Your provider will decide when it’s best to deliver the fetus depending on how far along your pregnancy is.
Advertisement
Each situation is different, but generally, most providers want to deliver your baby within 24 hours of your water breaking.
Chorioamnionitis is a serious condition during pregnancy. While you may not be able to control it, there are some things you can do like recognize signs of the condition and share all of your pregnancy symptoms with your pregnancy care provider. Treatment typically involves antibiotics, but it may also mean your baby will be born early. Discuss your diagnosis with your provider and be sure to ask any questions you have.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Worried about your high-risk pregnancy? Want the best maternal and fetal health care? Look no further than Cleveland Clinic. We’re here for all your needs.
