Spirometry is a type of pulmonary function test. It determines how well your lungs work by measuring how much air goes into and out of your lungs when you breathe. Spirometry is safe, though you may feel lightheaded or dizzy from repeated deep breaths. Your healthcare provider will contact you a few days after your test with your results.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
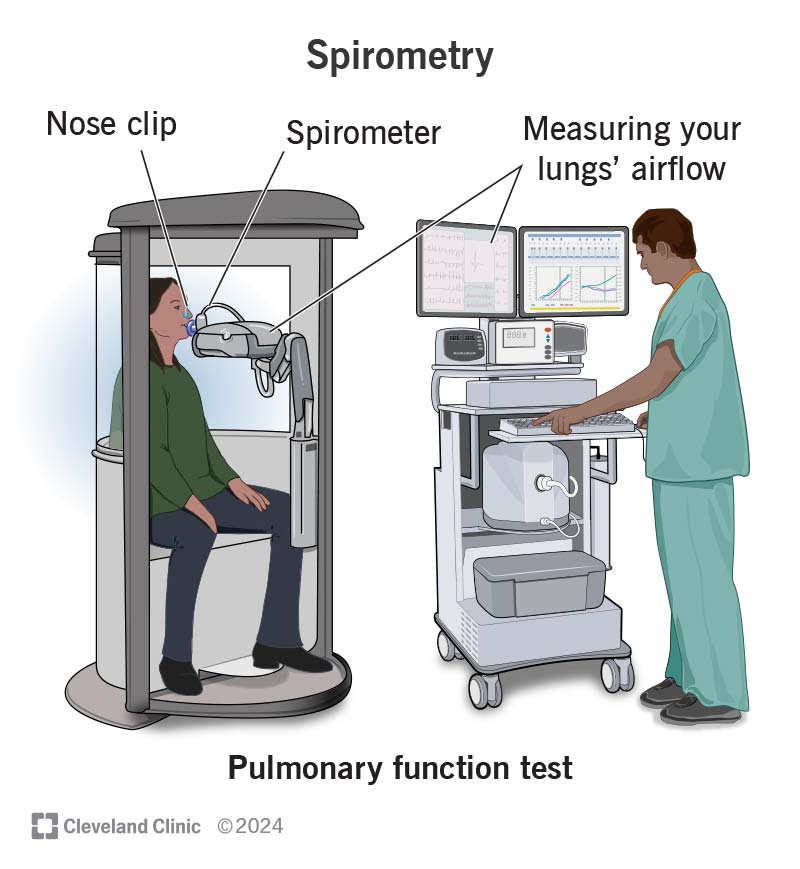
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17833-spirometry)
Spirometry (pronounced “spy-rom-uh-tree”) is a common type of pulmonary function test. Another name for a pulmonary function test is a lung function test. A spirometry test measures the flow of air through your lungs and estimates the amount of air in your lungs. It also tells your healthcare provider how strong your lungs are and how well you breathe.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Spirometry is safe. Healthcare providers commonly order it to evaluate lung function.
Spirometry determines if your lungs are functioning at their expected levels. It also helps to diagnose lung and airway diseases, including:
Spirometry can also:
Your healthcare provider may order spirometry if you have symptoms of lung or airway conditions. Some symptoms in which your healthcare provider may order spirometry include:
Your respiratory therapist, nurse, general practitioner (GP) or pulmonologist may perform spirometry.
Advertisement
A spirometer is a medical device that measures your airflow. It doesn’t help your lungs, but it helps your healthcare provider determine if there’s a problem with your breathing.
Spirometry uses a machine called a spirometer. A spirometer is a medical device that consists of a mouthpiece that connects to a computerized machine that measures your airflow.
Before your test, your healthcare provider may ask you to:
These precautions help ensure that your spirometry results are more accurate.
Your healthcare provider may conduct your test at an office or in a special lung-function laboratory. They’ll place soft clips on your nose. The clips help you breathe in and out only through the mouthpiece attached to the spirometer.
You’ll then take a deep breath in and blow forcefully into the spirometer through the mouthpiece. The spirometer measures the amount of air you blow out of your lungs and the amount you inhale back into your lungs.
You’ll repeat the test at least three times to ensure your results are accurate and reproducible.
Your healthcare provider may also ask you to breathe in a medicine that helps open your airways. You’ll then perform testing on the spirometer again. Your healthcare provider will compare the results of your tests before and after you inhaled the medicine. They’ll then decide if they can use the medicine in your treatment plan.
No, a spirometry test isn’t painful.
But you may feel dizzy, lightheaded or tired from breathing in and out so deeply. Blowing into the spirometer may also cause you to cough. These symptoms should go away shortly after you complete the test. Let your healthcare provider know if you need a break during testing.
Spirometry can also increase your heart rate. Tell your healthcare provider if you’ve had a heart attack in the past or any other conditions that affect your heart.
It depends on the type of spirometry that your healthcare provider orders. But in general, it takes about 15 to 30 minutes to complete the test.
After the test, you may restart any medicines your healthcare provider told you to stop taking. You can also return to your usual activities, including exercise.
Your healthcare provider will tell you when to expect your test results.
In some cases, they may also test for lung volume and diffusion capacity after a spirometry test. These tests measure your lung volume capacity, as well as the ability of your lungs to transfer oxygen to your blood. These tests supplement spirometry tests by helping your provider diagnose certain lung or breathing conditions. Your provider may conduct these tests regularly to see how your breathing is progressing.
Advertisement
A “normal” spirometer reading depends on a few factors, including your sex.
Your healthcare provider will use these characteristics to determine a typical reading for your demographic.
Spirometry measures two main components:
Once you’ve taken your test, your healthcare provider will compare your score against the typical reading for your demographic. A normal reading is 80% or higher than the typical demographic reading.
Your readings can also help your healthcare provider determine what kind of condition is affecting your lungs. These may include:
Advertisement
You won’t know your spirometry test results right after you finish. A specialist must first examine your test results, and they’ll discuss your results with the healthcare provider who ordered the test.
You should expect to get your test results within a few days.
Spirometry test results help your healthcare provider determine:
Your healthcare provider will contact you a few days after spirometry testing to discuss your results. Reach out to your healthcare provider if you don’t hear from them with your results after a few days.
You may have to schedule lung function tests every year if you have a chronic (long-lasting) lung disease.
See your healthcare provider if you notice any changes in your breathing. The changes might not be serious, or they might be a symptom of a lung condition. Your healthcare provider can use spirometry to help diagnose any possible lung conditions. Spirometry isn’t painful. A proper diagnosis can help you and your healthcare provider determine a healthcare plan that enables you to improve or maintain your quality of life.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Breathing issues can affect your life in many ways. Cleveland Clinic’s respiratory therapy program treats your symptoms so you can feel better day to day.
