The Achilles tendon is the thickest and strongest tendon in your body. It connects your calf muscles to your heel bone. Providers sometimes call it the calcaneal tendon. Your Achilles tendon helps you move, walk, jump and climb stairs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
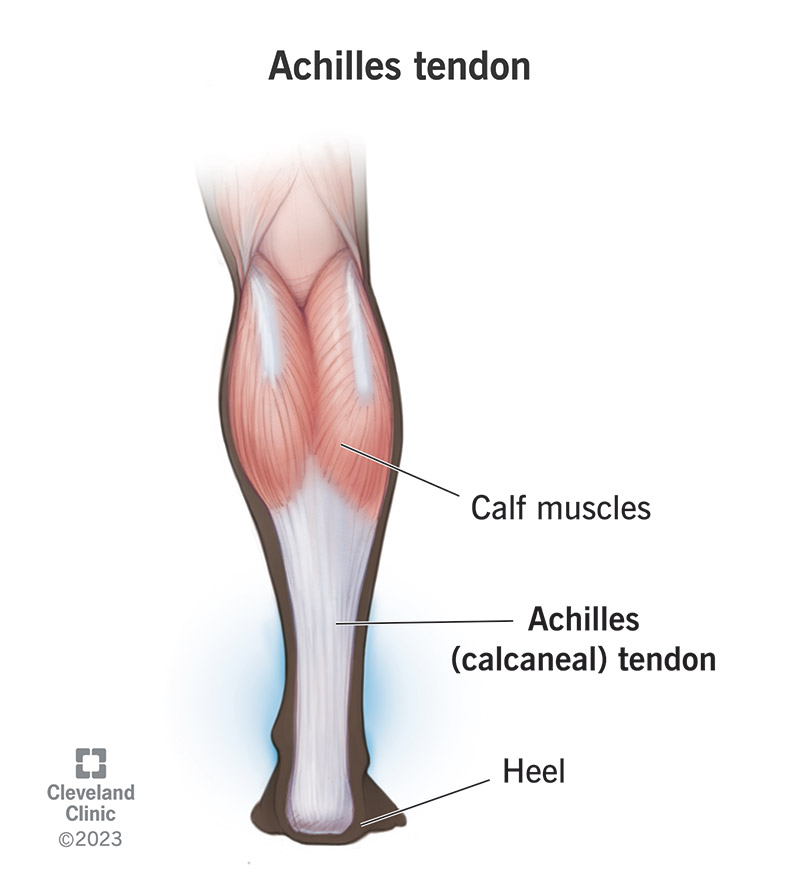
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/achilles-tendon.jpg)
The Achilles tendon is the tendon at the back of your leg right above your ankle. It connects your calf muscles to your heel bone (calcaneus). Calcaneal tendon is the medical name for the Achilles tendon.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Tendons are cords of strong, flexible tissue that connect muscles to bones throughout your body.
The Achilles tendon gets its name from Achilles — a hero in ancient Greek mythology who was invulnerable to any injuries except for one spot on the back of his heel.
The Achilles tendon connects your calf muscles to your heel bone and helps them move your foot and ankle.
When you contract (squeeze) a muscle, its tendons pull the attached bone, making it move. They’re like levers that help bones move when your muscles contract and expand. Your Achilles tendon lets you move your heel and foot. When your calf muscles contract, your Achilles tendon lifts your heel. You use your Achilles tendon when you:
The Achilles tendon starts in the middle of your calf and runs down the back of your leg to your heel. You have two Achilles tendons, one in each leg.
The Achilles tendon is usually between 6 and 10 inches (15 to 26 centimeters) long in adults. It’s the thickest and strongest tendon in your body. It can support forces around four times your body weight.
The Achilles tendon is made of two types of proteins — collagen and elastin.
Collagen is the most common protein in your body. It’s around one-third of your body’s total protein. It gives your tendons strength.
Advertisement
Elastin is stretchy and helps your tendons extend and bounce back to their original shapes as you move.
Your Achilles tendon gets blood from two blood vessels in your lower leg. Two nerves — the sural nerve and tibial nerve — control the Achilles tendon and give it feeling (sensation).
The Achilles tendon is one of the most “famous” tendons because of professional sports injuries. The most common Achilles tendon injuries and issues include:
A healthcare provider will diagnose Achilles tendon issues with a physical exam and some tests. They’ll examine your lower leg, foot and ankle. They’ll ask about your symptoms and when you first noticed them. Tell your provider what you were doing right before you felt pain or other symptoms.
Your provider might use physical tests like the Thompson test to check for an Achilles tendon rupture. They’ll use some of the following imaging tests to take pictures of your Achilles tendon and the tissue around it:
Which treatments you’ll need depends on which type of Achilles tendon injury you have, what caused it, your usual activity levels and your goals. Your provider will tell you which treatments will work best for your unique situation. Some common treatments for Achilles issues include:
You might not always be able to prevent Achilles injuries, especially if they happen when you fall, jump or are playing sports. In general, you can follow these tips to reduce your injury risk:
Advertisement
Most people can walk and move their ankle with a ruptured or injured Achilles tendon. However, it might be painful or difficult. Visit a healthcare provider right away if you think you have an Achilles tendon injury, even if you can walk or put some weight on it.
Using your ankle and putting your full weight on it can make injuries worse. Use crutches, a walker or other mobility aids if you have them while you’re waiting for a provider to diagnose your injury.
Some people only need to change the type of shoes they wear or take a break from physical activities to help their Achilles tendons heal, but don’t assume that an injury will go away without treatment.
Visit a healthcare provider as soon as you notice pain in or near your Achilles tendon — especially if you hear or feel a pop or know you experienced an injury.
The Achilles tendon is named after a hero in Greek mythology, and it does pretty heroic work helping your body move every day. Anyone can irritate or injure their Achilles tendon, even though most people associate Achilles injuries with professional athletes. Visit a healthcare provider if you feel pain in your lower leg, ankle or heel. They’ll help you understand what’s causing the discomfort and how you can help your Achilles tendon heal.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic experts are here to treat your tendinopathy (tendon pain) and get you back to doing the things you love.
