A macular hole is a full-thickness defect in your macula, part of your retina. If this happens, you may have problems seeing clearly, especially in your central field of vision. Surgery to treat a macular hole has high success rates if the hole is small.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_ksd71ruy/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Macular Hole
A macular hole is an actual hole or full-thickness defect in the macula of your eye, the central part of your retina. Your retina is the part of your eye that contains nerve cells that react to light and allow you to see. A macular hole generally happens in just one eye, but it can happen in both eyes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In the middle of the retina (the macula), the nerve cells are very close together. Sometimes, the jelly-like substance that fills your eye — the vitreous humor — changes its consistency and, as it shrinks, it can pull on the central macula and cause a macular hole to form. A macular hole can affect your vision in a variety of ways, but it mainly affects your central vision (the things that you can see in the center of your visual field). It affects activities like driving and reading.
One U.S. study indicates that the number of new cases of macular hole is 7.8 people per 100,000 people per year. It's more common in women. It happens much more often in people aged 55 and over, but it can happen to anyone.
There are primary and secondary macular holes. A primary macular hole is one that develops without any eye injury and isn’t due to another medical condition. A secondary macular hole is one that occurs with or due to another disease or condition, such as trauma or eye inflammation (uveitis).
There are a couple of ways that ophthalmologists may classify macular holes. These are called staging systems. One system uses four stages, with the first stage being the least severe and the fourth being the most severe. A newer system has three stages based on the results of imaging tests. Your eye care provider will give you information on how severe your macular hole is.
Advertisement
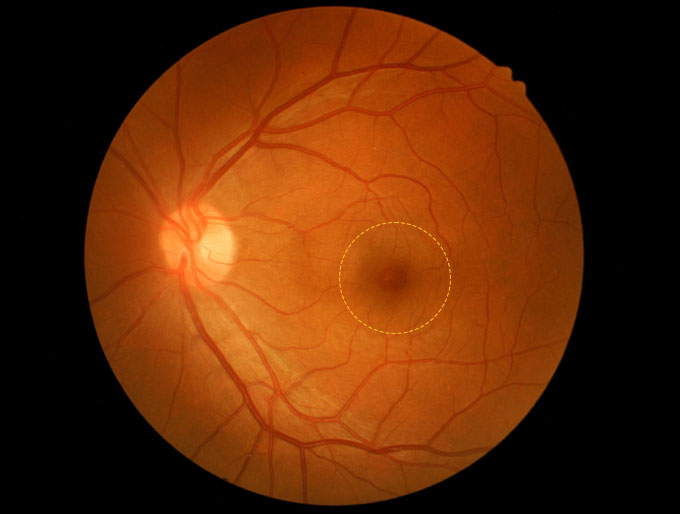
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14208-macular-hole)
The early symptoms of a macular hole include:
A later sign of a macular hole is a dark or blind spot in the center of your vision.
If any of these symptoms occur, it’s important to make an appointment with your eye care provider as soon as possible.
In most people, macular holes are due to vitreous traction that’s more likely to happen with aging. Sometimes a macular hole is the result of an injury or a medical condition that affects the eye, including being very nearsighted.
You may be more likely to develop a macular hole if you have:
Risk factors for macular holes include:
An untreated macular hole may lead to these complications:
Your eye care provider will begin by asking you about your family and medical history. You’ll want to tell them about any type of medication — prescription and over-the-counter (OTC) drugs — that you take. Your provider will then do a complete eye exam, which will include a slit lamp exam. Your provider will put eye drops in your eyes to make your pupils larger and allow for retina examination.
Your ophthalmologist will probably order one or more of these tests to examine your retinas:
The most common treatment for macular holes is a procedure called a vitrectomy. A vitrectomy is a surgery during which a retina specialist removes the vitreous gel of your eye. Your surgeon, an ophthalmologist trained in retina surgery, may also remove any bits of tissue (membranes) that may be putting tension on your macula.
Your surgeon will put a sterile gas into your eye to keep pressure on the hole until it heals. You may have to stay in a facedown position for one to seven days to keep the bubble in place so the hole will close.
If you have a small hole, your retina specialist may suggest watching and waiting rather than treating it. Sometimes an early-stage macular hole will close on its own.
Possible complications of a vitrectomy may include:
Cataracts are expected to progress in any person who’s having retina surgery.
If you have a vitrectomy, you may need to spend up to a week with your head down to keep the gas bubble in the correct position. The gas bubble lasts three to eight weeks, and your vision remains blurry while the gas bubble’s in your eye. It may take several months for your vision to improve and stabilize.
Advertisement
The success rate for vitrectomy surgeries is over 90%. The surgery is most successful when the hole is smaller and more recent. You may regain most or some of your lost vision.
You’ll need to take some time away from work or school. The length of time may vary depending on the type of work you do. Ask your surgeon about what you need to do or to avoid doing after the procedure.
You probably won’t be able to drive for six to eight weeks, and you won’t be able to fly for about that long, either. It takes this long for your body to absorb the gas. Changes in air pressure may make the bubble in your eye get bigger and dangerously increase the pressure in the eye. Avoid any type of activity that involves changes in air pressure.
If you get treatment sooner, or if the hole is small, your prognosis (outlook) is good.
Without treatment, you may lose much of your central vision, but you’ll retain your peripheral (side) vision.
There’s no way to prevent a macular hole. You may reduce your risk by:
Advertisement
Everyone should get regular eye appointments. Apart from these, see your eye care provider any time you notice a change in your vision. If you experience extreme pain, or if you have a sudden loss of vision, go to an emergency room.
If you have a macular hole, you may want to ask your healthcare provider:
Eyes are fragile and important. Knowing that you have an eye condition like a macular hole may cause anxiety. Surgery to treat a macular hole is typically successful, and the odds are better when your provider can find the hole when it’s recent and small. That’s one reason to see your eye care provider on a regular basis.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your eyes are one of your most important senses. If something goes wrong, it can change your world. Cleveland Clinic can help treat all types of retinal disease.
