Interrupted aortic arch is a rare heart condition some babies are born with. It means your baby’s aorta didn’t form as expected. There’s a gap in the curved part (the arch), preventing blood from flowing through to their body. Prenatal ultrasound usually diagnoses this condition. Thanks to medical advances, most newborns have surgery and survive.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
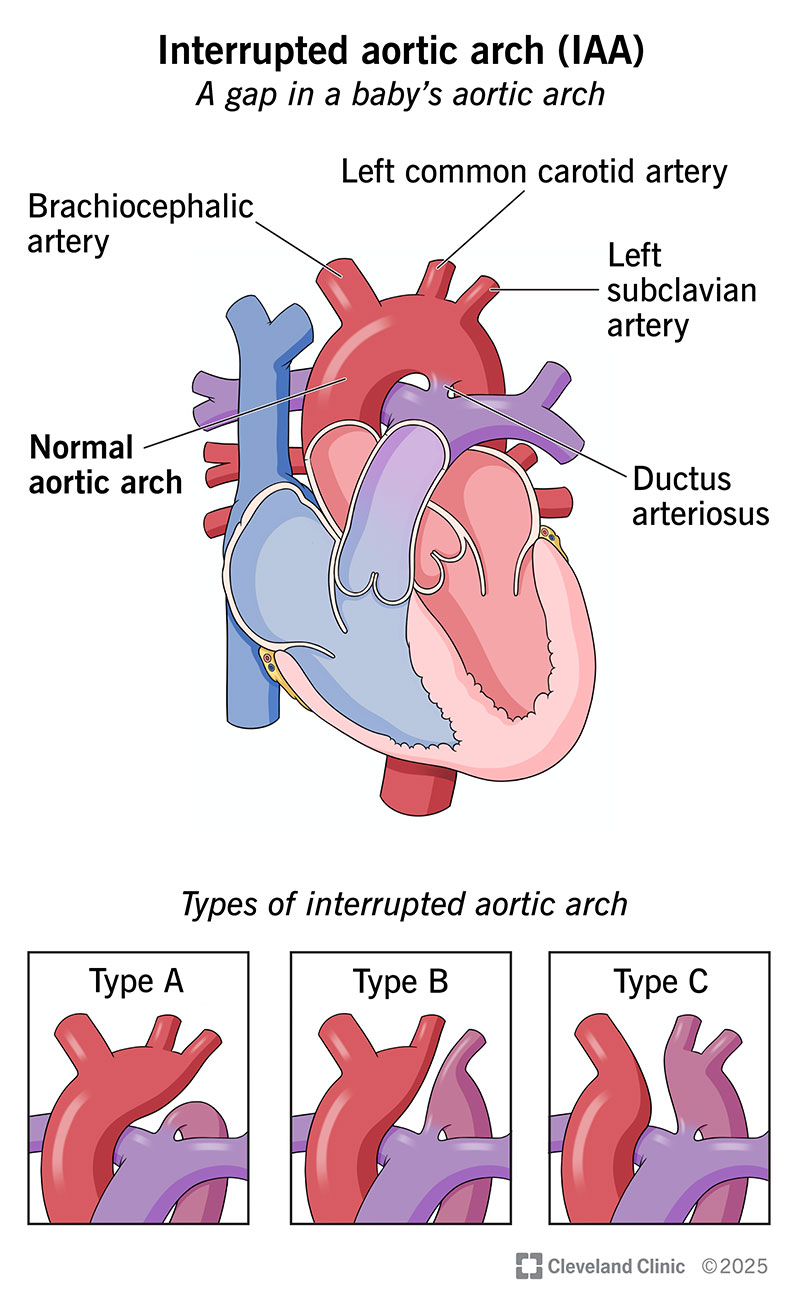
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14734-Interrupted-aortic-arch-illustration-revised)
Interrupted aortic arch (IAA) is a rare type of congenital heart disease that affects your baby’s aorta. This is the artery that carries blood from your baby’s heart to the rest of their body. Normally, your baby’s aorta should curve upward from their heart and then downward in their chest, forming an arch. But if your baby has IAA, that means there’s a gap (interruption) somewhere along the arch.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Picture a railroad with a missing track. Trains can’t get through because of the gap. Similarly, blood can’t flow through your baby’s aorta if there’s a part missing. This matters because your baby’s aorta is their main supplier of oxygen-rich blood.
For a day or two after birth, your baby’s body may still receive enough blood. This is thanks to a fetal blood vessel called the ductus arteriosus. This tiny vessel sends blood from their pulmonary artery into a lower part of their aorta — beyond the missing “railroad track.”
But the ductus arteriosus naturally closes on its own within a few days. This means it only helps temporarily. Healthcare providers can give your baby medicine to keep the vessel open a bit longer. But your baby will need surgery soon after birth to survive.
Interrupted aortic arch affects about 3 in every 1 million babies. It accounts for around 1.5% of congenital heart disease diagnoses. About half of all babies with IAA are also born with DiGeorge syndrome.
There are three different types of interrupted aortic arch based on where the gap occurs:
Advertisement
If your baby is diagnosed with IAA through prenatal ultrasound, they’ll receive care immediately at birth — before you notice any symptoms. Otherwise, symptoms usually appear within two weeks. Your baby may:
These symptoms begin when your baby’s ductus arteriosus starts to close. Once it closes, your baby’s organs can’t get enough blood. Your baby becomes very sick because of the lack of oxygen and nutrients their organs need.
Changes that occur during fetal development cause interrupted aortic arch. As with other congenital heart defects, it’s not always clear why those changes happen. But in some cases, healthcare providers can find genetic causes.
For example, babies with DiGeorge syndrome are missing part of a chromosome. This causes a wide range of features — including interrupted aortic arch (usually Type B) and other heart issues.
Interrupted aortic arch can lead to heart failure and shock. Without treatment, IAA can quickly (within days) be fatal.
Healthcare providers usually diagnose interrupted aortic arch before a baby is born. That’s because a prenatal ultrasound can show IAA, along with other heart defects. A diagnosis before birth helps providers begin to plan treatment. For example, they can prepare to give a newborn medicines that keep them alive until they can have surgery.
But some babies don’t get an IAA diagnosis until after birth, when they start to show symptoms. In this case, providers use an echocardiogram (echo) to get an up-close look at your baby’s heart. An echo can help providers diagnose interrupted aortic arch and other heart issues affecting your baby. The test results guide treatment.
Babies with IAA often have other forms of congenital heart disease, as well. Providers usually diagnose these at the same time as IAA. For example, issues may happen with how a wall (septum) between chambers forms, the number of valve flaps or how arteries connect to the heart.
Babies with IAA may have one or more of the following:
Surgery is necessary to treat interrupted aortic arch. Surgeons can connect the two parts of your baby’s aorta on either side of the gap so blood flows through as it should. Your baby’s care team will explain the exact details of the surgery and the best timing.
Usually, surgical repair for IAA happens within a week of birth. From birth until surgery, your baby will receive care in the NICU. Providers will give them medicine (prostaglandin E1) to keep their ductus arteriosus open. This helps their body get enough blood.
Advertisement
The nature of the surgery depends on your child’s heart anatomy — for example, which other heart defects they have — and their overall health. In general, you can expect that a surgeon will:
Your baby will need many follow-up visits after their surgery. Be sure to follow the schedule their care team gives you. These appointments allow providers to keep a close eye on your baby’s recovery.
As your child gets older, they’ll continue to follow up with a pediatric cardiologist — and eventually, an adult cardiologist.
As with any open-heart surgery, IAA repair comes with risks. Your child’s care team will help you understand what these are. But it’s important to keep in mind that surgery is the only way for your child to survive. And today, outcomes are far better than they used to be. More than 9 out of 10 newborns survive surgical repair for interrupted aortic arch.
Advertisement
About 20% to 30% of babies who have IAA repair surgery need another surgery or procedure later in their lives. This is because it’s common for kids with a repaired aortic arch to develop problems with blood flow through the aortic valve. These issues are treatable.
More and more children with congenital heart disease are living to adulthood — and thriving. As your child gets older, they’ll take a more active role in caring for their heart. The support you offer them today gives them the strongest possible start.
This isn’t how you pictured the first few days of your baby’s life. An interrupted aortic arch diagnosis can leave you and your family reeling — and trying to learn on the fly.
Try to remember you’re not alone. You’re part of a large community of parents caring for babies with congenital heart disease. Connecting with that community can help you feel supported. And whenever possible, let loved ones step in to help with daily tasks, like meal prep or errands.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Learning your baby has patent ductus arteriosus can be stressful. Cleveland Clinic Children’s experts craft a personalized treatment plan to match your child’s needs.
