Hepatitis C is a viral infection that can damage your liver over time. It spreads through contact with infected blood. It affects millions of people, but many don’t know they have it because symptoms are often mild or don’t appear at all. Early testing and treatment with antiviral medications can cure most cases and prevent complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Hepatitis C (hep C) is a viral infection that causes inflammation in your liver. This can lead to serious liver damage. The hepatitis C virus (HCV) spreads through contact with infected blood. Many people with hepatitis C don’t have symptoms. So, they may not know they’re infected. Because of this, the U.S. Preventive Services Task Force recommends a one-time hepatitis C screening for all adults ages 18 to 79.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Hepatitis C can be acute or chronic:
In the United States, researchers estimate that more than 2 million people have chronic hepatitis C.
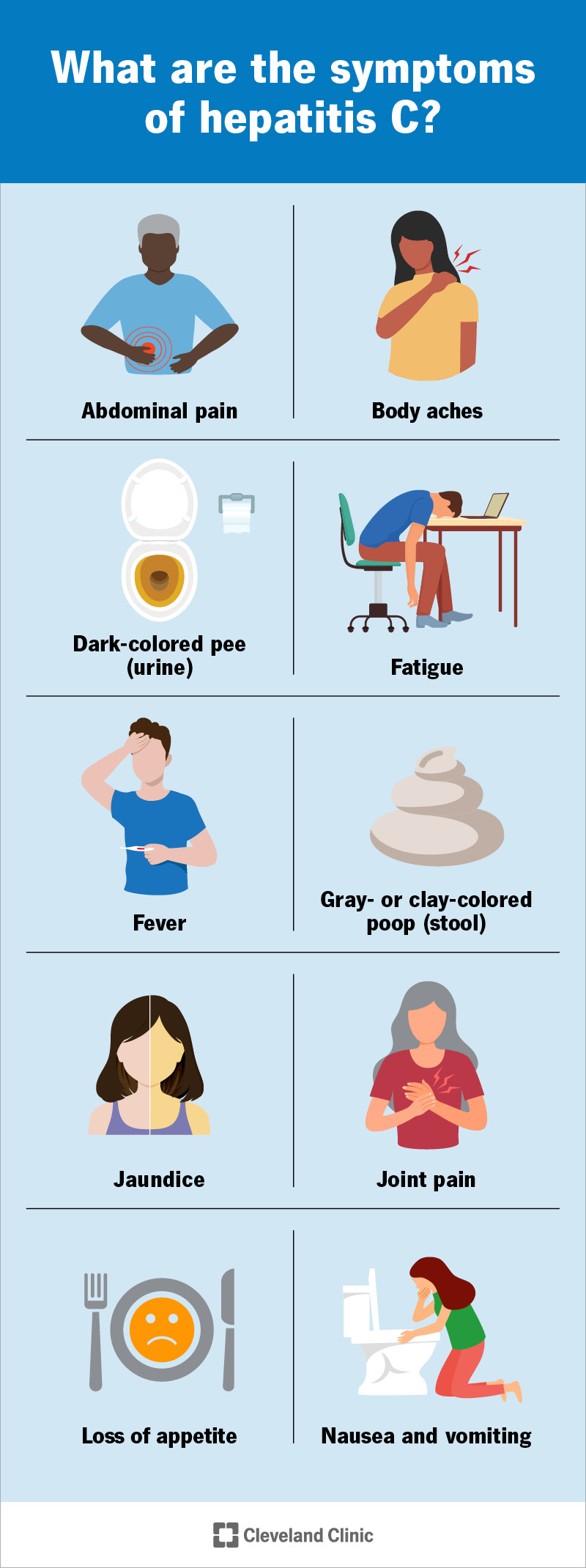
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15664-hepatitis-c.jpg)
Most people with hep C have no symptoms or only mild, nonspecific ones. When symptoms do occur, they may include:
The hepatitis C virus (HCV) causes hepatitis C. This virus infects your liver and leads to inflammation and damage. The virus spreads when infected blood enters your body. In many cases, people don’t know when or how they were exposed.
Advertisement
There are seven different types of the hep C virus. These are called genotypes. They vary in how they respond to treatment. In the U.S., genotype 1 is the most common.
Hepatitis C is contagious, but it doesn’t spread through casual contact. It spreads when infected blood enters your body. The most common way it spreads is through sharing needles or other equipment used to inject drugs. Other ways it can spread include:
In the past, hep C sometimes spread through blood transfusions or organ transplants. But this is very rare in the U.S. now because providers screen the blood supply for the virus.
Hepatitis C doesn’t spread through breast milk, hugging, kissing, or sharing foods or drinks with an infected person.
Hepatitis C is more likely to affect people who have had contact with infected blood. Certain situations increase your risk. These include:
If you’re at high risk, your healthcare provider may recommend screening for hepatitis C more often.
Hepatitis C can lead to serious liver damage over time, especially if the infection becomes chronic and you don’t get treatment. Possible complications of chronic hepatitis C include:
Your healthcare provider will go over your medical history and ask if you have any symptoms. They’ll order a blood test to check for a hepatitis C infection.
Many people with hepatitis C don’t have symptoms. So, providers often recommend testing as part of hepatitis C screening. If a screening test suggests hepatitis C, your provider may order other tests.
Healthcare providers mainly use two types of blood tests to diagnose hepatitis C:
Advertisement
If hepatitis C is confirmed, your provider will order other tests to see how much of your liver is damaged. These may include:
Hep C treatment involves the use of antiviral medications that target the virus. Most people take a combination of medicines in pill form for eight to 12 weeks. But treatment may last longer depending on your situation. Treatment depends on several factors, including the type of hep C virus you have and the health of your liver.
Therapy for hep C involves the use of medicines called direct-acting antivirals (DAAs). These drugs work by blocking the virus from multiplying in your body. Common antiviral drugs for hepatitis C include:
In rare cases, your healthcare provider may also add another antiviral medication called ribavirin to help improve treatment results.
Hep C is usually curable. More than 9 out of 10 people are cured if they take their medications exactly as their provider directed.
Advertisement
After treatment ends, your provider will do a blood test about 12 weeks later. If the HCV virus can’t be found in your blood, it means the infection has been cured.
Being cured means the virus is no longer damaging your liver. But it’s still possible to get hepatitis C again if you’re exposed to the virus in the future.
See your provider if you think you may have been exposed to hep C. Contact them if you develop symptoms like:
The outlook for hepatitis C varies depending on whether the infection clears on its own or becomes chronic. Only about 1 to 2 people out of 10 clear the virus from their body without treatment. For most others, the infection becomes chronic.
Without treatment, chronic hepatitis C can slowly damage your liver. About 1 out of 5 people develop cirrhosis within 20 years. One to 5 out of 100 people develop liver cancer within 30 years.
Hepatitis C spreads through contact with infected blood. You can reduce your risk by avoiding situations where blood exposure may occur. Steps that can help prevent infection include:
Advertisement
Currently, there is no vaccine to prevent hepatitis C.
Hepatitis C can quietly damage your liver for years without causing symptoms. But early testing and treatment can make a big difference. Today’s antiviral medications cure most people and help prevent serious complications. If you think you may have been exposed or have symptoms, talk to a healthcare provider. Getting tested is the first step toward protecting your liver health.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Untreated hepatitis can cause liver damage or failure. Cleveland Clinic’s expert providers offer you the latest treatments and caring support.
