Testosterone replacement therapy (TRT) can help improve the symptoms of low testosterone due to male hypogonadism. TRT has certain risks and benefits, so your healthcare provider will carefully evaluate if it’s safe and right for you.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
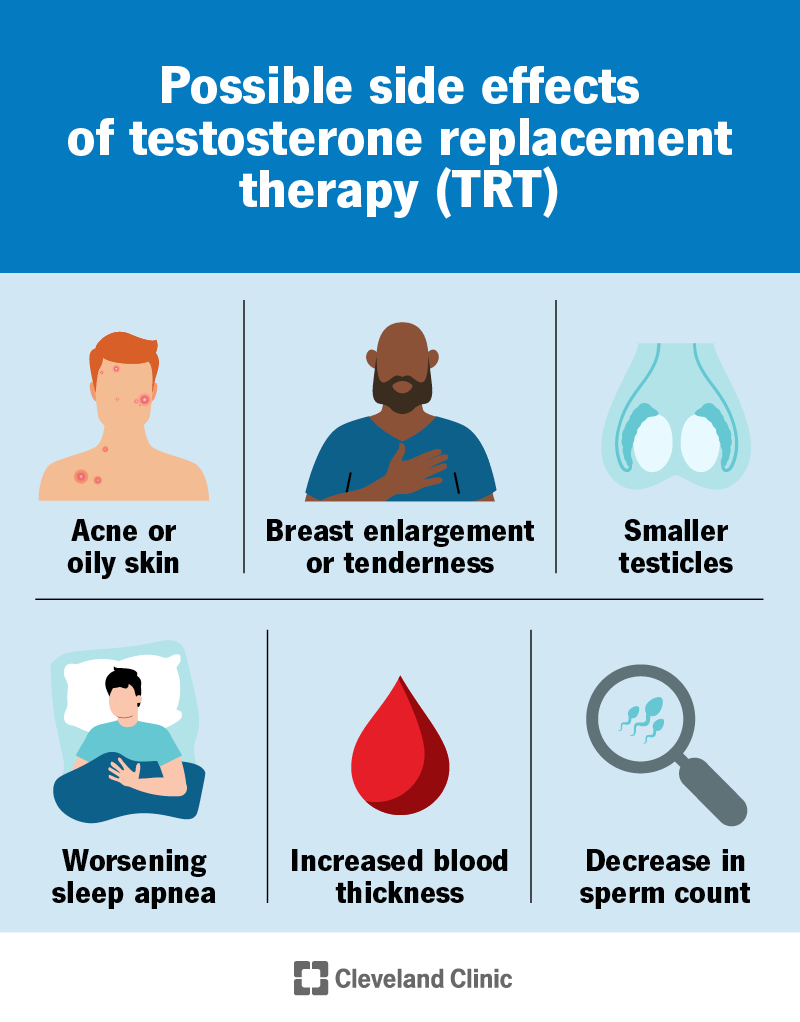
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/testosterone-replacement-therapy)
Testosterone replacement therapy (TRT) is an option for men who have low testosterone levels due to male hypogonadism. TRT involves taking manufactured forms of testosterone to regulate your levels of this hormone.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
TRT comes with certain risks and benefits. Together, you and your healthcare provider will decide if TRT is right for you.
The U.S. Food and Drug Administration (FDA) approves testosterone replacement therapy for males who have low testosterone levels due to a known medical condition (hypogonadism).
Hypogonadism can develop from damage to or malfunction of one of the following organs that are part of testosterone production:
For example, chemotherapy or radiation therapy can damage one of these organs. Or you may have a genetic condition that causes issues.
The FDA doesn’t approve the use of TRT for males with low testosterone without an associated medical condition. As of 2025, it’s not yet approved for males who naturally experience a decline in testosterone as they age.
TRT isn’t for everyone. Certain existing health conditions make it unsafe, like prostate cancer and heart failure.
Before starting TRT, your healthcare provider will make sure low testosterone is an accurate diagnosis. They’ll also make sure TRT is safe for you. They’ll ask about your medical history and do a physical exam. They may order the following blood tests:
Advertisement
With TRT, you take a manufactured form of testosterone to regulate your levels. This can help improve the symptoms of low testosterone, like low libido and lack of energy.
TRT doesn’t fix or cure the underlying cause of low testosterone. In fact, it will cause your testicles to stop working. This means that you’ll need the medication to continue having a normal level of testosterone in your body. If you stop taking testosterone, your body will have to recover its ability to make testosterone again.
Testosterone replacement therapy has several different forms, including:
Your healthcare provider will work with you to figure out which option is best for you. After you start TRT, you’ll need follow-up testing. This includes monitoring your testosterone level and getting other blood tests to make sure TRT isn’t harming your health.
Testosterone replacement therapy can improve many of the symptoms of low testosterone (male hypogonadism). TRT may improve your:
But it’s important to remember that TRT comes with potential risks and side effects.
The side effects of testosterone replacement therapy include:
Laboratory abnormalities that can happen while on TRT include:
It may take a few weeks before you start noticing differences in your body and mood once starting TRT. How long it takes varies from person to person. To allow the therapy to take full effect, healthcare providers typically wait 30 days after you start TRT to check your testosterone levels.
Advertisement
If you don’t notice an improvement in your symptoms after taking TRT for three to six months, your provider may recommend stopping the therapy. This is because if your symptoms don’t improve, your testosterone level may not be the cause of your symptom.
You can stay on testosterone replacement therapy for as long as it’s benefiting your symptoms and not causing health issues. TRT is meant to be a long-term therapy. If you stop taking testosterone, your levels will return to baseline.
Your healthcare provider will recommend regular testing to make sure TRT isn’t hurting your health.
Yes, you can stop TRT once you’ve started. You may do this for several reasons, like if:
If you stop TRT, you’ll return to your normal level of testosterone. Your body will take some time to restart production of testosterone naturally.
Once you start TRT, you’ll have regular appointments with your healthcare provider and routine blood tests. Your provider will let you know how often you need to do this.
Otherwise, see your healthcare provider if:
Advertisement
TRT can be dangerous for some people because it can make certain health conditions worse. You shouldn’t use TRT if you have:
You should also avoid TRT if you’re planning to have biological children. TRT can decrease sperm count and cause fertility issues. Trying to repair your fertility after TRT can be very expensive and take a long time.
TRT is meant for medical purposes. It’s not worth the potential health risks to use testosterone for nonmedical reasons, like bodybuilding or attempting to prevent aging changes.
Certain existing health conditions make TRT unsafe, like prostate cancer, breast cancer and heart failure. This is why healthcare providers do extensive evaluations and tests before approving the use of TRT. If you don’t have these health concerns, TRT is generally safe.
But there aren’t many studies on the long-term effects of TRT (for example, over decades). And some of the studies have mixed results.
For example, some studies suggest that TRT decreases your risk of heart attack over time, while others say it increases your risk. In 2015, the FDA warned that testosterone use is possibly associated with increased cardiovascular risk based on the results of two studies. However, in 2024 the results of a large, randomized trial found that testosterone gel wasn’t associated with increased heart risks over a medium-length period of time. Research has also studied the increased risk of venous thromboembolism, and the results are mixed.
Advertisement
For all these reasons, your healthcare provider will carefully consider if TRT is safe for you based on your unique characteristics.
If symptoms of low testosterone are interfering with your quality of life, know that you don’t have to just grin and bear it. Testosterone replacement therapy may be an option for you. Together, you and your healthcare provider will weigh the risks and benefits of TRT to see if it could help. Don’t hesitate to ask questions or voice your concerns. Your provider is there to support you in all aspects of your health.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.