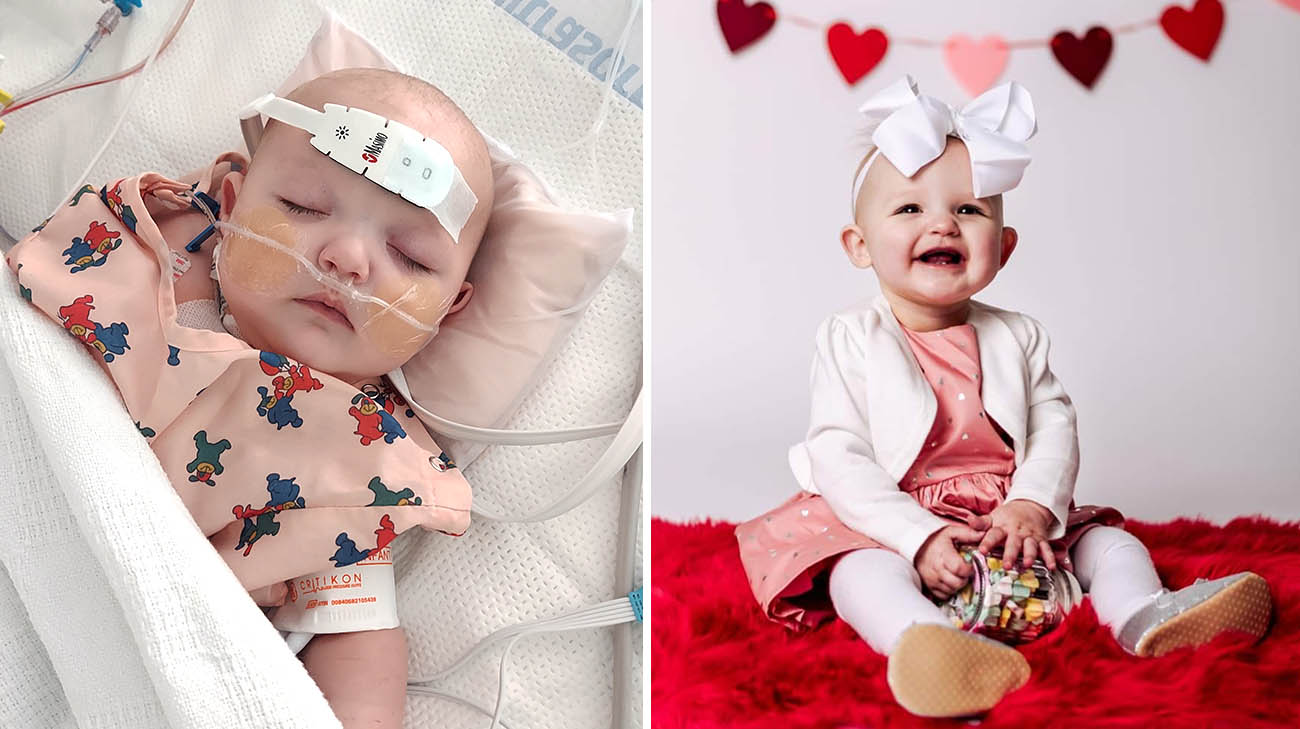
Born in April 2022 with a rare congenital heart defect, Grace Wheeler would require meticulous care, even after her discharge from Cleveland Clinic Children’s.
Grace’s parents Randi and Ken were ready to serve as the eyes and ears for the physicians, nurses and specialists responsible for Grace’s ongoing care as she recovered from surgery at home in Edinboro, Pennsylvania, and prepared for follow-up surgery a few months later.
“I would never have thought of myself as a nurse,” says Randi, who was working as a special education assistant at a nearby school when Grace was born. “As first-time parents, we would have been nervous about taking care of her, no matter what. But we got so much training and help from Cleveland Clinic we definitely had way more confidence with Grace. The program is amazing.”
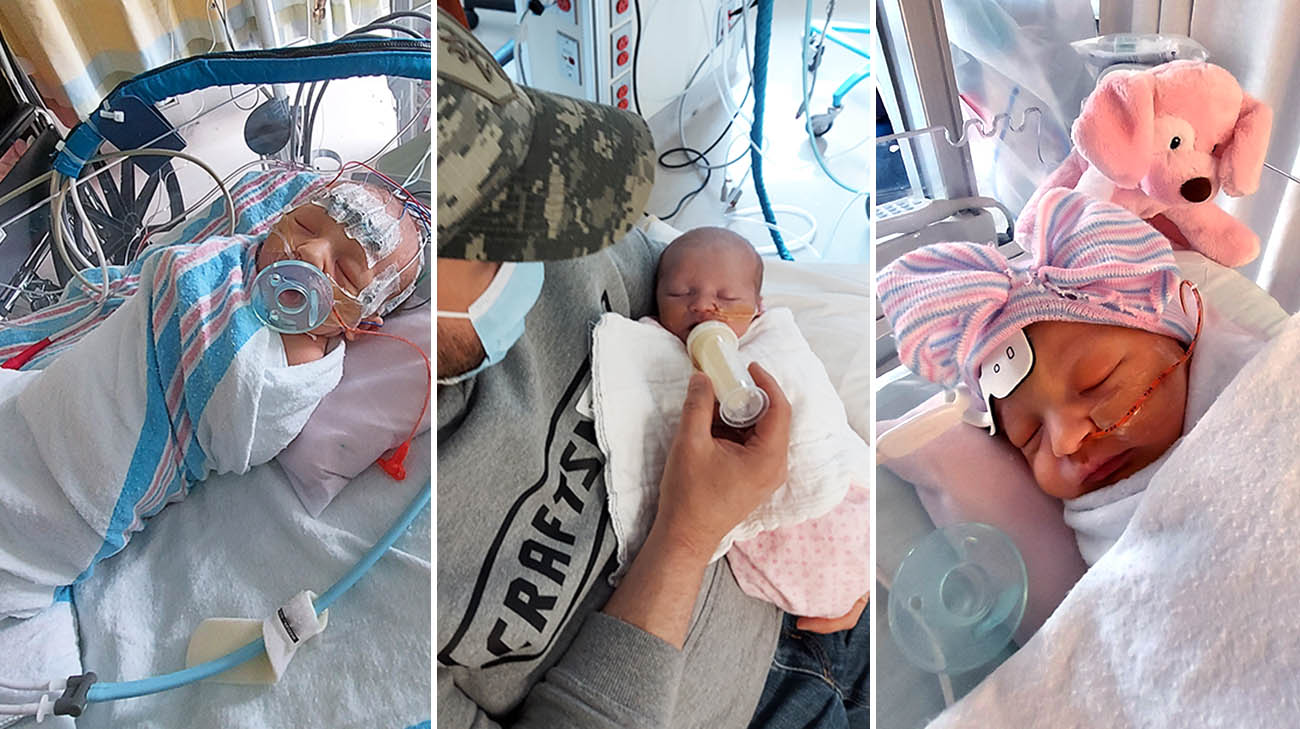
Grace was born with a congenital heart condition called double inlet left ventricle. She only had one functioning lower heart chamber — the left ventricle. (Courtesy: Randi Wheeler)
Cleveland Clinic Children’s Infant High Risk Home Monitoring Program helps pediatric patients with single ventricle heart conditions and their parents make the transition from inpatient hospital care to living at home. Pediatric cardiology nurse practitioner Jodi Zalewski, CNP, along with the program’s care coordinator and registered nurse Lexi Gill expanded and refined the program in 2022.
According to Grace’s pediatric cardiologist Francine Erenberg, MD, the system reduces risk of a catastrophic event for infant patients with heart conditions.
“Our goal is to try and prevent any complications that may occur after the child’s first major surgery and before the next one,” explains Dr. Erenberg. “We want to avoid a bad outcome occurring at home, and the monitoring program is a highly effective way of extending our team into the home, to better keep an eye on these babies.”
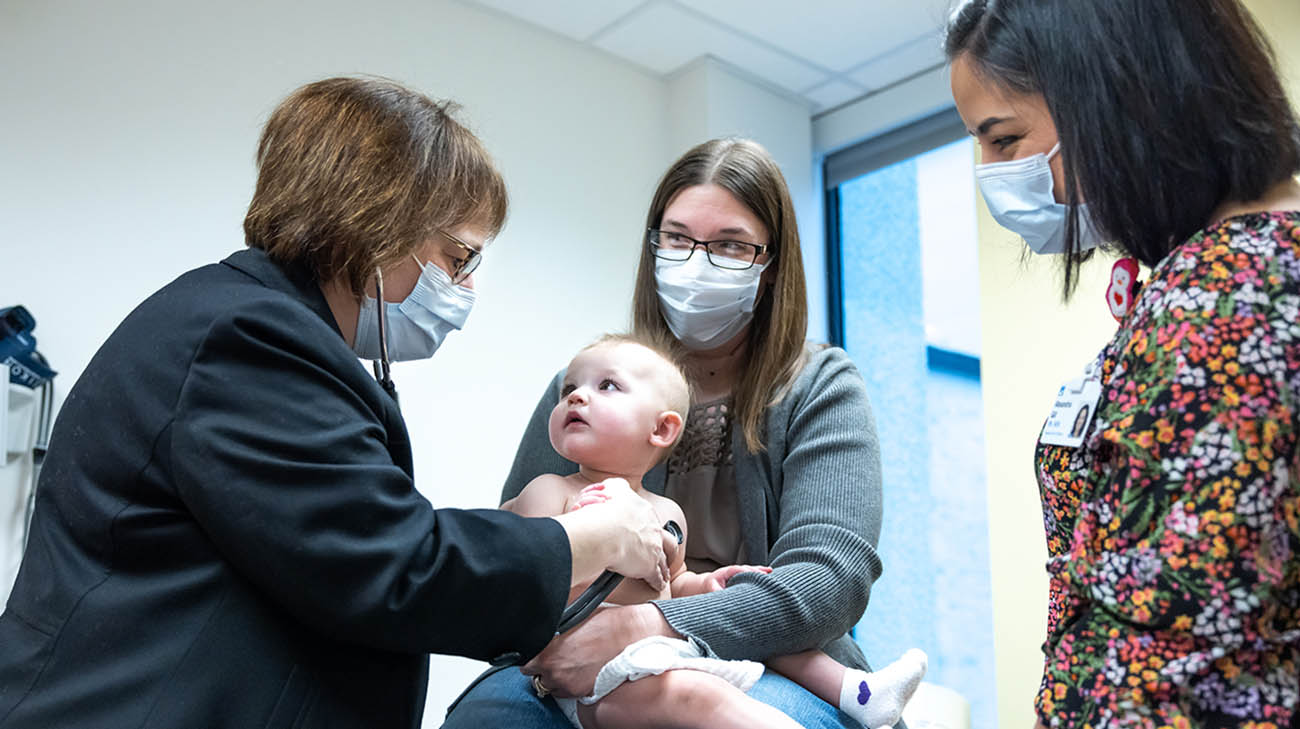
Grace, Randi, Dr. Erenberg (far left) and Lexi (far right), during a follow-up appointment at Cleveland Clinic Children's. (Courtesy: Cleveland Clinic)
Randi’s obstetrician first detected a problem with Grace’s heart well before she was born, based on the results of Randi’s 20-week sonogram. She was referred to Cleveland Clinic Children’s where Dr. Erenberg pinpointed the specific condition -- a rare congenital heart defect known as double inlet left ventricle (DILV).
As Dr. Erenberg explains, a normal functioning heart has two working ventricles, one that pumps blood to the lungs and one that pumps it to the rest of the body. Babies with DILV have just one working ventricle, thus requiring a series of corrective surgeries. Surgeons performed Grace’s first operation six days after her birth, during which they inserted a stent to enhance blood flow.
While the surgery to address Grace’s DILV and related conditions including hypoplastic left heart syndrome and tricuspid atresia was successful in enhancing blood flow, the tiny synthetic shunt ran the risk of failure as Grace’s body grew. By six months of age, she would need a follow-up operation called the Glenn procedure. It would replace the synthetic shunt with one from living tissue that can grow with the child.
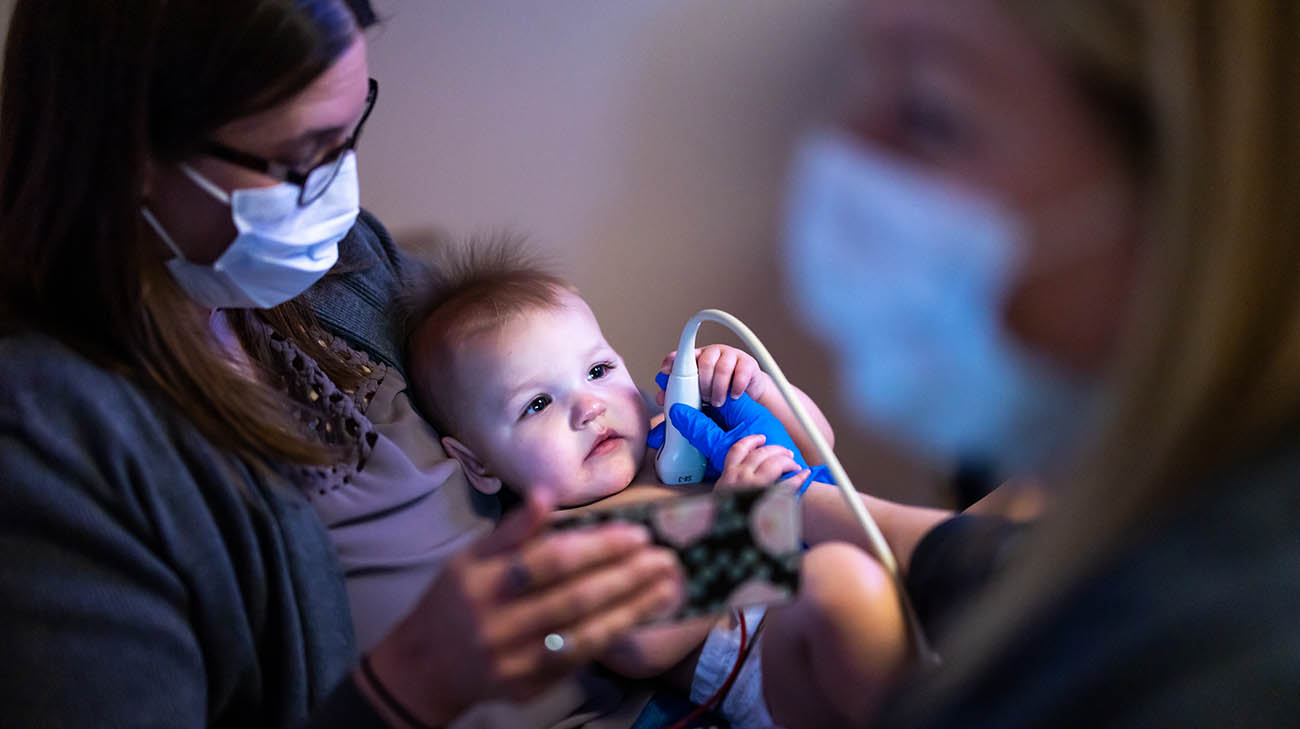
Grace undergoing an echocardiogram at Cleveland Clinic Children's. (Courtesy: Cleveland Clinic)
To ensure Grace had the best chance of survival during the four-month wait between surgeries, the home monitoring team put the program into action. They briefed Randi and Ken on everything they would need to provide care to Grace at home. Randi and Ken were armed with all of the equipment and devices required for everyday use including: a baby scale to make sure Grace was gaining weight; a pulse oximeter and heart rate monitor to check her vital signs; a touchscreen tablet to ensure connectivity back to the care team; and a reference binder detailing procedures and other information.
A Cleveland Clinic pharmacist trained Randi and Ken on how to precisely measure and administer Grace’s medications. They also learned how to load all the information they recorded into an app tied to Grace’s electronic medical records, which Jodi or Lexi would check each day. The technology enabled regular telehealth video calls with Dr. Erenberg and other physicians, who would examine Grace remotely thus limiting the number of long-distance drives to Cleveland for in-person visits.
Perhaps most importantly, Randi and Ken had 24/7 access to Jodi, Lexi or members of Grace’s care team, who would answer their questions and provide direction if a problem ensued.
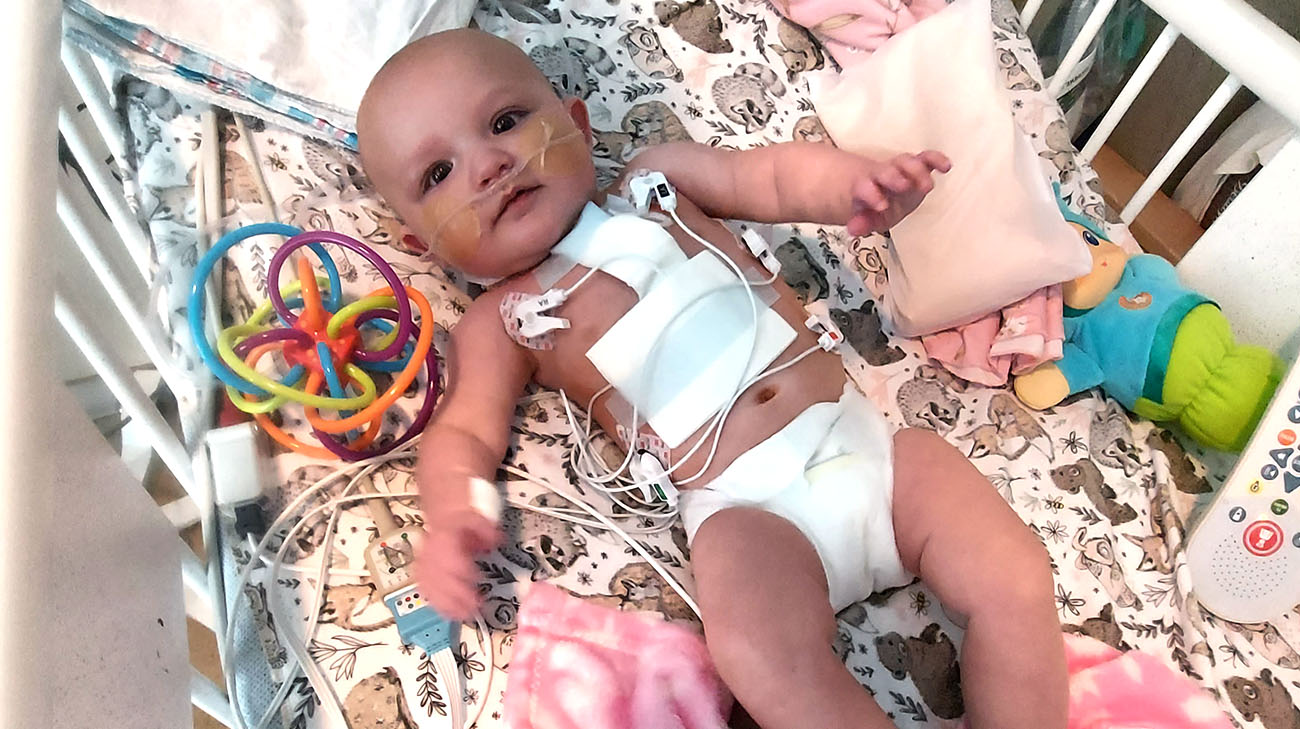
Grace underwent a heart surgery called the Glenn procedure. Doctors replaced the synthetic shunt with one from living tissue that can grow with Grace. (Courtesy: Randi Wheeler)
Soon after Grace began the program, Randi contracted COVID-19. She suspected her daughter had also gotten the virus and immediately contacted Lexi and Jodi. They worked with the family’s local pediatrician and emergency department staff on how to best care for Grace given her high-risk condition.
“As soon as Grace tested positive, they had an ambulance ready to take her immediately to Cleveland Clinic’s main campus,” says Randi. “It was amazing how everything was coordinated so well, and Grace recovered pretty quickly.”
Notes Lexi, “The biggest thing Jodi and I were able to do in building out this program is instill confidence and a level of comfort within these families. No matter where the patient lives, the parents are well equipped to take care of their child. We can coordinate whatever they need, smoothly and quickly.”
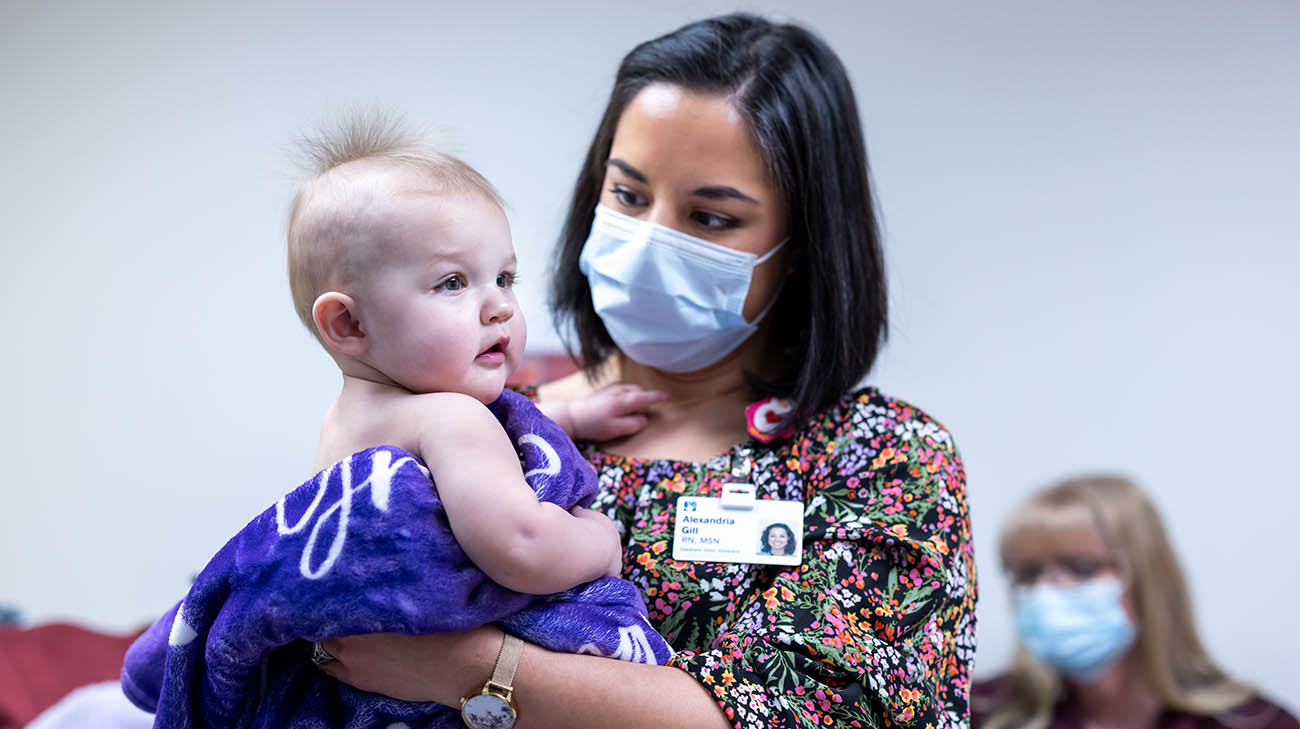
Grace and Lexi during a follow-up appointment. (Courtesy: Cleveland Clinic)
Adds Jodi, “It truly is a multidisciplinary approach to caring for these patients, and it’s rewarding to see it having such a huge impact.”
The program has led to decreases in the number of times patients need to be readmitted to the hospital or visit an emergency department. Jodi and Lexi will present this and additional findings at the 8th World Congress of Pediatric Cardiology & Cardiac Surgery in Washington, D.C., in August 2023.

After Grace successfully recovered from the Glenn procedure in August 2022, she graduated from the Infant High Risk Home Monitoring Program. (Courtesy: Randi Wheeler)
Jodi had the idea to enhance and expand the existing home monitoring program. She applied and was awarded a Cleveland Clinic Catalyst Grant to help fund her idea. The grant covered most of the cost for purchasing the equipment and technology enhancements necessary to implement the upgraded remote monitoring program.
Catalyst Grants pool donations to fund the brightest ideas from Cleveland Clinic caregivers to improve patient outcomes and experiences. To date, more than 250 grants have been awarded, representing a total of $11 million in support.
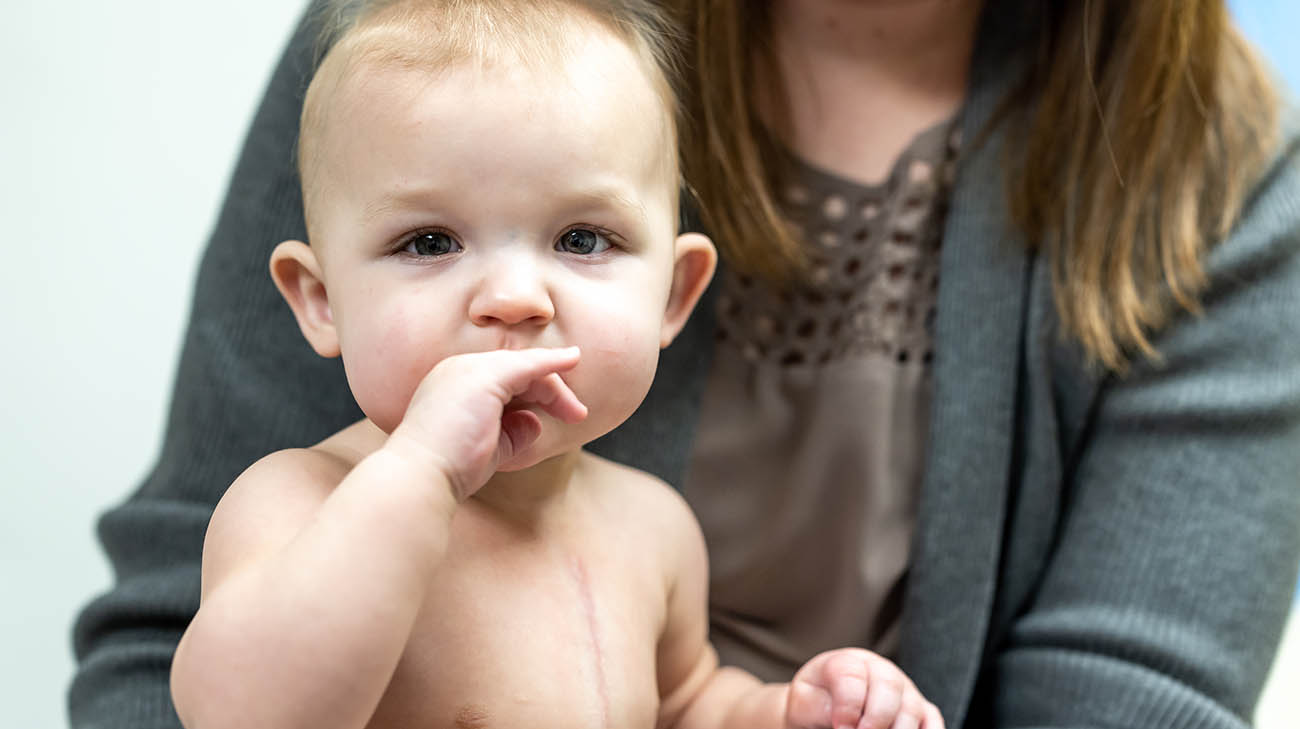
Grace is thriving at home. She continues follow-up visits with Dr. Erenberg. (Courtesy: Cleveland Clinic)
After Grace, who turned 1 in March 2023, successfully recovered from her Glenn procedure, she “graduated” from the program. Since then, she has thrived. She enjoys playing outside, reading books and watching educational videos. She’ll need another surgery when she is 4 years old, but for now only makes visits to see Dr. Erenberg every six months.
“When people meet her, they have no idea she had had two major heart operations,” Randi exclaims. “She’s doing really well.”
Related Institutes: Heart, Vascular & Thoracic Institute (Miller Family), Cleveland Clinic Children's

