
Welcoming your first child into the world is a big milestone for any parent. For Matt Hiznay, it’s something he didn’t think would be possible after doctors diagnosed him with stage 4 lung cancer at 24 years old.
“At the time of my diagnosis, I was so focused on taking everything one day at a time. I wasn’t thinking about the weeks or even months ahead,” says Matt.
It was August 2011, and Matt was entering his second year of medical school when he brought up a persistent dry cough to his doctor. Further testing revealed the diagnosis that didn’t seem possible for someone his age.
“I was thinking, ‘I’m 24. I’m a lifelong nonsmoker. I’m not supposed to get cancer,’” says Matt, the now 36 year old of Lakewood, Ohio.
According to the American Cancer Society, most people diagnosed with lung cancer are 65 years old or older. While smoking is the leading risk factor for lung cancer, a gene mutation caused Matt’s aggressive form of the disease.
“Matt is one of the youngest people I've ever seen with lung cancer. It's extremely rare. He has a type of cancer that's caused by a specific mutation to a gene called ALK, which is only present in about 4% of lung cancer cases,” says Nathan Pennell, MD, PhD, Matt’s hematologist and medical oncologist at Cleveland Clinic.

Matt’s now-wife Aleksandra supported him as he underwent multiple treatments after being diagnosed with lung cancer in 2011. In 2015, he found the medication that’s kept him in remission today. (Courtesy: Matt Hiznay)
After his diagnosis, Matt tried multiple treatments that would work for some time, but his cancer would ultimately recur. That’s until he enrolled in a phase I clinical trial for lorlatinib, a targeted therapy that would attack only the cancerous cells with Matt’s specific gene mutation.
“I wasn’t scared,” Matt says about beginning the trial. “There’s not much that can scare me anymore. I have a lot of faith in these types of drugs and therapies, and I’ve been fortunate I’ve responded.”
Since starting the trial in 2015, Matt continues taking the now FDA-approved medication today. While his cancer hasn’t been cured, it remains in remission. He currently has no evidence of disease.
“People take their diabetes and heart pills, and I take my cancer pills,” says Matt.

Matt ended up enrolling in Cleveland Clinic’s Molecular Medicine PhD program and worked in a lab at Lerner Research Institute for a period of time. (Courtesy: Cleveland Clinic)
After benefitting from a clinical trial, Matt is paying it forward through his work by furthering medical research. Instead of finishing medical school, he joined Cleveland Clinic’s Molecular Medicine PhD program and conducted research in a lab at Lerner Research Institute. He now works for a company that matches patients with cancer to clinical trials based on genetic reports.
“Even though I didn’t finish medical school, it all kind of came full circle. I’m not able to treat patients directly, but I work for a company still helping oncologists do that,” says Matt.
Along with continuing his education, Matt is also grateful he made the decision with his care team to undergo sperm banking, which is the process of collecting, freezing and storing sperm cells. Since certain cancer treatments can affect fertility, sperm banking is a way to increase the chances of having biological children down the road.

Matt and his wife are enjoying every moment with their daughter Theodora. Matt’s thankful for making the decision to undergo sperm banking. (Courtesy: Matt Hiznay)
“For a young person who’s recently been diagnosed with an advanced cancer, fertility preservation is often the last thing on their mind. They're not really thinking about starting a family at that time, but it’s still important to have the conversation and let them know fertility preservation options are available,” says Dr. Pennell.
More than a decade after undergoing fertility preservation, Matt and his wife welcomed their daughter, Theodora, into the world in May 2023. “The decision I made back then has simply meant everything. Having my daughter has enriched my life so much,” says Matt.
Now a 12-year lung cancer survivor and first-time father, Matt has been able to celebrate his milestones with the care team he’s known since 2011. It’s been rewarding for both Matt and Dr. Pennell.
“Matt's story is the most extraordinary treatment journey I've ever been privileged to be a part of. It's something that can give hope to other patients,” says Dr. Pennell.
Matt adds, “When we brought Theodora to my most recent appointment, it was very emotional seeing the smiles on everyone’s faces. They were able to see the fruits of their labor, and I was happy to have been able to do that for Dr. Pennell and his team.”
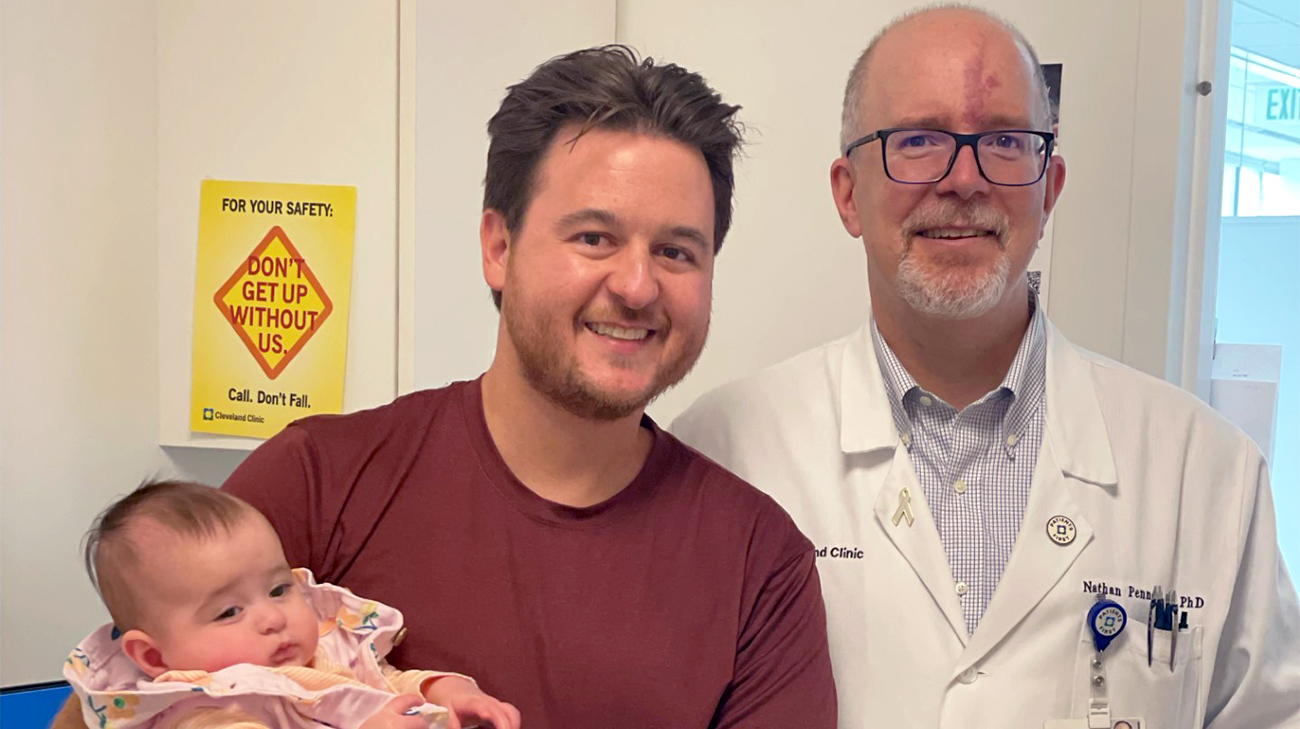
After she was born, Matt brought Theodora to visit his care team, including Dr. Nathan Pennell. (Courtesy: Matt Hiznay)
Matt continues to enjoy spending time with his family and cheering on his favorite Ohio sports teams. He hopes sharing his story can help others struggling with a difficult diagnosis.
“My story was possible for me, and it can certainly happen again. When you’re first diagnosed, it can become overwhelming very quickly. Focus on getting through each day and don’t get too ahead of yourself – just take things one day at a time,” says Matt.
Related Institutes: Cleveland Clinic Cancer Center

