Spinal fusion is a surgery procedure that reinforces your back structure and stability by linking two vertebrae together. The vertebrae support each other, with the goal of reducing pain and easing symptoms related to your spinal cord and nerves.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
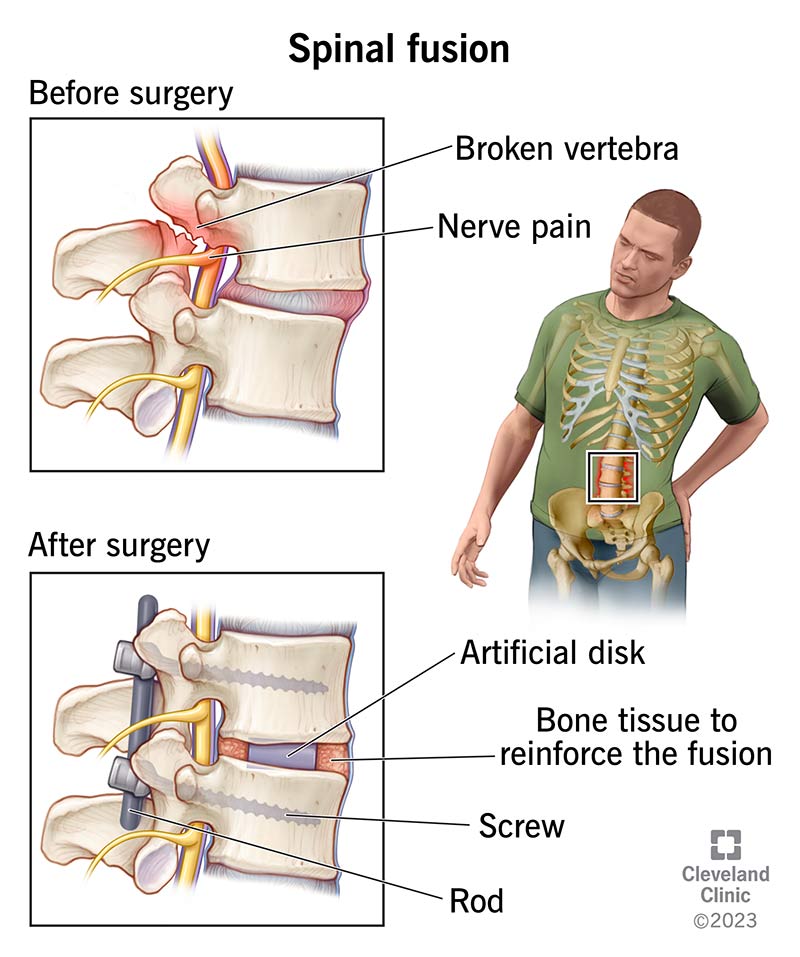
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/25168-spinal-fusion)
Spinal fusion is a surgery that connects two or more vertebrae in your spine (backbone). These ring-shaped bones form an interlocking column that holds your body upright. Fusing them together can reinforce your back’s structure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There’s more than one type of surgeon that specializes in spinal fusion surgery. Neurosurgeons and orthopedic surgeons can do them, depending on the underlying condition and your specific needs.
There are many options for treating back pain and spine problems. Sometimes, treatments other than surgery are more effective or safer (with a lower chance of complications). But for some people, spinal fusion may be the best choice.
A spinal fusion can treat pain, numbness, muscle weakness and more. Weakness at any point of your spine can put pressure on your spinal cord or the spinal nerves that branch off of it. Pressure on your spinal cord or nerves can disrupt the signals traveling through them. Spinal fusion treats conditions that can affect your vertebrae or the joints or soft tissue that support and connect your vertebrae.
Some examples of conditions like this include:
Advertisement
Once you and your surgeon agree that a spine fusion is the best treatment, there are a few more steps to make sure you’re ready to undergo surgery. Some of the most likely steps include:
First, you’ll spend time in the preparation area. During this phase:
Then, they’ll wheel you to the operating room. At this time:
Finally, the time has come for you to be put to sleep so the surgery can start.
Advertisement
Spinal fusion surgeries vary depending on what part of your spine they’re trying to reach and what kind of fusion you’ll need. Some of the variables include:
Advertisement
Once all the portions of the spinal fusion are complete, your surgeon will close the incision(s) with surgical staples, sutures or other means. Some types of sutures need removal, while others your body absorbs on its own. Your provider will tell you what type you have and whether you’ll need a follow-up visit to remove them.
After the surgery is over, your care team takes you to a place to recover where:
Your time in the operating room includes many steps in addition to the actual time for surgery. The actual spinal fusion can take anywhere from one to five hours. The time needed for the surgery can vary depending on your specific needs and circumstances, so your provider is the best person to tell you how long your surgery could take.
After your surgery, the next step depends on whether your surgery was an inpatient or outpatient procedure. An outpatient procedure means you’ll probably go home the same day or early the following day. An inpatient procedure means you’ll stay in the hospital for a few days.
Advertisement
Depending on the surgery you had and the reason you needed it, you may need to learn how to hold yourself and maintain posture. That can affect how you sit, stand, walk and move around. You may also need to wear a brace or support of some kind.
During your recovery, your provider will have you avoid certain activities and types of movement for a while. That means you’ll need assistance with many tasks, including some that seem simple. It’s critical that you follow your provider’s guidance on activity limitations. If you don’t understand part of the instructions, be sure to ask questions. It’s always better to ask beforehand than to do something that disrupts your recovery.
Your provider may also recommend that you undergo physical therapy after surgery. That usually starts a few weeks after your surgery. Physical therapy can help you build your strength and heal from the surgery. It can also help you adjust to any differences in how your back moves after the surgery.
Spinal fusion surgery can help improve your quality of life. It can help ease pain and related symptoms like tingling or numbness in your arms or legs. Less pain means that you can spend more time doing the things you enjoy. Most people who have spinal fusion surgery are happy with the results.
Most of the possible risks and complications from spinal fusion surgery are similar to any surgery, including:
Spinal fusion surgery is also very close to your spinal cord and nerve roots, and involves reducing movement between certain bones in your spine. While rare, there are risks and complications, like:
Because of all these factors, your healthcare provider will talk and work closely with you to determine if spinal fusion is the best option for you.
Recovery from surgery is a gradual process. You’ll be able to resume many of your day-to-day activities within a few weeks after surgery. You’ll slowly resume light exercise and activities over the first few weeks. Depending on your job, you may be able to return in a few weeks to a few months. But getting the full rewards from spinal fusion surgery generally takes much longer. You’ll continue to notice benefits months after your surgery. Full recovery is normal, but it’s common for people to have reduced flexibility and movement because the fused vertebrae in their back no longer move like they did before.
Your healthcare provider will schedule follow-up visits after surgery, and you should see them as recommended. You should also see your provider if you experience changes in your symptoms, or if your symptoms continue to disrupt your life longer than expected (your provider can tell you how long you can expect symptoms to affect your lifestyle).
You should see your healthcare provider as soon as possible or seek medical attention if you have any symptoms of infection or serious nerve or spinal cord problems.
Infection symptoms include:
Nerve and spinal cord symptoms that need immediate care include:
Spinal fusion surgery is a serious medical procedure. Your provider will likely encourage you to try other treatments before surgery. That’s because the surgery may not be the only or best option.
But that doesn’t mean spinal fusion surgery is something to avoid. For many people, it’s the best option to treat ongoing back pain and back-related issues.
Some people can return to their life as it was after undergoing spinal fusion surgery, but some have limitations or life changes. The main reason for this is spinal fusion makes a part of your back less flexible than it used to be. That can reduce or stop some symptoms, but a loss of flexibility or movement for more extensive fusions is common and expected. Your healthcare provider can tell you what’s most likely to be the case for you if you undergo spinal fusion surgery.
Spinal fusion surgery itself isn’t painful, and anesthesia is a key part of managing pain during the procedure. But recovery from spinal fusion surgery can be painful. Your surgeon and other healthcare providers will work with you to manage your pain, but some amount of pain is common and expected as you recover.
If you have questions about how much pain to expect, talk to your provider. They can help you understand what you should expect vs. what needs further attention or treatment.
Spinal fusion surgery can be effective for years, but that can vary from person to person. Many different factors can affect how long this surgery can help. Some people need a follow-up surgery years later to re-fuse vertebrae or treat changes that happened over time after the first fusion surgery.
Spinal fusion surgery is a procedure that links two vertebrae in your back so that they no longer move independently of each other. This can stabilize your back structure and reduce symptoms like pain, numbness or weakness in body areas further down. But spinal fusion surgery isn’t a magic cure. Experts recommend it cautiously, and your provider will likely recommend other treatments first.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
The neurosurgery care team at Cleveland Clinic helps find solutions for your brain, spine and nerves — whether that means surgery or not.
