Dizziness is a common issue. If you have dizziness, you may feel woozy and disoriented. You may feel as if you’re about to lose your balance. Many things may make you dizzy, such as anxiety or a reaction to medication. But dizziness may be a symptom of an underlying medical issue. Talk to your healthcare provider if you’re having frequent or serious dizzy spells.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
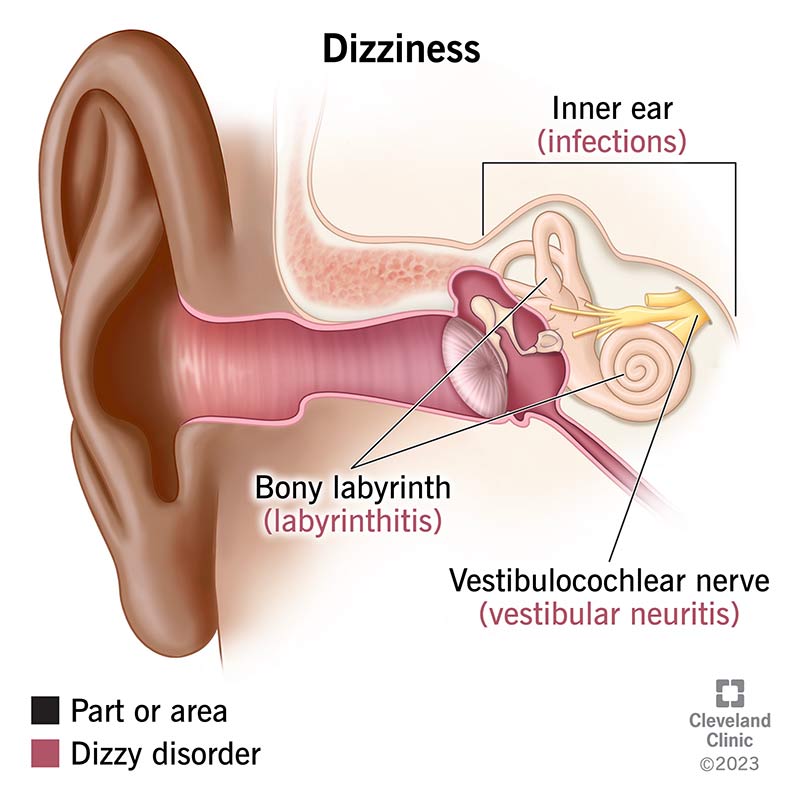
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/6422-dizziness)
Healthcare providers describe dizziness as having impaired or disturbed spatial orientation. You might describe dizziness as feeling woozy or light headed. You may feel as if you need to sit down before you fall down. Frequent or severe dizziness may affect your quality of life. People experience dizziness in different ways, including:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dizziness happens when something affects your sense of balance. A stable sense of balance requires a steady flow of information from your ears, eyes, tissues and central nervous system. Your central nervous system uses this information to tell your body how to maintain balance.
When something disrupts the flow, your central nervous system can process information incorrectly and you can feel unsteady and dizzy. Inner ear disorders, neurological conditions, medications and even stress may make you feel dizzy.
Advertisement
Medical conditions and other issues that may cause dizziness include:
Dizziness treatment depends on the cause. For example, if you’re dizzy because you have an inner ear infection, your healthcare provider will treat the infection. If you’re taking medications that make you feel dizzy, your provider may recommend you limit activities until your body adjusts to the medication. Some people benefit from a vestibular test battery to help determine if dizziness is due to an inner ear problem and vestibular rehabilitation therapy (VRT) to help treat the dizziness. Vestibular rehabilitation therapy involves exercises to manage dizziness symptoms.
No, but you can manage dizziness. If you’re feeling dizzy, lie down until dizziness passes. When you get up, be sure to move slowly and carefully.
Dizziness may not seem as if it’s a symptom of a serious issue, but you should still talk to a healthcare provider if you’re frequently dizzy:
Advertisement
The best way to prevent dizziness is to find out why you’re dizzy. For example, if you become dizzy when you’re dehydrated, you may prevent dizziness by drinking enough water. If you take blood pressure medication that makes you dizzy, your healthcare provider may prescribe a different medication or dosage. Unfortunately, you can’t predict or prevent all things that cause dizziness, such as a neurological disorder.
Talk to your provider if:
With vertigo, you have a sensation that you’re moving through space or your surroundings are spinning. Dizziness is an overall feeling of being unbalanced.
Everyone has dizzy spells — a sudden wooziness that comes and goes. But some people have severe or frequent dizziness that disrupts their daily lives. Talk to a healthcare provider if you often feel very dizzy. That way, you’ll know why you’re dizzy and what you can do to manage dizziness.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
