Hormonal IUDs are a type of birth control that use progestin to prevent pregnancy. An IUD is a T-shaped device that your provider inserts into your uterus. There are four types available in the U.S. They can offer between three and eight years of pregnancy protection.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
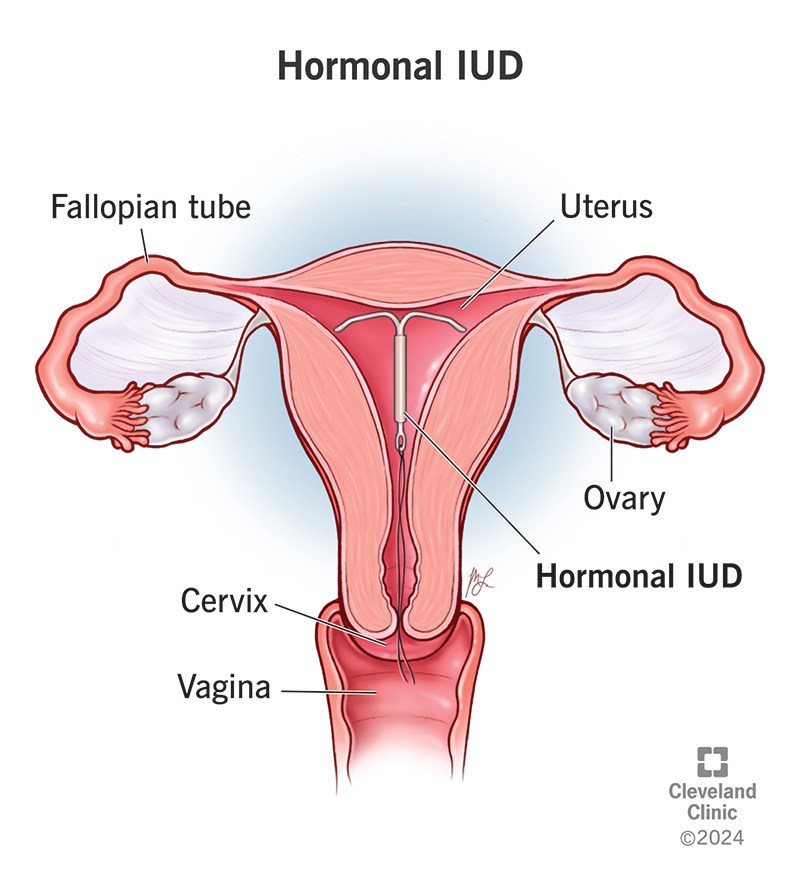
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/hormonal-iud-mirena)
A hormonal IUD (intrauterine device) is a small, T-shaped device a healthcare provider inserts into your vagina to prevent pregnancy. It’s a highly effective method of birth control that works by releasing small amounts of the hormone progestin into your body. A healthcare provider must insert an IUD for you, but once it’s in, it gives you continuous pregnancy protection for between three and eight years. That doesn’t mean you have to keep it in that long — you can have your provider remove it at any time.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are four types of hormonal IUDs available in the United States: Mirena®, Liletta®, Kyleena® and Skyla®. They all contain the same hormone (levonorgestrel), but they differ in how long you wear them. Other countries may have other hormonal IUD options available.
A hormonal IUD is a small piece of plastic shaped like a T. It has a short string on the end, which allows your provider to remove the IUD later. A hormonal IUD releases tiny amounts of progestin in your body. It prevents pregnancy in two ways:
Hormonal IUDs are more than 99% effective. Outside of abstinence (not having sex), IUDs are significantly more effective than most forms of birth control. This is mainly because there’s little to no room for error. After your healthcare provider puts it in, it works completely on its own without you having to think about it.
Advertisement
You can get an IUD at any point in your cycle. But if your provider inserts it more than seven days since the beginning of your last period, you should use a backup birth control (like a condom) for at least seven days. But, if it’s less than seven days since the beginning of your last period, you shouldn’t need a backup birth control at all.
The most common side effects happen during or shortly after your provider inserts the IUD. These effects tend to go away on their own. In the weeks following IUD placement, some people experience:
These side effects should subside after about three to six months. Although some people report not getting a period at all after they get a hormonal IUD.
Talk to your healthcare provider if you experience these or other side effects. It may be that this type of birth control doesn’t work for you. Your provider can help you find one that works better for your body.
There’s been a lot of research on this topic, but most studies show hormonal IUDs don’t cause weight gain.
There are many advantages to using hormonal IUDs for birth control. Some of those are:
While IUDs are safe for most people, they come with risks. Some possible complications are:
Advertisement
Additionally, some people shouldn’t get an IUD. This includes people who have:
Getting pregnant with an IUD is uncommon but possible. You should seek medical care if you have any reason to believe you may be pregnant when you have an IUD. Your healthcare provider will have you take a pregnancy test before placing your IUD.
There are several different kinds of hormonal IUDs to choose from. All of them work in the same way, but some last longer than others. If you’re interested in this type of birth control, talk to your healthcare provider about the pros and cons of each type, how they work and the possible side effects. While IUDs are over 99% in preventing pregnancy, they don’t offer any protection against STIs.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your birth control needs to work for you. At Cleveland Clinic, we help you find the right birth control option to fit your goals and lifestyle.
