Precordial catch syndrome is a sharp pain that appears without warning on the left side of your chest, near your heart. It’s not a medical emergency, but you may want to talk to a healthcare provider. Medical experts aren’t sure what causes it, but it often appears when you don’t sit or stand straight. It goes away within a few minutes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
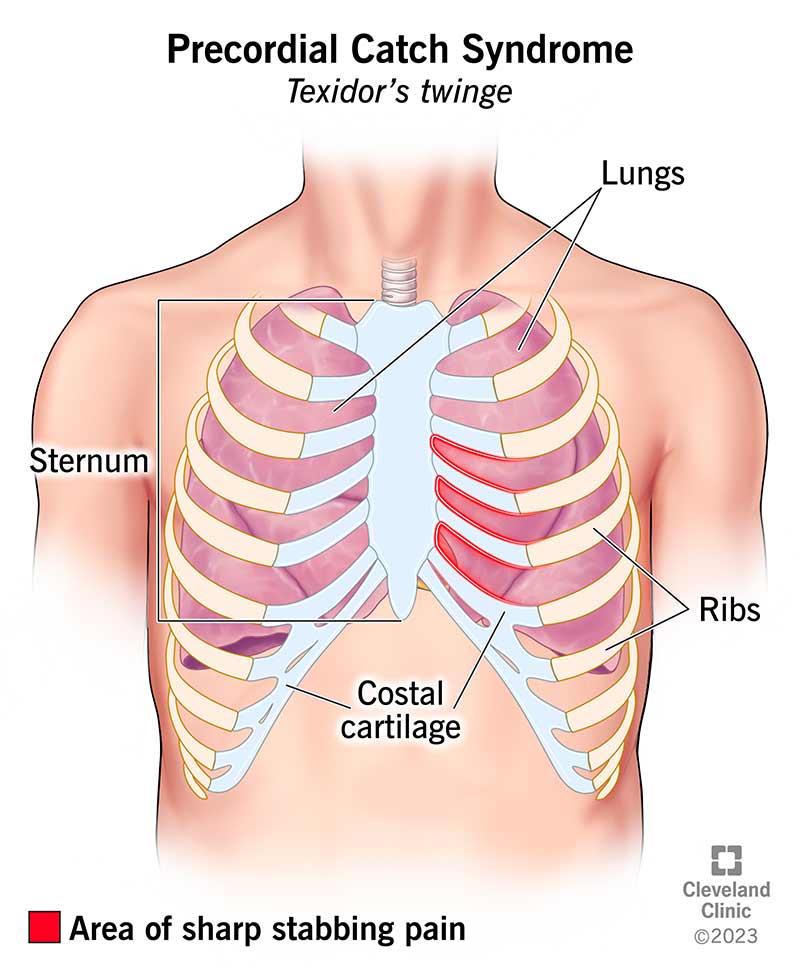
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/precordial-catch-syndrome.jpg)
Precordial catch syndrome is a short, sharp pain (“catch”) that suddenly appears in your chest, near your heart. “Precordial” means the pain relates to the precordium. The precordium is the area of your chest wall covering your heart.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The pain can be intense and extreme — it may feel like you’re getting stabbed by a sharp object — but it goes away quickly, doesn’t affect any other parts of your body and isn’t a symptom of a severe condition. You may experience the pain only once in your life, or it may appear occasionally.
Other names for precordial catch syndrome include:
No, precordial catch syndrome isn’t serious. It’s a common, harmless condition. There’s no association between precordial catch syndrome and heart or lung disease.
Precordial catch syndrome is common, especially in older children, teenagers and young adults.
The main symptom of precordial catch syndrome is a sharp, stabbing pain on the left side of your chest, usually just below the nipple. The characteristics of precordial catch syndrome pain include:
Advertisement
Medical experts aren’t sure what causes precordial catch syndrome. But they think it may be due to pinched nerves or muscle spasms in the lining around your lungs (pleura) or in your ribs or cartilage. Because it usually affects older children, teenagers and young adults, it may also be a side effect of a growth spurt.
Anyone can have precordial catch syndrome, but it most commonly affects children as young as 6 and young adults into their early 20s.
Precordial catch syndrome isn’t a dangerous condition, but complications can arise. These include:
A healthcare provider can diagnose precordial catch syndrome. They’ll ask about your symptoms, review your medical history and conduct a physical examination. During the physical exam, they’ll listen to your lungs and heartbeat with a stethoscope (auscultation). They’ll also check your chest for feelings of tenderness.
A provider can usually diagnose precordial catch syndrome through a physical exam. They’ll likely only order tests if you have other symptoms of conditions that may cause chest pain, such as a fever, cough or bruising, or if they hear any abnormal sounds while listening to your lungs and heartbeat. These tests may include:
Precordial catch syndrome pain stops after a short period. You can help relieve the pain by standing or sitting up straight and trying to relax while taking slow, shallow breaths. Some people report that taking a deep breath — even if it’s painful — helps the pain go away faster.
Precordial catch syndrome goes away, or the pain becomes less severe, in most people by the time they reach their early to mid-20s.
The outlook for people with precordial catch syndrome is extremely good. You may be able to help prevent pain by standing or sitting up straight. Most people outgrow it by the time they reach their 20s.
Healthcare providers aren’t sure if you can prevent precordial catch syndrome. Some people report they have fewer episodes if they remember to take deep breaths regularly and pay attention to their posture.
If you have precordial catch syndrome, the best way to take care of yourself is to sit or stand up straight, relax and focus on taking gentle, shallow breaths. Stretches or yoga poses that help open your chest muscles and counteract poor posture may also help. Making sure you drink enough water is also very important. In general, you can tell that you drink enough water if your urine (pee) is clear or very light yellow.
Advertisement
You can also take nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil®) or naproxen (Aleve®), to help relieve pain. But precordial catch syndrome pain usually disappears before an NSAID can take effect. Not everyone can take NSAIDs, so it’s a good idea to check with a healthcare provider.
Don’t ignore chest pain. It’s a good idea to see a healthcare provider if you have sharp pain in your chest, even if it goes away quickly and doesn’t affect any other part of your body. A healthcare provider can rule out other possible conditions.
Call 911 or go to the nearest emergency room if you have chest pain that lasts longer than five minutes, doesn’t go away when you rest or take medication or appears alongside other symptoms, including:
Advertisement
Costochondritis is a common, harmless condition that causes inflammation in the cartilage in your chest. Healthcare providers aren’t sure what causes it. But triggers may include rapid growth, coughing too hard, a bacterial infection, an injury or overexercising.
Costochondritis pain usually affects both sides of your upper chest, along the outside of your breastbone or sternum. But unlike precordial catch syndrome, the pain worsens when you touch the affected area. The pain can also last for several months.
It’s easy to assume the worst any time you have sharp, sudden chest pain, especially if it gets worse when you try to take deep breaths. But precordial catch syndrome isn’t dangerous. It goes away quickly, and most people outgrow it in their 20s. Talking to a healthcare provider for an official diagnosis can bring peace of mind.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
As your child grows, you need healthcare providers by your side to guide you through each step. Cleveland Clinic Children’s is there with care you can trust.
