Arthritis can affect any joint in your hands. It can make using and moving your affected fingers hard or painful. Signs of arthritis can include pain, stiffness or swelling. Most people can manage symptoms with nonsurgical treatments, like medication, physical therapy exercises, or wearing a splint or brace.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
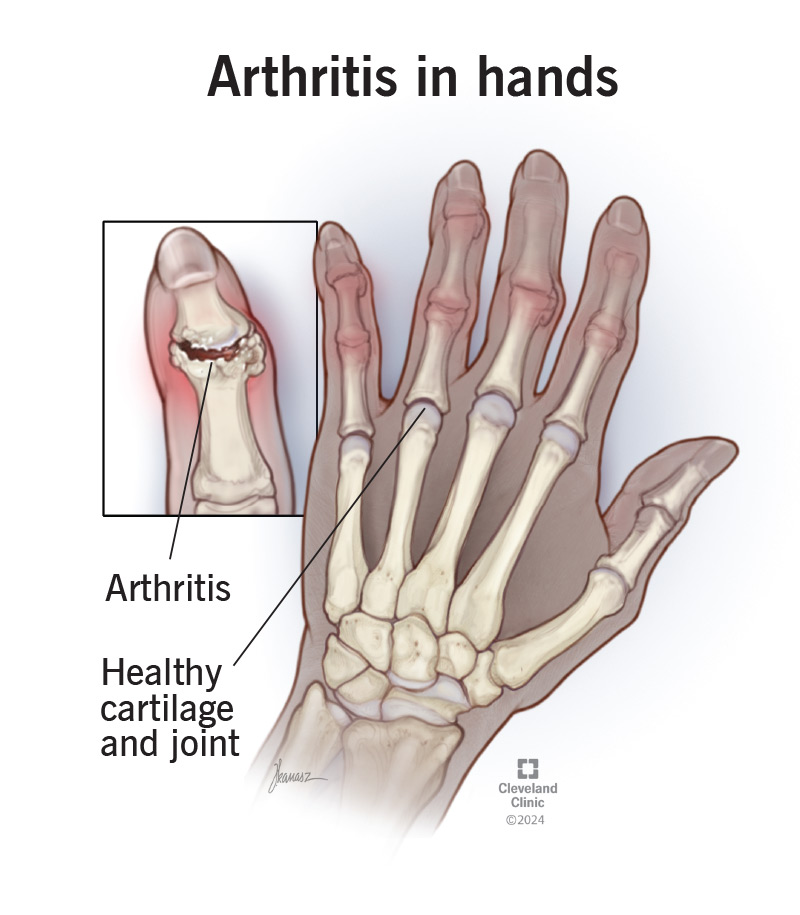
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/arthritis-in-hands)
Hand arthritis is any type of arthritis that affects the joints in your hands, fingers or thumbs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Arthritis damages the cartilage and other tissue in your joints. Once that cartilage wears down, your bones can rub together. This is what causes symptoms like pain, swelling and stiffness. You might not be able to use your hands as well as you used to as arthritis gets worse. It might be harder to manage everyday tasks.
Lots of people think arthritis is just an inevitable part of aging. And that can be true. But that doesn’t mean pain and stiffness in your hands is something you have to live with. Visit a healthcare provider if you think you might have arthritis in your hands. They’ll help you understand what’s causing the symptoms and which treatments will help manage them.
There are more than 100 different types of arthritis. Some of the common types that affect hands include:
The most common symptoms of arthritis in your hands include:
Advertisement
Everyone experiences pain differently. Hand arthritis pain may feel like a constant, dull ache in your joints. Some people feel sudden, sharp or stabbing pain, too.
When and how you experience symptoms depend on which type of hand arthritis you have. For example, osteoarthritis is more likely to cause symptoms with use or in the evening. Inflammatory arthritis (like rheumatoid arthritis) usually causes symptoms that are worse in the morning but improve with use.
Certain foods and drinks can trigger gout symptoms in episodes called flares. Eating or drinking things that can trigger gout may lead to a symptom flare.
Stress may also trigger some types of arthritis. Psoriatic arthritis and psoriasis can flare up when you’re feeling lots of stress.
The cause of arthritis in your hands usually depends on which type you have:
Anyone can develop arthritis in their hands. You may be more likely to if you:
A healthcare provider will diagnose arthritis in your hands with a physical exam and a hand X-ray. Tell your provider when you first noticed symptoms like pain and stiffness. Let them know if any activities or times of day make symptoms worse. The X-ray will show lost cartilage or changes in your bones.
You might also need blood tests. For example, your provider may check a sample of your blood for rheumatoid factor to help diagnose rheumatoid arthritis. They’ll check for high uric acid levels if they think you may have gout.
Your healthcare provider will suggest treatments to manage the symptoms you’re experiencing. Common treatments include:
Advertisement
Your provider will usually only suggest surgery for hand arthritis if nonsurgical treatments don’t help you feel better. Or if you’re still having severe symptoms after trying other treatments. The most common surgery types are:
Your provider or surgeon will tell you which type of surgery is best for you. They’ll give you a recovery timeline that’s customized to your unique needs.
Visit your healthcare provider if you experience any of the following symptoms:
There’s no cure for arthritis. But your healthcare provider will help you find treatments that manage the symptoms you experience and how often they affect you.
Some people with arthritis experience more severe symptoms as they age. Ask your provider how often you should have follow-up visits to check for changes in your joints.
Advertisement
Some types of hand arthritis happen naturally or because of health conditions you can’t control. So, there’s not always a way to prevent it. But you can lower your chances by:
We use our hands almost constantly every day. And it can feel like there’s a huge obstacle between you and your favorite activities if you’re dealing with pain and other hand arthritis symptoms. Even though arthritis usually takes a long time to develop, it might seem like you notice these signs all of a sudden.
Visit a healthcare provider as soon as it feels like your hands aren’t working as well as they used to. They’ll help you understand which type of arthritis you have and which treatments you’ll need to feel like yourself again.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
We diagnose and treat conditions that cause wrist pain and elbow pain. Learn how Cleveland Clinic experts use minimally invasive treatments to relieve your discomfort.
