Eczema on your face is a condition that makes your skin itchy, dry and flaky. Eczema prevents your skin’s protective barrier from functioning as it should, which can make your skin sensitive to irritants and allergens. There’s no cure for eczema on your face, but treatment is available to help your symptoms go away.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
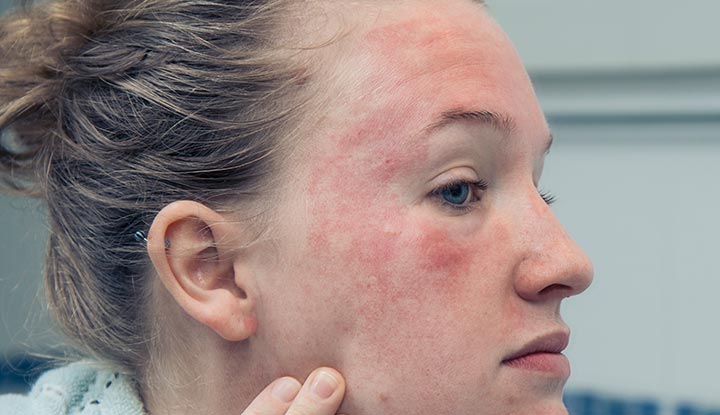
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24604-eczema-on-face)
Eczema on your face, or facial eczema, is a condition that can make the skin on your face dry, flaky and itchy. Eczema prevents your skin’s natural barrier from outside elements to function properly. This makes your skin sensitive, so it can easily react to irritants and allergens in your environment, which cause flares.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Several different types of eczema can form on your face. Some of the most common include:
It’s possible to have more than one type of eczema that can form on your body at one time.
Eczema on the face can affect anyone. It’s more common among people who have:
Women are more likely to get eczema.
Just over 10% of the United States population have a form of eczema, which equals about 1 in 10 people. Symptoms of eczema are unique to each person and can affect different locations on your body including your face.
Symptoms of eczema on your face range from mild to severe and include:
You’ll experience symptoms of facial eczema on your skin from your chin to your forehead. Your cheeks are the most common site where eczema on your face could appear.
Multiple factors cause eczema on your face, including:
Advertisement
Each person diagnosed with eczema on their face has unique triggers that cause their symptoms to flare up. Some of the most common triggers for eczema could include:
Eczema isn’t a contagious condition. You can’t pass eczema on your face to another person by physical or close contact.
To diagnose eczema on your face, your provider will examine your skin to look for signs of eczema like patches of dry skin and skin discoloration. If your symptoms look similar to other skin conditions, your provider will offer tests to confirm a diagnosis, rule out other conditions or determine the cause of your symptoms. Tests could include:
Treatment for eczema on your face is unique to your skin and what caused your flare-up. Treatment could include:
Before starting treatment with a new medication or drug, talk to your provider about the possible side effects, frequency and dosage of when you should take the medication to avoid interactions.
Advertisement
While there are multiple types of moisturizers available on the market, the kind of moisturizer, cream or cleanser that you choose can have an impact on how your skin heals or reacts.
Choose skin care products that:
Every person has unique qualities to their skin that react differently to skincare products. The moisturizer that works best for you might not work for someone else. If you’re unsure about what type of moisturizer to use on your skin, talk to your healthcare provider.
After treatment for a flare of eczema symptoms, it could take several weeks before your skin clears up completely. Treatment from your provider or dermatologist helps your symptoms go away faster. You can prevent future flares by avoiding irritants and allergens that caused your symptoms and using a moisturizer on your skin regularly to rehydrate your skin.
Eczema is a lifelong condition without a cure. Your symptoms can flare up on your face if you interact with environmental triggers like irritants and allergens. It takes several weeks before your symptoms go away, even with treatment.
Advertisement
Frequently apply unscented moisturizers designed to treat eczema to your skin throughout the day. The best times to apply moisturizer to your skin is in the morning when you wake up, every few hours to prevent dry skin throughout the day, after a bath or a shower when your skin is damp, and before you go to bed. Your provider might offer a medicated topical cream or ointment to treat your eczema during a flare.
Some people diagnosed with eczema on their face might experience low self-esteem, as their symptoms are visible on their skin when they enter social settings. It’s challenging to hide facial eczema because makeup can further irritate your skin and delay your healing time. If your eczema causes emotional distress or your symptoms get worse instead of better, contact your provider.
Yes, eczema on your face will go away, but it could take up to several weeks with treatment. Eczema is a chronic condition that can return to your face after it goes away. The best way to prevent a flare of eczema symptoms on your face is to avoid irritants and allergens and regularly moisturize your skin. If your eczema doesn’t seem to go away, talk to your provider about medication to treat your symptoms.
Advertisement
You can’t prevent all cases of eczema, but you can reduce your risk of flare-ups by:
Visit your healthcare provider if your symptoms get worse or don’t improve after several weeks. Talk to your provider if your skin reacts negatively to a moisturizer or topical medication, especially if it causes a rash or pain.
Eczema on your face is a chronic condition that can affect your skin throughout your life. The condition can flare up unexpectedly or happen if you interact with skin irritants and allergens. As eczema can affect your appearance, some people experience self-esteem concerns after a facial eczema diagnosis. Talk to your provider or a mental health professional if your skin affects your ability to thrive socially. To prevent future flares, use moisturizer regularly to keep your skin hydrated.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
