Dermatofibrosarcoma protuberans (DFSP) is a rare type of skin cancer that starts in your skin’s middle layer (the dermis). This cancer grows slowly and rarely spreads. But it can return after surgical treatment. It may start in areas that have skin damage from burns, scars or tattoos. Dermatologists perform Mohs surgery to treat DFSP.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
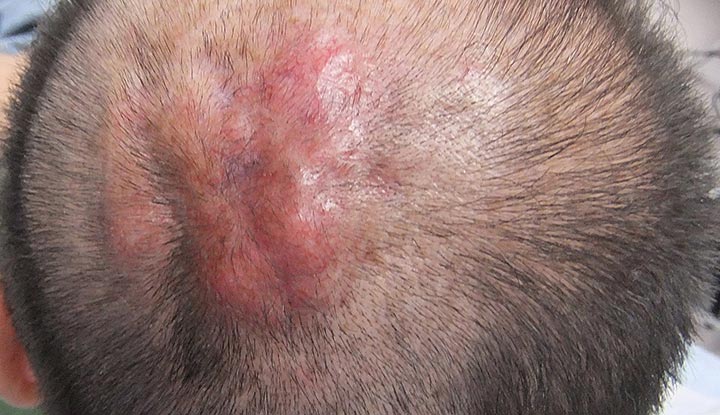
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24068-dermatofibrosarcoma-protuberans)
Dermatofibrosarcoma protuberans is a rare skin cancer that begins in your dermis, your skin’s middle layer. It’s pronounced “dur-MAT-toe-fy-bra-sar-CO-ma” “pro-TOO-bur-anz.” Your healthcare provider might call it DFSP.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This slow-growing cancer rarely spreads. Still, you need treatment to remove the tumor and prevent cancer from coming back (recurrence) or spreading (metastatic cancer). With proper treatment, DFSP has a high survival rate.
No. DFSP is a malignant (cancerous) soft tissue tumor and a type of skin cancer.
DFSP is a sarcoma (soft tissue tumor), cancer that develops in muscle, fat and skin. These tumors can also affect bones.
Cancer that spreads outside the original tumor is metastatic cancer. Approximately 1 in 20 people with DFSP experience cancer spread.
Metastatic DFSP is most likely to occur if you don’t get treatment or the cancer goes deep into fat and muscle.
For unknown reasons, DFSP can be more aggressive when it develops during pregnancy.
A small percentage of people with DFSP have an aggressive type called fibrosarcomatous dermatofibrosarcoma protuberans (DFSP-FS). These tumors are more likely to spread and come back after surgical removal.
DFSP is a rare cancer that affects approximately 4 out of 1 million people worldwide each year. They account for 1% to 6% of all soft tissue sarcomas.
The cancer typically affects adults ages 20 to 50, but children also get this skin cancer. Some infants have DFSP at birth. DFSP appears to affect people who are Black more often than people of other ethnicities.
Advertisement
Pathologists (doctors who examine bodies and body tissues) examine cells under a microscope to determine the type of DFSP. Types include:
As many as 9 in 10 people who develop DFSP have a gene change (mutation) that causes the condition. This gene change occurs in cells after you’re born. You don’t inherit a gene mutation from a parent that causes DFSP.
In addition to racial factors, a skin injury or scars may increase your risk of DFSP. Causes of skin injuries include:
Early symptoms of DFSP are easy to dismiss or not notice. The tumors typically appear on your chest, back, shoulders, abdomen or buttocks. Tumors can also form on your arms, legs, scalp and inside of your mouth.
At first, you may notice a small patch of skin that looks like a bruise. The spot is flat and painless. It may feel rough and look discolored.
In infants and children, DFSP can look like a birthmark. These spots are usually about 1/2 inch to 2 inches (1 centimeter to 5 centimeters) across.
DFSP symptoms become more noticeable as the cancer grows. The growing tumor pushes into the top layer of skin (epidermis). Firm lumps (nodules) of tissue appear on the skin (“protuberans”).
You may notice that the nodules are:
A noncancerous skin condition called cellular dermatofibroma can look like DFSP, especially during the cancer’s early stage. Cellular dermatofibromas are benign soft tissue tumors that typically appear on your legs. They may be itchy or painful. Most dermatofibromas don’t need treatment.
Dermatologists, medical doctors who specialize in skin cancer and skin diseases, diagnose DFSP. Your provider will perform a skin biopsy to remove part or all of the growth. Pathologists examine the tissue under a microscope to check for cancer cells.
Advertisement
If the skin biopsy determines you have DFSP, you may get an MRI to determine the size and depth of the tumor.
Surgical removal is the treatment of choice for DFSP. Dermatologists perform Mohs surgery to remove DFSP tumors. During the procedure, your provider:
DFSP tumors can grow back after surgical removal. 20% to 30% or more of people experience a recurrence of DFSP within three years after wide excision, and up to 4% to 5% recur after Mohs surgery. But tumors can recur for 10 years or more.
Healthcare providers use imatinib to treat metastatic DFSP or tumors that are too large or difficult to surgically remove. Imatinib can also shrink the tumor, making surgical removal possible. Radiation treatment can be done for incompletely excised DFSP or inoperable DFSP.
Advertisement
With proper treatment, more than 99% of people with this nonaggressive, slow-growing cancer live 10 years or longer.
These steps may improve your outlook:
You should call your healthcare provider if you notice new skin changes, such as:
You may want to ask your healthcare provider:
Many skin changes are harmless. But some changes can indicate skin cancer or another skin disease that requires treatment. You should contact your healthcare provider whenever you notice changes to your skin. Dermatofibrosarcoma protuberans (DFSP) is a rare skin cancer that’s unlikely to spread. Still, you need surgical treatment to keep the tumors from spreading. A prompt diagnosis and treatment are critical to improving your outlook.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.