Urethritis is a common condition that causes inflammation in your urethra. Infections are the most common cause of urethritis. But you can also get it from irritants or trauma. Treatment usually includes antibiotics.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
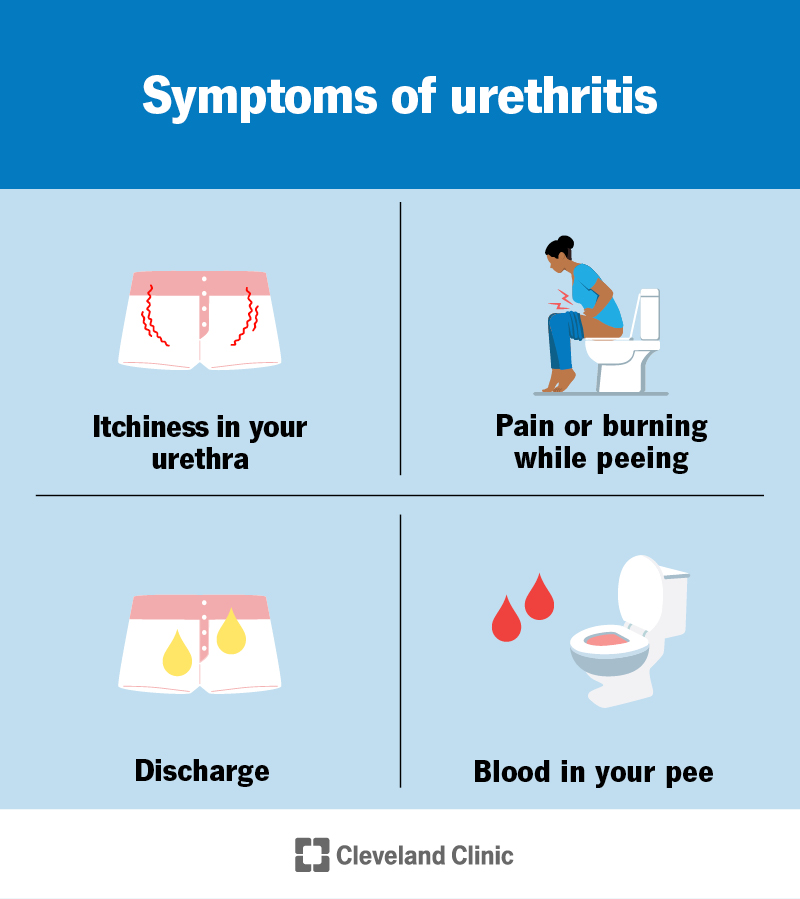
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/urethritis)
Urethritis (yoor-uh-THRI-tis) is inflammation in your urethra. Your urethra is the tube that takes pee from your urinary bladder to the outside of your body. Typically, a bacterial infection causes urethritis. Sexually transmitted infections (STIs) are the most common type of infections that cause it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Urethritis is common. Anyone can get it. About 4 million people in the U.S. get it each year. And throughout the world, around 151 million people get it annually. These numbers may be low. It’s possible to have urethritis without having any symptoms (asymptomatic).
The different types of urethritis include:
Signs and symptoms of urethritis include:
Pus, blood or a cloudy yellow or white fluid (discharge) may leak from the tip of your penis. You may also have blood in your semen (hematospermia).
STIs are a common cause of urethritis. Besides gonorrhea, other STIs that can cause urethritis include:
Advertisement
Other urethritis causes include:
Not always. But urinary tract infections (UTIs) can sometimes cause urethritis.
Urethritis itself isn’t contagious. But the infections that cause it can be contagious. If an STI causes urethritis, you should get treatment for it as soon as possible. Anyone else you have sexual intercourse with should also get treatment. If only one person gets treatment, you may keep passing the STI to each other.
You’re more likely to get urethritis if you:
Without treatment, urethritis can spread and affect other parts of your urinary system and male or female reproductive systems. You’re at a greater risk of:
It can also cause:
A healthcare provider will review your medical history and ask you questions about your symptoms and sexual history. They’ll also perform a physical exam of your genitals (which may include a digital rectal exam for males and a pelvic exam for females).
They’ll also recommend tests, like:
These tests help confirm a urethritis diagnosis. They also help find out if a certain type of infection is the cause.
Antibiotics are the main treatment for urethritis. You may only need one antibiotic, or you may need a combination of different ones. Antibiotics that healthcare providers commonly prescribe to treat urethritis include:
If they believe you have an infection, your provider may start you on antibiotics even before getting your test results back. They may also suggest taking a pain reliever.
Advertisement
For most infectious causes, no. But for some noninfectious causes, it may go away on its own. Your healthcare provider may recommend that you:
You should start to feel better a few days after taking antibiotics. Usually, you’ll need to take the medications for a week to 10 days.
Call a healthcare provider if you have symptoms of urethritis. Contact them again if you’ve already started treatment and:
They may recommend additional tests or prescribe a different antibiotic.
During your appointment, you may wish to ask the following questions:
With proper diagnosis and treatment, the prognosis for urethritis is good. Make sure to take all your medicine, even if you feel better. If you don’t finish your full course of antibiotics, the infection may come back and be harder to treat.
Advertisement
Tell your sexual partner(s) if you have urethritis. They must also take antibiotics. If only one of you receives treatment, you can pass the infection back and forth to each other.
Avoid having sexual intercourse until you and your partner(s) receive treatment and no longer have symptoms.
If you have urethritis, you can help relieve discomfort and pain by:
You can help lower your risk of developing urethritis by:
It can be tough talking about your private areas. But if you’re having unprotected sexual intercourse and develop urethritis symptoms, you should make an appointment with a healthcare provider. They’ll ask questions about your sex life, which may feel uncomfortable. But a provider’s job is to help, not to judge. Be honest with them about your sexual activity so they can provide the best diagnosis and treatment. And if you have urethritis, tell your partner(s) so they can get treatment and avoid giving it back to you or spreading it to others.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
